Garcinia Cambogia Side Effects: How Garcinia Cambogia Extract Fosters Diabetes

Garcinia cambogia side effects are said to be few and of minor
significance, according to the marketers of the diet pill. Instead, the
general public is predominately exposed to claims of garcinia cambogia
benefits, centering around the weight loss supplement's purported
capability to confer quick fat loss.
However, an eligible body of scientific evidence unravels notable diabetes-mediating garcinia side effects –some of them closely resemble the documented diabetes-nourishing statins' side effects ("statins" are very popular cholesterol-lowering medications).
The arguably greatest personal challenge in corporate cultures is the discovery of the real truth about a seemingly endless list of things.
The difficult task applies to and engulfs politics, economics, science, mainstream medicine, or other commercialized entities such as the weight loss industry. The example investigated here, with garcinia cambogia extract (GCE) out of the weight loss supplement industry, authenticates the soundness of this general pattern.
(Note: I have intentionally repeated certain critical points throughout the lengthy article to facilitate and improve understanding of the rather complex information presented in this report.)
(An aside: I've written a highly shortened exclusive version of this report for greenmedinfo.com, "The World's Largest, Open Access, Natural Medicine Database". A link to that article, entitled "Does A Popular Dr. Oz-Endorsed Diet Supplement Promote Diabetes?" can be found and accessed by visiting "List Of My Off-Site Articles" under the 'Articles' link icon at the top of every webpage of rolf-hefti.com.)
What Is Garcinia Cambogia?
–Dr. Oz, Health Product Advertisements, And The Marketing Of Garcinia Cambogia Extract For Diabetes
"Journalism works with the five W’s and one H: Who? Where? When? What? Why? and How? Investigative journalism adds a crucial seventh question: Is it true?" (Helke Ferrie, Medical Researcher & Author)
Garcinia cambogia (GC) is a fruit. The garcinia cambogia fruit is also known by the names of malabar tamarind, gambooge, kukum, brindleberry, and bitter kola [3], or kudam puli and garcinia gummi-gutta. Typically, garcinia nutritional diet supplements contain a botanical extract derived from the rind of the fruit. Supplements of garcinia cambogia extract usually consist of concentrated amounts of one of the alleged main "active" or essential elements in garcinia cambogia's rind, hydroxycitric acid (HCA) or hydroxycitrate, a chemical related to citric acid [2,3]. (On occasion, some people had mistakenly referred to the natural weight loss supplement as cambogia garcinia.)
HCA garcinia cambogia extract has been most famously advertised by the highly popular medical authority and celebrity doctor Mehmet Oz, MD (widely known as "Dr. Oz" or "Doctor Oz"), at his popular TV show ("The Dr. Oz Show") and the Doctor Oz website, beginning in 2012, as the "holy grail" of weight loss management, a "fat buster", and a "breakthrough in natural weight-loss", portraying it as a safe effective natural diet supplement [1]. Doctor Oz has habitually dispensed various weight loss tips on his award-winning television show.
The popularity of garcinia cambogia weight loss supplements soared after their public endorsement by idolized television advice guru Doctor Oz, and many marketers began claiming that this slimming aid is one of the best diet supplements. A phenomenon that has been called the "Dr. Oz effect" (a spin-off of a broader term, the "celebrity effect"), prompting many people with weight issues to take garcinia cambogia extract, especially as the natural diet pill promised to offer rapid weight loss.
The most popular, top-selling garcinia weight loss supplement in the US has been "Hydroxycut", that contains a proprietary botanical mixture of the plant (called "Super Citrimax", "CitriMax", or "Citrin") and other ingredients. Unfortunately, the ingestion of certain ephedra/ephedrine-free garcinia products of the alleged supreme garcinia cambogia brand Hydroxycut had been linked to several cases of liver damage, rhabdomyolysis (a serious muscle disorder), and other toxicities [4,5]. As one might expect, this has caused some people to ask, “is garcinia cambogia safe?”
Reading through the marketing messages of the (online) promoters and sellers of garcinia diet pills and websites with (fake) garcinia cambogia reviews (most of which are sites selling GCE with enticing promises such as “the best garcinia cambogia pills”), one of their typical main claims is –apart from that it is one of the best diet pills to buy– that the diet product has no major side effects or that it is one of the "safest dietary supplements available on the market".
For the most part, purportedly highly credible and highly authoritative medical websites (e.g., WebMD.com, an online representation of the orthodox medicine business monopoly) and nutrition websites make similar bold assertions about the general lack of (severe) garcinia cambogia side effects.
Besides the advertising claims that GCE-HCA products are safe diet pills and natural agents of fast weight loss (or weight control), you can even find research studies on garcinia cambogia side effects and benefits in the medical literature, that state, "it cannot be concluded that Garcinia/HCA is unsafe" [6], as denoted in one such paper. Although, no data presented in that same review study [6] rated that garcinia-cambogia supplements are safe in meaningful long-term studies, lasting at least two years, whether in animals nor humans.
The commercial marketing of certain plants and herbs for obesity (e.g., garcinia cambogia for weight loss) has experienced an expansion to affiliated health conditions. Some research investigators had proposed a number of physiological mechanisms that could explain how plant compounds can have benefits for diabetics, such as:
- via the stimulation of insulin release,
- a reduction of intestinal glucose absorption, or
- by way of an augmentation of glycogen synthesis (=production of glucose stores in the liver and muscles, technically termed gluconeogenesis or neoglucogenesis) [7].
Among the topics and claims of herbal medicine for diabetes (e.g., cinnamon for diabetes) and means to cure diabetes naturally, a positive relationship between garcinia cambogia and diabetes has also been intimated. The list of projected garcinia cambogia benefits includes the assertions that the extract supposedly (among other declarations) "reduces cravings for sweets and enhances the effectiveness of the body's own insulin", "allows the muscles of the body to absorb more glucose" and garcinia diet supplements "also bind up leftover glucose in the bloodstream" [8].
In rats, for instance, hydroxycitric acid-garcinia cambogia extract delayed glucose absorption in the small intestine while all of the supplied glucose eventually still got absorbed over the feeding period [9]. Other garcinia cambogia studies with laboratory animals found that HCA-garcinia cambogia products have the capacity to somewhat improve a physiological hallmark of diabetes mellitus, namely oxidative stress insults to the body [10].
In response to such research propositions and findings, some promoters and vendors of herbal weight loss and garcinia cambogia products have also begun to recommend the (adjuvant) use of garcinia diet supplements in approaches of diabetes mellitus treatment (and the prevention of diabetes). In the classic garcinia cambogia episode of the Dr. Oz TV Show mentioned above, potential garcinia cambogia benefits for diabetics were also commented on (apart from other merits) by one of his guests who was promoting the value of the fat-burning diet pill, prompting Doctor Oz to exclaim about GCE that "in many ways it's the holy grail" [1].
Yet contrary to this interpretative framework, a rather thorough perusal of the medical evidence strongly supports the perspective that numerous garcinia cambogia side effects have diabetes-promoting activities. Hence, the popular claims that there are no major garcinia cambogia side effects, and that the natural diet supplement is very safe and ought be tallied among diabetes herbal remedies or botanical modalities are untrue.
Furthermore, what is of broader significance (as described and cited in this article) is that in juxtaposition to the common misleading or false rhetoric and hype about "miracle" garcinia cambogia products and minimal garcinia cambogia side effects, there is, in spades, plenty of misleading or false rhetoric and hype by the conventional medical business (the medical profession) about its various "wonder" products and services, and an underemphasis about their harms.
What Is Diabetes Mellitus, What Are The Symptoms Of Diabetes Type 2?
"The physiologic control of glucose homeostasis results from a balance between hepatic glucose release (glycogenolysis and gluconeogenesis) and dietary glucose absorption versus skeletal muscle and adipose tissue glucose uptake and disposal. Disruption of this delicate balance either through defects in insulin secretion, liver glucose output, or peripheral tissue glucose uptake results in pathophysiological states of insulin resistance and diabetes." (Makoto Kanzaki, PhD & Jeffrey E. Pessin, PhD, Diabetes Researchers) [11]
The pathophysiology of diabetes mellitus, the most typical diabetic symptoms, or the warning signs of diabetes type 2 are:
- high blood sugar –routinely referred to as hyperglycemia (traditionally, diabetes was called the "sugar disease")– and high amounts of sugar in the urine (glycosuria) with corresponding frequent urination to get rid of the sugar surplus (thus, diabetes is viewed as a "wasting disease"),
- abnormal tissue response to normal insulin concentrations (insulin resistance),
- defective insulin secretion from the pancreas,
- mitochondrial dysfunction in some body tissues,
- pancreatic beta cell dysfunction or destruction,
- elevated fat content in the blood stream (hyperlipidemia), and
- increased oxidative stress (including in the brain) and chronic inflammation [13-22].
By and large, these well-characterized biological modifications define diabetes.
Type 2 diabetes mellitus (formerly called non–insulin-dependent diabetes mellitus or adult-onset diabetes), is much more prevalent than type 1 diabetes mellitus (traditionally referred to as insulin-dependent diabetes mellitus) [12].
As far as diabetes and weight loss diet pills concern, garcinia cambogia side effects sustain, foster, or aggravate, more or less, all of these clinical manifestations of diabetes through various (overlying) physiological mechanisms –independent from the consumption of either an adulterated or pure garcinia cambogia extract.
What Causes Diabetes Mellitus?
–The Principal Clinical Features Of Diabetes: Injury To The Pancreas & The Brain
“Science consists in grouping facts so that general laws or conclusions may be drawn from them.” (Charles Darwin, 1809-1882, Naturalist & Originator of the Theory of Evolution)
How is diabetes caused? Over a century ago it had been observed that hemochromatosis, a disorder where iron accumulates in tissues (leading to iron overload), has the capacity to destroy pancreatic ß-cells (beta-cells) which can result in diabetes mellitus [23,24]. Iron carries a high inflammatory potential, particularly at higher doses, as a generating source of injurious reactive oxygen species (ROS), also known as free radicals [25-27].
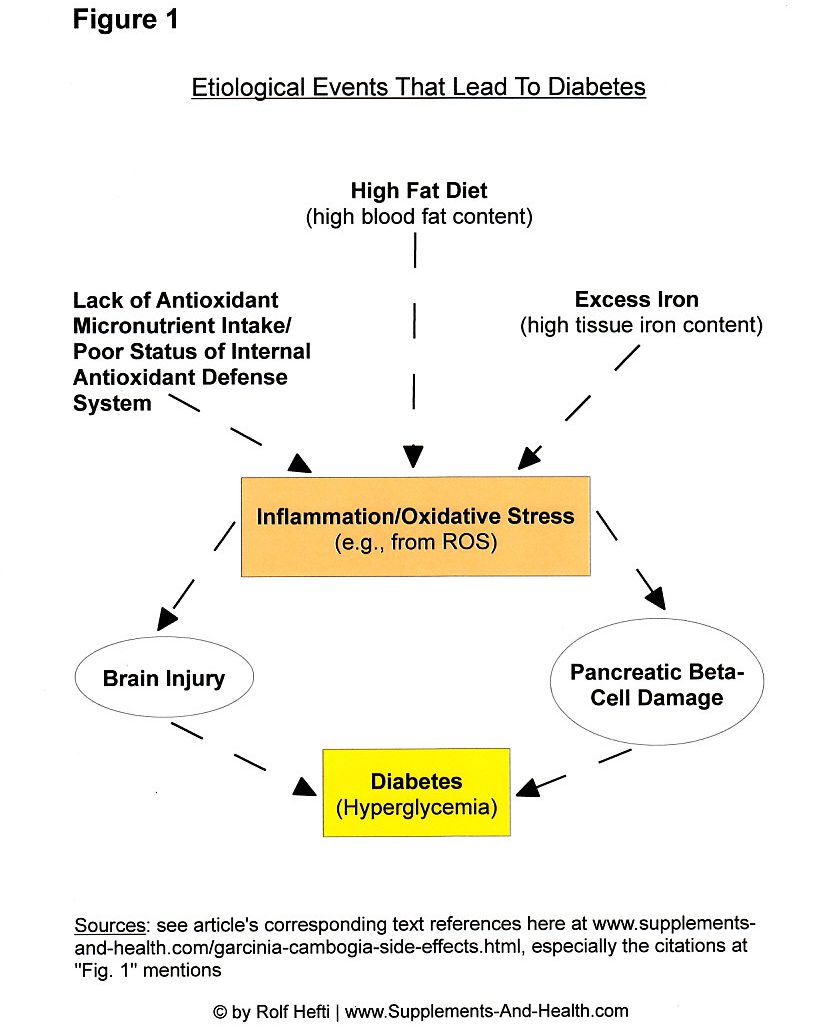
Much pertinent research over the ensuing years has corroborated the diabetes-pancreas link. Specifically, that the killing or dysfunction of pancreatic insulin-secreting beta cells (from the islets of Langerhans), producing a pancreatic insulin deficiency, is among the prime contributors or causes of diabetes mellitus (the etiology of diabetes) [13,16,18,20,28] –in both diabetes type 1 and 2 [29] (see Figure 1; "Figure" is abbreviated hereafter to "Fig."). Almost all new cases of diabetes, for example, carry beta cell antibodies, indicative of some irritating or harmful influence upon the pancreatic gland [30], or an overactive immune system. This lends support to the view of diabetes as a manifestation of a chronic (low-grade) inflammatory syndrome [322,323,336].
(Speaking of inflammatory injury to the pancreas, in another article of mine on L-tryptophan, 5-HTP, and serotonin, with the title "Tryptophan Side Effects: L-Tryptophan Is Far From Harmless" (direct link to it at the end of this article under Recommended next pages), I mentioned that certain inflammatory tryptophan metabolites, derived from pure tryptophan supplements, can orchestrate a degenerative-diabetogenic influence on the pancreas such as in the production of fibrosis.)
Diabetics, or obese individuals, often suffer from hyperlipidemia, or high blood fat content [31-34]. Fats are susceptible to free radical attacks, especially the long-chain polyunsaturated fatty acids (PUFAs), such as linoleic acid, EPA, or DHA, because of their multiple "exposed" (unoccupied) molecular double carbon bonds, creating a variety of harmful inflammatory chemicals [26,27].
Systemic fatty acid excess (hyperlipidema) results in injury to the brain. A high fat diet (of refined processed foods) –including
the high intake of PUFAs, such as the purported "essential fats" (EFAs) linoleic acid and linolenic acid, also known as "vitamin F" or informally referred to as omega-6 fatty acids and omega-3 fats (alongside an inadequate supply of antioxidants [35,36])– induces an increase of inflammation and oxidative stress in the brain, leading to neuron injury and loss of certain cerebral regions (such as in the hypothalamus) that govern metabolism, glucose control, and energy homeostasis [22,37-39]. And, a high fat diet (of refined goods) can also destroy the insulin-producing cells in the endocrine pancreas (beta-cell apoptosis) via inflammatory events [336] (see Fig. 1).
Garcinia Cambogia Side Effects: The Promotion Of Hyperglycemia (High Blood Sugar Level)
–What Causes Hyperglycemia? Sugar, Or Maybe Not?
"When hundreds all believe the same thing there is danger. It becomes unassailable. The contagion factor gives it more power." (Arthur Janov, PhD, 1924-2017, Psychologist, Academic Hall of Fame)
Since the 1930s and 40s (and subsequent decades) many good research experiments had demonstrated that stressors of all sorts (e.g., chemical toxins, physical insults, psychological traumas) regularly raise adrenaline and other catabolic stress hormones of the glucocorticoids/corticosteroids family such as cortisol [40,41].
Catabolic hormones, such as cortisol or the catecholamines (adrenaline, noradrenaline), trigger the release of fat stores (adipose lipolysis) into the blood [42-44] and signal the release of glucagon (from pancreatic islet alpha-cells).
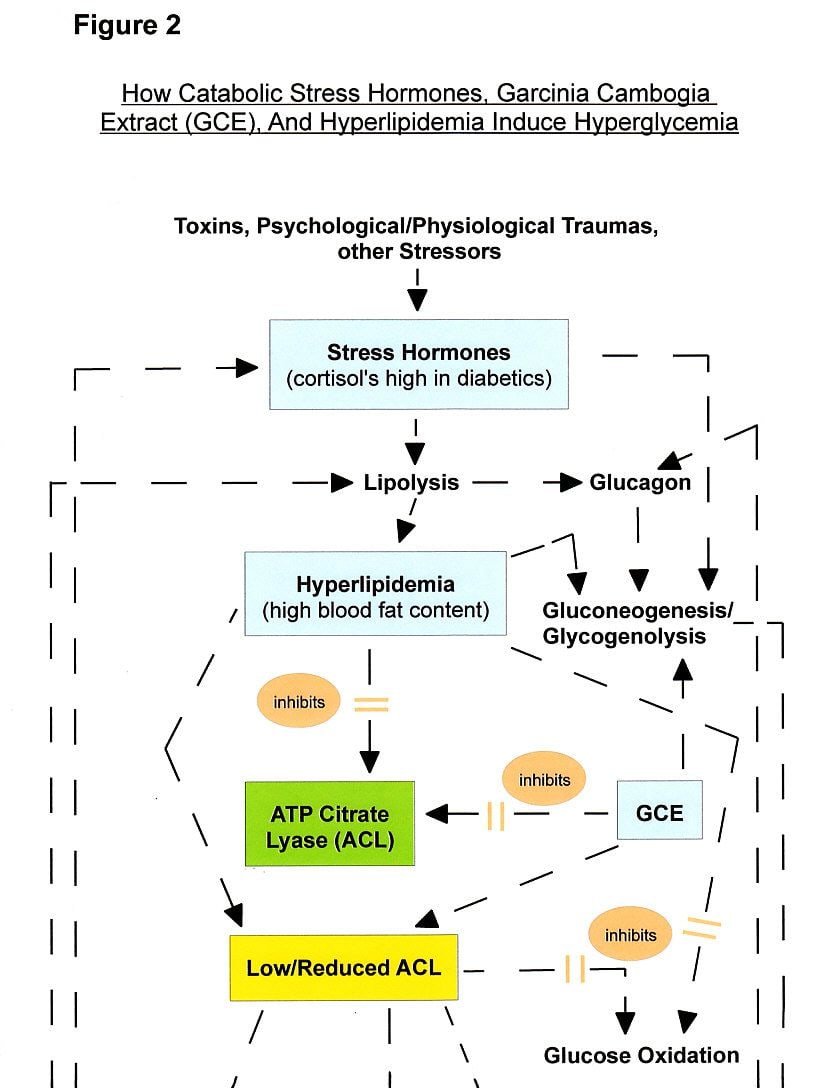
Glucagon, too, gets activated by low blood sugar states (hypoglycemia) or an insulin deficit, and glucagon is a hormone responsible for raising the sugar content in the blood via (1) the induction of endogenous glucose production in the liver (=gluconeogenesis) and (2) the mobilization of liver glycogen stores (=glycogenolysis; glycogen is a storage form of glucose that some individuals had called "body starch") into the blood stream [45-47] (see Fig. 2).
And, (excess) free fatty acids in the blood are also glucogenic (akin to certain amino acids), activating gluconeogenesis and glycogenolysis [15,47], and raise the level of "sugar" (i.e., glucose) in the blood, conceivably as an adaptive maneuver to marshal the ideal fuel for cell metabolism, glucose.
But while stress hormone-mediated lipolysis, resulting in excessive blood fat concentration, enhances glucagon/lipid-induced (hepatic) glucose production (gluconeogenesis/glycogen synthesis) and its breakdown and release into the blood (glycogenolysis), raising blood glucose content, it suppresses glucose utilization by the body [48-50], creating an deficit of glucose inside of cells (neuroglucopenia, neuroglycopenia or intracellular glycopenia) and a glucose excess (hyperglycemia) in the blood stream, respectively [19].
In terms of diabetes and blood sugar level, both animal and human experiments rather convincingly indicated that hyperglycemia is primarily the result of "excessive glucose production via gluconeogenesis" (in the liver) and glucagon-mediated glycogenolysis –incited by free fatty acid mobilization (a.k.a lipolysis) or an insulin deficit– rather than the outcome of insulin resistance (i.e., insulin receptor dysfunction), an idea that has been most commonly postulated [47,49-53] (see Fig. 2).
"Enhanced lipolysis" and "overproduction of glucose" (excessive gluconeogenesis) are prominent characteristics of diabetes mellitus type 2 (T2DM) [15,54] and major events why in diabetes blood sugar levels are customarily high. So, high blood cortisol and high fat levels might be among the more meaningful signs and symptoms of hyperglycemia rather than insulin resistance.
For the most part, gluconeogenesis entails the production of glucose from protein breakdown (proteolysis) [47]. A transitory hypoglycemic state (just like a variety of stressors) adaptively recruits catabolic stress hormones, such as the classical glucocorticoid cortisol [55], which raise the blood sugar value by cannibalizing body tissues (protein wasting) and turning them into glucose in the process of gluconeogenesis. To limit protein loss and, thus, the catabolic decay of the body structure, stress hormones concomitantly also trigger lipolysis [47].
In diabetes, cortisol levels are increased, spurring the production of glucose in the liver [56]. And, as expected, diabetics have an up-regulated hepatic production of glucose [51,56]. This physiological state of elevated glucose production gets intensified by the administration of supplemental garcinia cambogia extract (containing HCA) because hydroxycitric acid-garcinia cambogia, like fatty acids from lipolysis or from a high-fat diet [50,53], activates liver gluconeogenesis [54,57,58] (see Fig. 2). (Diverging from this hyperglycemia-fostering action of garcinia cambogia extract, strangely, the most authoritative orthodox medical websites I've looked at uniformly claimed, by and large, in 2014/2015 when I originally worked on this report, that among the potential garcinia cambogia side effects is the diet supplement's potential to dangerously lower blood sugar levels (in conjunction with drug treatment for diabetes), apparently based on a single study with mice.)
While plasma cortisol concentration is elevated in diabetics, promoting hyperglycemia, their blood content of thyroid hormones, such as the active thyroid hormone triiodothyronine (T3) and its less operational precursor thyroid hormone, thyroxine (T4), are reduced [56].
T3 promotes glucose uptake and its metabolic clearance (glucose oxidation or "sugar burning"), whereas a loss of T3 enables and augments the accumulation of blood glucose, contributing to sustained hyperglycemia [56] and hypothyroidism [59] (see Fig. 2). Low thyroid function, especially low T3 blood concentration, therefore, should be tabulated among potential hyperglycemia symptoms or predictors. Cell energy atrophy, such as from a T3 deficit, engages iron, increasing its concentration and activity, and leads to lipid peroxidation-mediated tissue injury [59] (see Fig. 2).
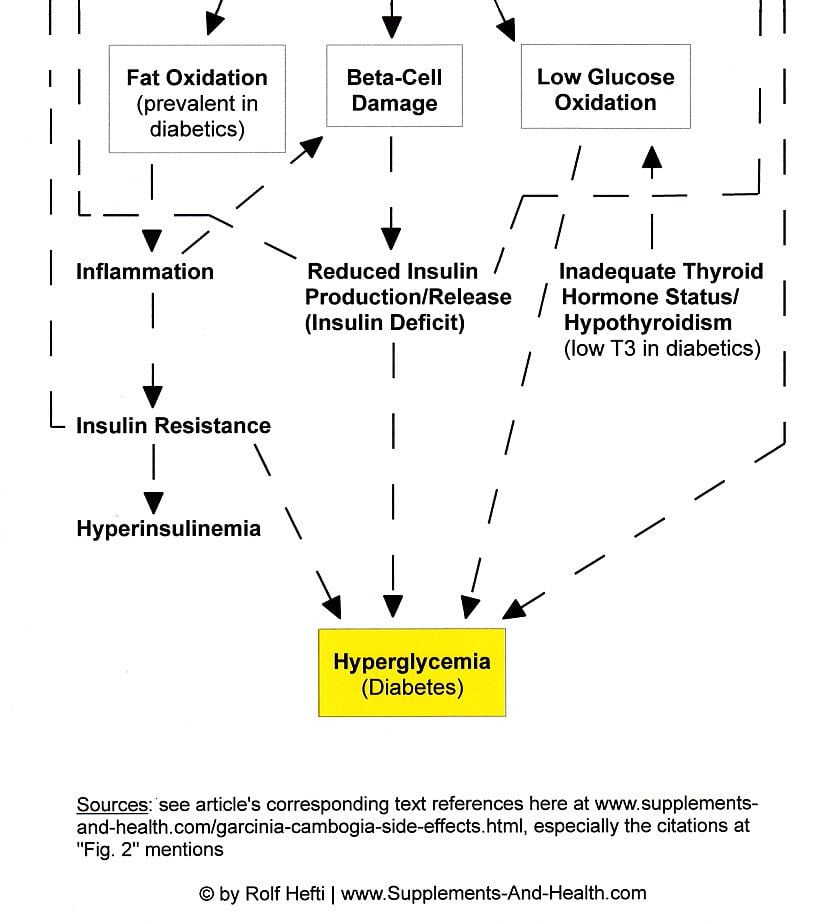
Therefore, diabetic hyperglycemia is thought to be a consequence of:
- a stress-hormone/insulin deficiency-incited overproduction of sugar in the liver (gluconeogenesis) and its secretion into the blood (glycogenolysis),
- a pancreatic insulin deficiency, triggering also gluconeogenesis and glycogenolysis, in addition to lipolysis,
- thyroid dysfunction (a key element of the metabolic syndrome) that hampers carbohydrate oxidation, and
- a higher level of free fatty acids (FFA, also known as non-esterified fatty acids or NEFA) in the blood (hyperlipidemia) –turning on internal glucose synthesis (hepatic gluconeogenesis) and inhibiting cellular glucose use– induced by (stress hormone-mediated) adipose lipolysis or eating a lot of (refined) fatty food (obese individuals and people with diabetes tend to have higher blood fat levels compared to healthy people) [15,33,47,56,59-63].
All of the above physiological mechanisms are complexly interrelated (see Fig. 2).
Despite of these well-documented physiological processes, the popular sentiment in the culture and health care system today in the early years of the 21st century is –and has long been– that "sugar is toxic" (or “carbs are bad”) and that dietary "sugar causes diabetes", painting the substance as the direct fundamental culprit or cause of hyperglycemia rather than seeing hyperglycemia as a component of a syndrome or a symptom of diabetes relatively independent from, or indirectly related to, dietary sugar consumption. So the demonization of simple sugars has been systematic and overwhelming because it is a notion pushed by both conventional and unconventional natural medicine.
The primary physiological processes accredited for hyperlipidemia-induced hyperglycemia are:
- fats in the blood, whether sourced from lipolyis or a high fat diet (of refined foods), block the cells' insulin-activated glucose uptake [60,64,65] and the use of glucose as a fuel material, privileging oxidative fat combustion instead [15,60,65-67], repressive events that end up raising the blood sugar value (see Fig. 3). This means that a higher blood fat content (e.g., from lipolysis) promotes the cellular uptake and burning of fats [68,69]. A shared obesity and diabetes symptom is that individual afflicted with these conditions burn long-chain fatty acids (e.g., polyunsaturated fats/PUFAs and certain saturated fats) preferentially over sugar and burn fats at a higher rate than lean individuals [14,32,63,70].
- some long-chain fats (certain saturated fatty acids and certain polyunsaturated fatty acids/PUFAs) in the blood decrease and disable the adenosine triphosphate citrate lyase protein (ATP citrate lyase, ACL, ACLY, or ATP-CL, also known as citrate cleavage enzyme), thereby inducing damage and programed cell death (apoptosis) in pancreatic insulin-producing beta-cells (after the lipids have accumulated and been consumed as metabolic fuel in pancreatic islets which is known as the "lipotoxicity hypothesis") [15,20,71-79] (see Fig. 2). (Insulin is the basic hormone responsible for blood sugar control [11,47,80].) This parallels the evidence that a high fat diet (of processed foods) is associated with apoptotic brain cell loss and diabetogenic effects via the hypothalamic-pancreatic axis [37-39,81] (see Fig. 1).
Now, how does garcinia cambogia work? What are the primary physiological effects of GCE?
Garcinia cambogia diet supplements' main ingredient, hydroxycitric acid (HCA), inhibits the lipogenic ATP citrate lyase (ACL) enzyme [2,54,57,58,82-85]. Increased sugar production in the liver (neoglucogenesis) is one of the downstream results of that obstructive action (see Fig. 2).
And, another well-identified garcinia cambogia danger is that ...
Both animal and human experiments with ACL-disrupting HCA-garcinia supplementation found that the products significantly shift the metabolic machinery to the burning of fat (lipid oxidation), away from carbohydrate burning (glucose oxidation) [84,86-88] (see Fig. 2) –making garcinia extract a body fat burner or carb blocker, respectively.
Garcinia's fat burning property is biologically unsettling because fatty acid oxidation is metabolically less efficient and creates a bigger amount of damaging ROS products (e.g., lipid peroxides) in comparison to sugar oxidation (oxidative glucose disposal) [19,32,69].
A classic feature of metabolic irregularity in diabetes is diminished fuel efficiency, clinically evident in a shift from glucose oxidation to fat oxidation [29,60,67] (see Fig. 2). In fact, in diabetes, energy metabolism is not merely suboptimal but also deranged and dysfunctional [29,89].
Metabolic dysfunction (or the "metabolic syndrome") is at the bottom of many, if not all, chronic degenerative diseases, such as cancer, cardiovascular disease (CVD), diabetes, nonalcoholic fatty liver disease, and neurological brain diseases [28,60,68,90-92]. It has been increasingly recognized that heightened metabolic fat burning (fatty acid beta oxidation) is markedly linked to long-term complications of diabetes involving the cardiovascular system, such as the promotion of atherosclerosis [93,94].
The hyperlipidemia of diabetics is further reinforced or aggravated because the ACL/lipid-mediated metabolic dysfunction and destruction of beta cells conceivably lead to a pancreatic insulin deficiency because prolonged exposure to systemic free fatty acids in the blood reduces the gland's insulin yield and release [95] (see Fig. 2).
This relative insulin insufficiency:
- triggers glucagon over-secretion to activate endogenous gluconeogenesis and glycogenolysis, driving plasma glucose levels up (leading to, or exacerbating, fasting hyperglycemia), and
- stimulates cortisol into action initiating the mobilization of free fatty acids from fat depots (lipolysis), raising the blood lipid concentration in diabetics [96] (see Fig. 2), as one of the inhibitory roles of insulin is the occlusion of fat storage breakdown [19,38,47,60] (see Fig. 3).
The mobilization of (storage) fats into the blood as a consequence of pancreatic damage or from a high fat diet (of processed refined foods) triggers the release of insulin [97] which, resembling an acute adaptive reaction, obstructs lipolysis and attempts to recuperate glucose oxidation.
Yet, while a transient exposure of pancreatic beta cells to blood fats stimulates the secretion of insulin, their chronic exposure to lipids decreases insulin release [15,95,98,99] and can lead to chronic hyperglycemia [54] (see Fig. 2).
The state of a pancreatic insulin deficit seriously incapacitates, in a self-enforcing circle, the hormone's function to contain and regulate both fat and sugar content in the blood stream.
The excessive amounts of, or the extended exposure to, long-chain free fatty acids in the circulating blood, culminate in systemic insulin resistance and hyperinsulinemia (one of the symptoms of insulin resistance) because of the fats' destruction of insulin-binding cells in muscle, liver, and heart via increased inflammation and oxidative insults such as from lipid peroxidation [28,66,100-102] (see Fig. 2).
Insulin resistance itself worsens the diabetogenic situation, in what appears to be another vicious cycle, by signaling the release of free fatty acids (lipolysis) from lipid storage [103], exacerbating high blood fat content (hyperlipidemia) and tissue damage from deleterious products of oxidative fat burning.
Normally, insulin lowers the blood sugar concentration [11,80,104] and decreases mitochondrial fatty acid beta oxidation [50] (see Fig. 3). Once insulin resistance, hyperinsulinemia, and (hyperlipidemia/glucocorticoid-incited) hyperglycemia are pronounced as in advanced diabetes 2, insulin injections (insulin therapy) or diabetic drug management are increasingly ineffective in combating the "sugar disease" [105]. In muscle cells of insulin-resistant diabetics, for example, insulin does not properly suppress fat metabolism compared to tissue of non-diabetic subjects [32].
Among the diabetes type 2 information published by the U.S. Center for Disease Control (CDC) it is brought up that in a lot of cases the loss of toes, feet, or legs because of diabetic neuropathy, or blindness because of diabetic retinopathy, or death because of strokes and heart attacks, are the end results of advanced diabetes [12].
Astonishing Diabetes Type 1 & Diabetes Type 2 Information
–How Garcinia Cambogia Side Effects Counteract The Therapeutic Effects Of Diabetic Insulin Therapy
"[...] that is part of what science is: proposing novel explanations from observed patterns in data, from which further work is done to substantiate or refute the initial findings." (David Quist, Mycologist, Environmental Scientist & GMO Whistleblower, in 2003)
How is diabetes treated? The traditional treatment for diabetes mellitus has been insulin therapy. How does insulin work, what is the function of insulin? The principal mode of action of human insulin therapy (i.e., insulin shots, other forms of insulin medication) is glucose control by way of the hormone's ability:
- to suppress adipose lipolysis, the liberation of tissue fats into the blood [47,62], that would lead to a reduction in plasma fat content and fatty acid oxidation [50,62] and, instead, would favor glucose oxidation [50,60] (see Fig. 3);
- to restrain gluconeogenesis (sugar production in the liver) [47] (see Fig. 3). In a pancreatic insulin deficiency state, lipolysis is increased and blood fats intensely stimulate glucagon-mediated hepatic glucose output (gluconeogenesis), cultivating hyperglycemia [62] (see Fig. 2).
When blood insulin concentrations are high (hyperinsulinemia), which is routinely the case in diabetes (e.g., due to insulin resistance), lipids will compete with, and obstruct, glucose "for uptake by peripheral tissues", such as muscle tissue, despite a hyperinsulinemic and hyperglycemic state [62].
Yet, as described above, the primary garcinia cambogia side effects undermine, and actually help to neutralize, the major therapeutic actions of standard type 1 and type 2 diabetes treatment (i.e., conventional insulin therapy), such as the stoppage of gluconeogenesis and the promotion of glucose metabolism, enabling, sustaining, and driving a diabetic state (see Fig. 3).
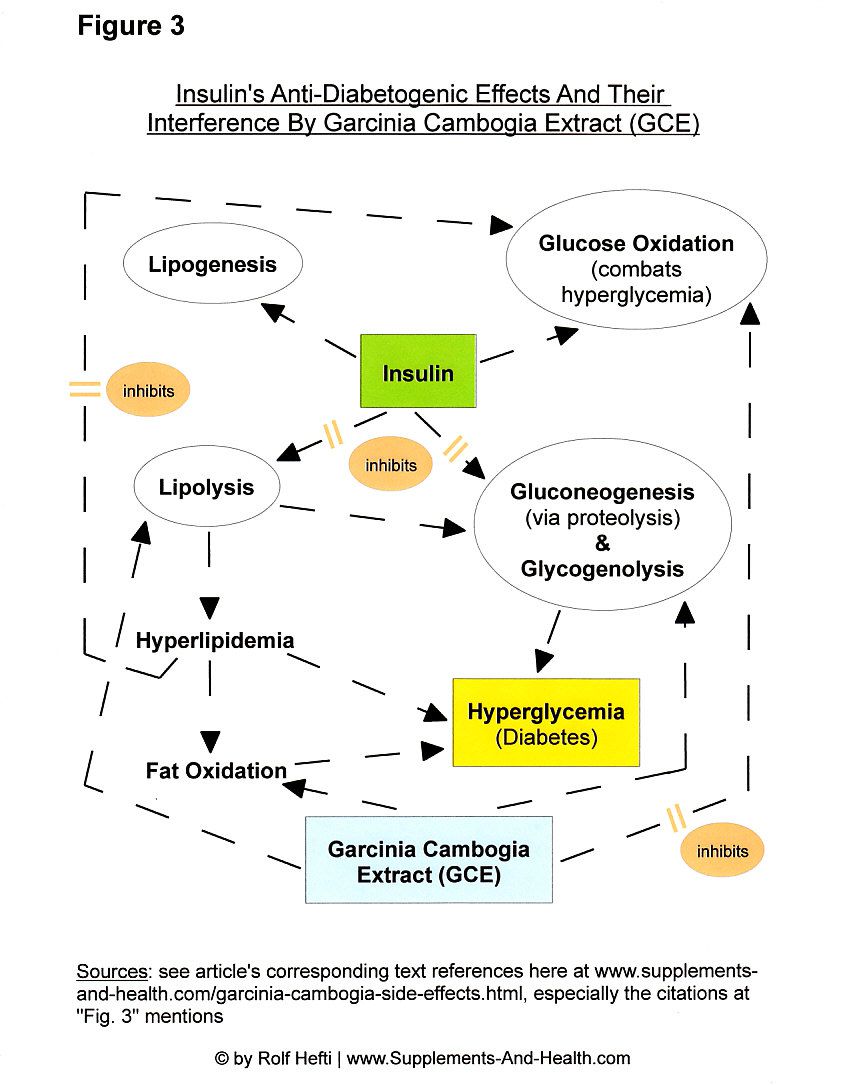
Mark McCarty, a prolific biomedical researcher, brought out in one of his scientific study papers that:
"Disinhibition
of hepatic fatty acid oxidation with hydroxycitrate (HCA) [...] in
diabetics runs the risk of further enhancing excessive hepatic
gluconeogenesis." [54]
Diabetogenic Garcinia Cambogia Side Effects: Increased Pancreatic Beta-Cell Death
“You can’t poison a crucial enzyme or block an important receptor
for the long-term and expect a good result.” (David Brownstein, MD
[363])
The enzyme "ATP citrate lyase" is critically involved
in the body's production (de novo synthesis) of cholesterol and fat
(lipogenesis, involving fatty acid synthesis and triglyceride synthesis)
[3,82,84,106,107] (see Fig. 7). Observed results from biological interference of this ACL-mediated process by the use of garcinia cambogia weight loss pills are
salient reductions in cholesterol and triglyceride levels [84,108,109].
As
aforementioned, among the garcinia cambogia side effects is the
suppression of the lipogenic enzyme ATP citric acid lyase by
hydroxycitric acid (HCA), interfering with the production of the free
form of cholesterol and fats, and optimal metabolic fuel utilization.
The freezing of internal cholesterol synthesis is a physiological worry and potentially dangerous because all vital steroid sex hormones (e.g., pregnenolone, DHEA, progesterone, testosterone), along with bile salts and vitamin D, are made up from this base substrate –namely, LDL cholesterol, the so-called "bad cholesterol" [3,26,110] (see Fig. 7).
(Statins,
cholesterol-lowering drugs, are also known to suspend the production of
other essential nutrients [111], such as co-enzyme Q10 (CoQ10, a.k.a
ubiquinone); for more on that read my piece "Facts About Dietary
Supplements: Supplement-Drug Interactions" –direct link to it at the end
of this article under Recommended next pages. Since
HCA-garcinia cambogia extract disrupts the enzymatic pathway of
cholesterol synthesis further upstream from statins, it is quite
conceivable that the diet supplement too decreases endogenous CoQ10
production –see Fig. 7.)
In terms of steroidogenesis and sexual function, statin therapy is
linked to:
- decreased testosterone levels (a.k.a hypogonadism, androgen deficiency syndrome, or simply "low T" –a marketable abbreviation for "low testosterone", a term popularized by the medico-pharma business),
- loss of libido (one of the potential low T symptoms), and
- erectile dysfunction (also one of the symptoms of low testosterone, due to, presumably, statin drugs' promotion of atherosclerosis –see Fig. 8) [111,115, 347-351].
Further, the substantiated connection between statins and low testosterone has a corollary in the evolution of diabetes. Evidentiary data link a lack of testosterone to an elevated risk of diabetes.
For instance, animal experiments found that a male testosterone deficiency reduces the ability of pancreatic beta cells to secrete insulin upon stimulation by glucose, leading to glucose intolerance and hyperglycemia [359]. Apparently, one of the benefits of testosterone is as a anti-diabetic hormone, and a low T profile fosters a predisposition to diabetes II (T2DM).
In humans, a testosterone insufficiency (a low testosterone condition) in type 2 diabetic men is associated with impaired mitochondrial function and increased inflammation (due to enhanced oxidative stress), leaving these patients more susceptible to cardiovascular malfunction [364].
Research data show that low testosterone levels (both total testosterone and "free testosterone") are significantly related to higher levels of C-reactive protein (CRP), a well-established marker of systemic inflammation [353,354]. In men, low T means more whole body inflammation (a configuration which could be driven or aggravated by adverse effects of statins –and, conceivably, garcinia cambogia side effects).
The low testosterone-high C-reactive protein link is one of several mechanisms of how statins can increase inflammation in the body (including in the pancreas) and is independent from the traditional cardiovascular risk factors. Moreover, some scientific evidence demonstrated an association, in men, between low T and high CRP with the metabolic syndrome or a greater diabetes risk [355-358], corroborating the notion that the disease is a low-grade inflammatory condition.
Furthermore, the real truth about cholesterol and statins reveals that the artificial lowering of cholesterol production through statin therapy (potentially leading to a cholesterol deficiency state) was linked to a significant increase in cancer, stroke risk, and higher mortality (including more suicides) which had been known since at least the 1970s [110-127,333,370].
In their book "How Statin Drugs Really Lower Cholesterol and Kill You One Cell at a Time" (2012) the authors stated that:
"Irrefutable, reproducible science proves statins are deadly and LDL cholesterol is vital to life." [111]
(Intriguing side-note: Niacin is a form of vitamin B3 [129,139]. High-dose niacin lowers cholesterol, an effect encountered with statin drug use. However, the intake of megadose niacin supplements over 10+ years resulted in practically the opposite findings in terms of "side effects" (that is, remarkable niacin benefits): a significant reduction in cancer and mortality, and a longer life [128,129]. Whereas the cholesterol-lowering "statins' side effects" are very deplorable, the cholesterol-lowering "niacin side effects" are very beneficial.
I suspect that the eminent discrepancy in outcomes might be because the impact of deadly statin drugs on cholesterol is (like with garcinia cambogia side effects) the result of blocking the synthesis of the substance (see Fig. 7), slashing free cholesterol levels, whereas niacin pills' curtailing effect on the essential substrate is the result of an energetically-induced acceleration of its conversion to steroid hormones (steroidogenesis), lowering cholesterol concentrations in its wake, because the vitamin niacin (a popular natural cholesterol remedy) is a key material for metabolites of oxidative respiration such as NAD (nicotinamide adenine dinucleotide) and NADH (nicotinamide adenine dinucleotide hydride, the chemically reduced biologically more "active" form of NAD, also known as coenzyme 1) [129].
Most of all, this indicates that how cholesterol numbers get reduced in the body is of decisive relevance.
Meaning, the biological-physiological mechanisms that lead to a sinkage of cholesterol values, for example, whether...
(a) through the shutdown of cholesterol production (with statin cholesterol meds, “natural statins” such as red yeast rice, or hydroxycitrate-laden garcinia cambogia extract supplements),
(b) through the resort to a cholesterol-lowering diet plan emphasizing high fiber foods (foods high in fiber help lowering cholesterol naturally by physically removing or “sweeping” cholesterol from the gut),
(c) through the use of vitamin C supplements (one of the benefits of vitamin C supplements is increased production of bile which sequesters cholesterol; as alluded to, both statins and GCE probably decrease bile synthesis),
(d) through the use of thyroid supplements (thyroid hormone activates the metabolic conversion of cholesterol to sex hormones, shrinking cholesterol levels in its wake), or
(e) through the use of niacin supplements
... determine if a particular method of lowering cholesterol is degenerative or rather regenerative.
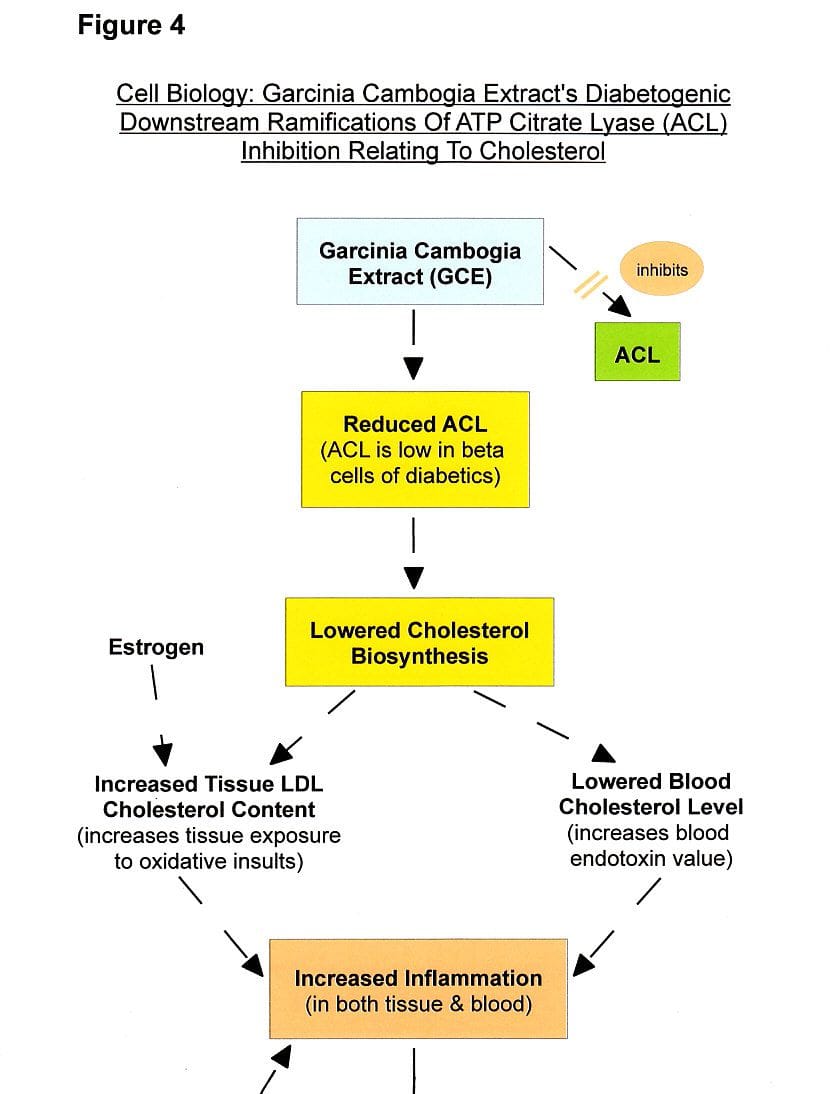
Statins' inhibition of cholesterol biosynthesis (and one of the main garcinia cambogia side effects) results in a corrective-compensatory accumulation of intracellular (tissue) cholesterol levels via an "upregulation of LDL receptors for enhanced uptake of LDL-cholesterol" from blood plasma [111,130] (see Fig. 4).
The serious tampering with the body's creation of cholesterol appears to elevate inflammation in both the organs (cell tissue) and the blood stream. (Although, statins have, just as is the case with "advantageous" garcinia cambogia side effects, some anti-inflammatory properties too, such as through their blockade of cyclooxygenase –the COX enzyme (both the COX-1 and COX-2 variants)– which is responsible for the formation of prostanoids and prostaglandins.)
The clearance of cholesterol from the blood, as a result of upregulated flow of LDL cholesterol into cells, increases the plasma load of inflammatory endotoxins (bacterial lipopolysaccharides or LPS; basically, LPS are bacterial products of intestinal food digestion) because the majority of LPS is normally bound and sequestered by cholesterol in the blood, mitigating and restricting their detrimental activities (endotoxin toxicity) such as cytokine mobilization [131,333,336] (see Fig. 4).
Because LDL cholesterol (LDL-C), traditionally called the "bad cholesterol" [132], is very susceptible to oxidative attacks by reactive oxygen species (ROS), incurring free radical damage, the enhanced LDL cholesterol uptake by cells is theorized to increase the inflammatory burden (probably seriously exacerbated in part by the statin-induced reduction of certain antioxidants such as CoQ10, vitamin K, and selenium-containing glutathione peroxidase [115,360]) in the pancreatic beta islets –mediated by an excess of both oxidative stress and nitric oxide (NO), governed by interleukin-cytokine signaling [28,133,134]– resulting in pancreatic islets dysfunction, lowered insulin yield, and a rise in cell death (pancreatic apoptosis) [133,135-137] (see Fig. 4). (Also, the pro-inflammatory rebound effect of cholesterol-lowering interference could proffer, in part, a reasonable explanation why statins are associated with increased coronary-arterial calcification (atherosclerosis) [360], with the highest score of artery blockage in the group receiving high-intensity statin therapy [251,334] (see Fig. 8).)
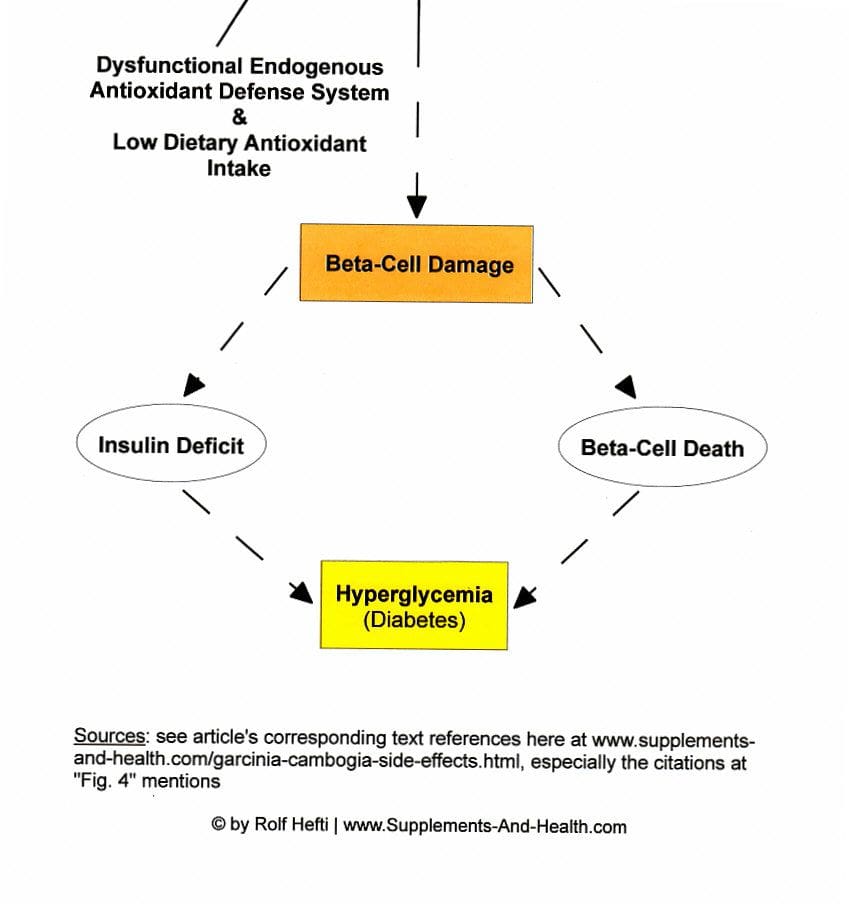
HDL cholesterol, what had been coined "good cholesterol", protects
against LDL cholesterol-induced beta-cell dysfunction and
inflammation-induced apoptosis [130,138]. And, one of the purported
health benefits of niacin supplements is that they elevate HDL
cholesterol concentrations [139]. Although, statin-incited boost in HDL cholesterol had been associated with an increased risk of cardiovascular disease [110].
These
biological side effects from the inactivation of cholesterol
bioproduction had been proposed to account for the elevated diabetes
risk in connection with the intake of (certain) statin cholesterol meds (i.e.,
statin-induced new-onset diabetes mellitus) which stifle de-novo cholesterol synthesis [130,137], akin to garcinia cambogia side effects (see Fig. 7).
Garcinia
cambogia-HCA has some anti-inflammatory action due to its
bioflavonoid-polyphenol content [108,140]. Presumably, this counteracts
or attenuates some of the manifold pro-oxidant, inflammatory
ramifications induced by HCA-incited garcinia cambogia side effects,
such as:
- the poisoning of cholesterol synthesis,
- the stimulation of lipolysis (an outcome of the reduction of insulin viability through ACL-inhibiting garcinia cambogia side effects), and
- garcinia's direct rearrangement of fuel metabolism from glucose to fat burning.
Apoptosis, by the way, is predominately a protective mechanism [141].
Programmed cell destruction, i.e., apoptosis, is a process essential to
growth, development, tissue homeostasis, and survival of the organism
[142]. For instance, when normal cells get heavily or irreparably
damaged –as beta cells of the pancreas do by oxidative stress, for
example [143]– or in cases of mitochondrial disorders [141], the
abnormal cells signal the initiation of their own demise (cell suicide),
as the mitotic replication of dysfunctional, damaged, or old cells
isn't constructive to the integrity and survival of the body system
[144].
If apoptosis is perpetually high in normal beta-cells,
whereas the ratio of cell loss to new cell growth increases, the
pancreas will have progressively less functional cells, manifested in
beta-cell mass reduction, to express its vital physiological roles such
as producing and secreting insulin, externalized in a loss of insulin
output, resembling and defining the pathological configuration of type 1
diabetes (among the cardinal symptoms of diabetes type 1 is the loss of
insulin production).
And, as stated before, a lack of insulin
compromises the hormone's function to suppress (1) internal sugar
production and (2) glycogen breakdown in the liver, allowing for blood
glucose levels to rise excessively, thereby intensifying or contributing
to hyperglycemia (high blood glucose levels) [47] (see Fig. 2 & 3).
NO-mediated
pancreatic beta cell destruction (apoptosis) is the chief cause for the
insulin dependency of type I diabetics [133]. And the ACL enzyme is
closely intertwined with cell apoptosis.
Normally, the concentration and activity of cytoplasmic ATP citrate lyase (ACL/ACLY/ATP-CL) is particularly high
in healthy pancreatic beta cells –compared to other cell types– of both
humans and animals [20,145,146], supporting cellular integrity and the
proliferation of new cell growth (mitosis), and sustaining a healthy apoptosis
index.
The overabundance of ACL viability in beta islets supports
the data showing that beta cells represent "lipid synthesizing tissue"
(fat storage) [146] rather than lipid consuming tissue (fat
beta oxidation). (Among the leading garcinia cambogia side effects, hailed as beneficial weight loss actions, are the termination of fat
storage and the shift to lipid oxidation, mediated through ACL
inhibition (see Fig. 2).)
Low ATP citrate lyase status, independent
from its association with dietary lipids, correlates with an
augmentation of pancreatic islets cell death (apoptosis), and its
up-regulation (overexpression) blocks the termination of pancreatic
cells by free fatty acid combustion, underscoring the highly pivotal and
protective role of ATP citrate lyase in pancreatic cell survival [20].
Fascinatingly,
other normal human cells, such as lung cells, don't (readily) succumb
to increased apoptosis in a ATP citrate lyase deficiency (ACL
deficiency) state [147]. I reckon that the higher apoptotic
susceptibility of pancreatic beta cells in low cytosolic ATP citrate
lyase conditions is directly related to their elevated risk of incurring
oxidative-inflammatory injuries [148], facilitated by poor basal ATP
formation [81] relative to most other cell types, a situation that
fosters apoptosis despite a customarily high beta-cell content of
apoptosis-shielding triglycerides [149].
In parallel to the
augmented oxidative stress exposure from lipolysis and the choking of
cholesterol generation via the HCA-laden garcinia cambogia
extract-induced suppression of ATP citrate lyase, is a defective
internal antioxidant defense system in certain people with advanced type
I diabetes, worsening the situation synergistically in those
individuals [150] (see Fig. 4).
In diabetic animals the level and activity of
ATP citrate lyase in the liver and pancreas beta-cells is low, and a
diet high in fat (or fasting) reduces the enzyme [151-153].
Analogously, the activity and concentration of ATP citrate lyase is typically and notably reduced in pancreatic islets beta cells of people with diabetes mellitus type 2 compared to non-diabetic individuals [20,146].
The
predominant effect of HCA, the main "active" ingredient of garcinia
cambogia diet supplements, is the inhibition of the ATP citrate lyase
enzyme [2,82-85], a clinical feature that accelerates and aggravates
apoptosis of normal beta cells –one of the most worrisome garcinia
cambogia side effects, especially for diabetics or prediabetics.
Garcinia-HCA Extract's Impact On Leptin: More Diabetes-Inducing Garcinia Cambogia Side Effects?
"He who is afraid of asking is ashamed of learning." (Old Danish Proverb)
What is leptin? The traditional leptin definition identifies the substance as the so-called "satiety hormone" (leptin means thin) because leptin exerts a pivotal influence on food intake due to its central role in the regulation of metabolism and energy expenditure [154]. Rare cases of human genetic mutations that result in a congenital deficiency of leptin were linked to severe obesity [155]. Other research experiments in both humans and animals found that a lack of leptin protein, or its genomic substrate, the obese gene (OB gene) [156], causes massive obesity [157].
The leptin connection with diabetes is also supported by scientific data. Mice with a genetic defect in the leptin protein/gene are typically obese, inactive, diabetic, have a lower body temperature and energy metabolism [158].
Injections of the "fullness hormone" leptin into these mice caused:
- a decrease in food intake,
- weight loss,
- an increase in physical activity,
- a reduction in both glucose and insulin blood content,
- a rise in body temperature (via upregulating brown fat thermogenesis), and
- a higher metabolic rate [158,159].
Practically none of these observed alterations were noted in lean
controls that had been subjected to leptin injections [158,159].

Importantly, leptin is intricately implicated in both regeneration (health) and degeneration (disease) –depending mainly on its concentration, functionality, the duration to its exposure, the overall state of health of a person, and, conceivably, tissue localization.
Leptin, for instance, increases oxidative injury (free radical stress) because of its preference for metabolic burning of fat [160,161], demonstrated by higher amounts of markers of lipid peroxidation (e.g., isoprostanes) in the blood circulation and urinary excretion [162] (which may epitomize insulin resistance symptoms).
Conversely, a low leptin tone can, among other adverse effects, lead to immune deficiencies/compromised immune system (e.g., thymus gland shrinkage and lymph system degradation) and a poisoning of thyroid function [163-166]. As aforenoted, untreated patients with diabetes have a decreased blood concentration of the thyroid hormones T3 and T4 [56]. This seems to support the sentiment that a leptin deficit exacerbates the diabetic thyroid dysfunction.
Leptin is predominantly derived from fat cells [157]. What is the role of leptin? Evidently, one of its most prevalent, and arguably most important, functions and occurrences appears to be in the brain [154,167]. After all, glucose control, insulin release, and other prominent biological processes of diabetes are intimately linked to the brain-pancreas axis [81] (see Fig. 1).
Leptin has powerful neuroprotective effects: it fights inflammatory-oxidative insults in the central nervous system such as the brain, it guards the stability of the mitochondria, it protects against neural excitotoxicity, it upregulates defensive brain antioxidants, and it reduces cell apoptosis through the prevention of oxidative-excitotoxic attacks [81]. A specific example of leptin benefits is the hormone's ability to vigorously protect brain cells from iron-induced damage [81].
As alluded to earlier, chronic inflammation and oxidative stress in the brain, leading to brain cell damage, are strongly associated with the onset and exacerbation of diabetes [39].
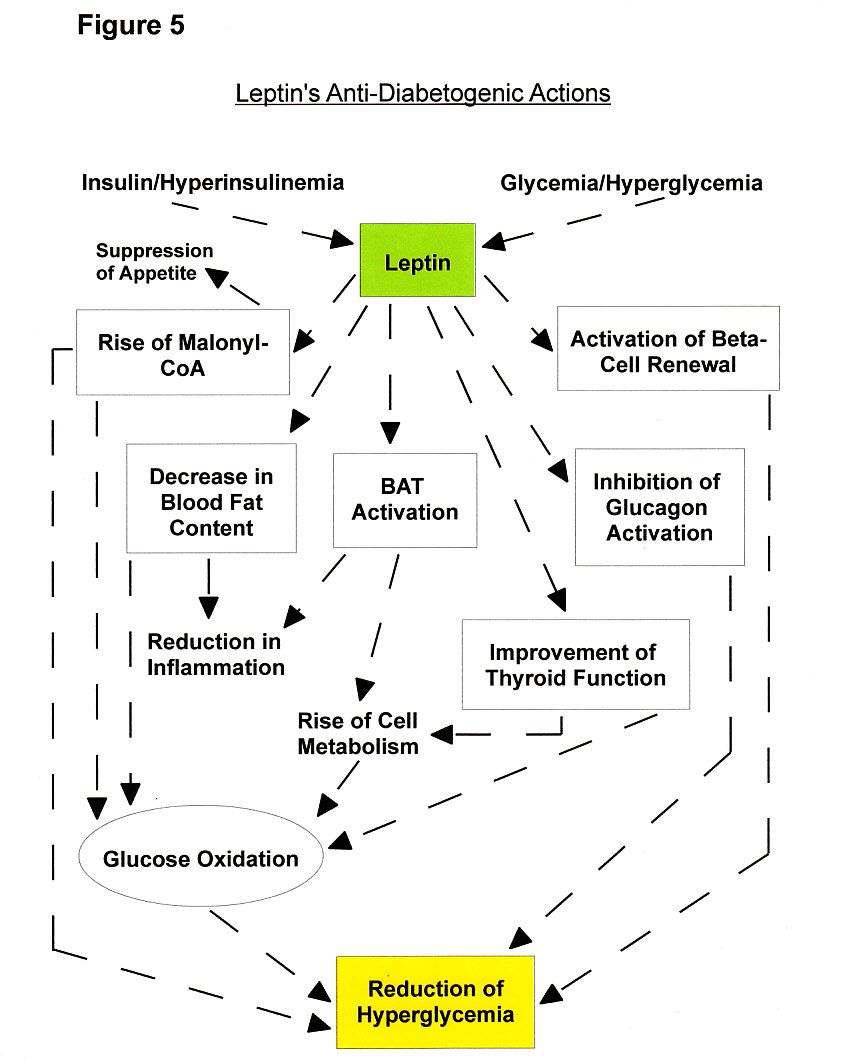
In addition, leptin has mighty protective effects on the mitochondrial integrity of pancreatic cells against various stressors [168] and it activates the mitotic growth of new insulin-secreting beta cell in the islets of Langerhans [169-171] (see Fig. 5). Although, while leptin activates insulin production, leptin inhibits insulin secretion into the blood stream because leptin and insulin have antagonistic effects [161]. Among the classic characteristics or warning signs of diabetes is mitochondrial dysfunction which leptin therapy was able to restore in obese diabetic mice [22].
Apart from being an agent of beta-cell regeneration, another beneficial pancreatic effect of leptin is its prevention of the accumulation of fats in the insulin-secreting organ (and other body tissues) in instances of overeating (hyperphagia) because the hormone's deficiency or inadequate cellular utilization (leptin resistance) results in lipotoxicity (e.g., lipoapoptosis) of nonadipose tissues such as with the dysfunction or killing of beta cells in the pancreas [75,77].
Leptin's anti-diabetic action of lowering blood carbohydrate content and improving glucose metabolism (in muscles), via a raise in blood leptin content, had also been recorded [158,161,172,173], possibly by raising malonyl-CoA (malonyl coenzyme A) [174] and suppressing glucagon secretion [175], helping to forestall the induction of diabetic hyperglucagonemia (high blood glucagon levels) [176] (see Fig. 5).
A reciprocal homeostatic relationship seems to be at work between leptin and glucose because (increased) glucose metabolism or blood glucose (or insulin) content drives and turns on leptin secretion and augments the number of leptin receptors the hormone gets bound to (yet carbohydrates reduce plasma leptin which, I assume, is because of heightened leptin activation, increasing tissue-bound leptin content from a higher intracellular influx) [177-181].
In lean leptin-deficient mice with diabetes type 1 and hyperglycemia, the administration of leptin therapy, with high or low doses, significantly lowered blood glucose (and free fatty acid) levels in all the treated animals, prevented the catabolic state of cachexia (=wasting disease), diabetic ketoacidosis (an insulin deficit activates ketogenesis [47]), and death, restored hemoglobin A1c (HbA1c) back to normal, and markedly reduced food intake and induced weight loss (primarily body fat) [175]. (HbA1c refers to glycated hemoglobin, a marker of glycemic control [47].)
However, leptin treatment in animals with tainted leptin signaling pathways and functionality in the central nervous system (e.g., the brain) failed to evoke several of these anti-obesity/anti-diabetic effects [182]. Disturbed leptin function in the brain, leading to dysfunctional brain-body leptin signaling, may also explain why in obese humans with type 2 diabetes leptin replacement therapy, albeit raising blood leptin concentration, did not elicit a loss of weight or improve glycemic control [183].
Overweight or obese people frequently suffer from hyperleptinemia [184]. Yet while the leptin status in the brain of obese individuals is marginally increased, their blood leptin values are extremely high compared to the former [185]. Faulty leptin receptor functionality or signaling in the central nervous system, such as the brain, appear to account for the inconsistent clinical observations with leptin treatment [182].
Diabetic rodents have distinctly reduced blood plasma leptin levels [178]. Rodent experiments found that HCA-garcinia cambogia extract lowered both insulin and serum leptin levels [186,187]. In statin-induced new-onset diabetes type 2, one of the proposed mechanisms for the depressed pancreatic insulin release and the stifling of beta cell functionality and proliferation, is the decrease in leptin concentration [188].
In terms of leptin side effects, an inhibitory action on leptin may be constructive in obese type 2 diabetics. Among the undesirable diabetes symptoms are cardiovascular events such as atherosclerosis [29]. An elevated serum leptin prominence is associated with vascular dysfunction, heart attacks, and heart disease [189-191] which may be potential repercussions of intensified production of free radicals in vascular cells [192] because leptin privileges the metabolic combustion of fat [160,161] and high blood leptin content, as in hyperleptinemia, leads to increased oxidative insults intracellularly [193]. Leptin, for instance, is positively associated with the hardening of arteries (atherosclerosis) and blood platelet aggregation [191,194].
Yet, other studies found that the negative correlation between leptin concentration and vascular function disappeared after adjusting for obesity, body mass index (BMI), or hyperinsulinemia [195,196]. Indeed, an ex vivo study reported "better" vascular function in overweight human diabetics with higher leptin levels, independent of BMI, obesity, or insulin status [197]. Nevertheless, body fat mass does positively correlate with blood leptin levels [191], presumably because fat cells manufacture the hormone.
Is the correlation of high blood plasma leptin and cardiovascular and coronary heart disease perhaps a downstream ramification of a dysfunctional leptin-mediated brain-body constellation? In animal vascular ischemia, a symptomatology of a potential impeding heart attack, the leptin functionality in the brain is impaired [198]. The dysfunction in neuronal leptin signaling is thought to cause hyperleptinemia (high blood leptin levels) [199,200].
Leptin stimulates lipolysis in white fat tissue via nitric oxide activation [201,202]. Although in obesity, the leptin-NO (nitric oxide) mechanism seems to be broken [203] –perhaps, this might also be the case in diabetes 2. Among garcinia cambogia side effects is the aforecited repressive action on leptin, thus the diet supplement may emanate some beneficial anti-lipolytic activity, concurrent with its pro-inflammatory, pro-lipolytic action (from its selective championing of fatty acid oxidation and its prohibiting action on insulin production via ACL disruption –see Fig. 2).
Leptin, like a garcinia cambogia supplement (i.e., GCE), promotes fat oxidation, displacing tissue glucose metabolism [160,161]. But while GCE-HCA nutritional supplements target the release and combustion of white fat [187], which is abundant in the viscera and the abdomen ("belly fat"), leptin appears to mostly stimulate the burning of brown fat, located preferentially in the upper region of the body, especially the neck area, via adaptive thermogenesis characterized by the hormone's capability to marshal the transformation of white fat to brown fat for fuel combustion (the "browning reaction") [209,213] depending on the unique situational context, generating oxidation energy, in response to –for example– prolonged exposure to metabolic stressors [204-209]. (The topical overabundance of brown fat mass around the central nervous system, the brain, and the heart –and, perhaps, that it is more prevalent in children than adults [210]– seems to indicate the supreme physiological-evolutionary importance of this category of fat and brown fat thermogenesis.)
Also, brown adipose tissue (BAT, colloquially known as brown fat), and beige fat are primarily designated for dynamic adaptive energy expenditure (or heat production), used for such situations as thermoregulation in cold environments [211], compared to white fat (white adipose tissue or WAT) that is aimed mainly at energy storage [209,211-215].
The BAT-recruiting property of both leptin and insulin, mediated by activation of the brain's hypothalamus [215], is responsible for increased metabolism and body temperature.
The dynamic energy-mobilizing capacity and role of brown fatty acids is highlighted by the following:
- the presence of a copious number of mitochondria, the furnace units of energy production, and the respiratory enzyme cytochrome C oxidase in brown fat cells [209,216], compared to few mitochondria in white fat cells [211] (the discrepancy in mitochondria count explains the name "brown fat" because mitochondria carry the brownish-red mineral iron [217]);
- brown fat formation and activity is triggered by stressors (e.g., the thermal stress of cold environments) through various stress hormones [206,209,218]. (Exposure to stressors also leads to the generation of new mitochondria [218] and stress-mediating pathways (e.g., the sympathetic nervous system) are also engaged by leptin [160,161]);
- plain sugar (sucrose), containing the ideal energy fuel source (i.e., glucose), also raises brown fat metabolism by decidedly increasing brown fat mass [219].
Whereas glucose combustion bears the most metabolic efficacy, producing ATP [29,97,220], the oxidation of brown fat (BAT thermogenesis) produces little chemical energy in the form of ATP but blows off chemical energy in the form of heat [209,211,212,221].
The disposal of (excess) body energy, via the calorie-burning capacity of functional BAT-combustion, helps to prevent and quench metabolic disorders (induced by, for example, high-fat diets or lipolysis) such as obesity and diabetes [211,212,221-224].
Exposure to cold temperatures, raising brown fat weight and cytochrome oxidase activity (and, thus, the rate of cell respiration) to an extreme degree, was reported to ameliorate and reverse the diabetogenic effects (e.g., insulin resistance) of eating large amounts of (highly processed) fatty food, by raising insulin sensitivity (how easily and properly tissues detect the insulin signal) and improving glucose tolerance [225].
It needs to be kept in mind that in thermoneutral environments where brown fat burning isn't recruited to elevate the basal metabolic rate in order to maintain body temperature, the anti-obesity effect of heat-generating brown fat thermogenesis dissipates [209]. On the other hand, activated thermal beige and brown fatty acid oxidation was reported to decline in proportion to increasing excess weight (obesity) [215,226,227].
The more abundant functional brown fat reservoirs are in a person, the higher is the basal rate of metabolic respiration [227] –dispensing surplus metabolic energy at an increased rate relatively independent of the person's unique situational context.
When brown fat oxidation (BAT oxidative metabolism) is switched on, the tissue repository consumes about as much glucose as the brain [211], although the fat tissue still uses mostly lipid fuel molecules as its main fuel source [228]. For instance, in muscle cells, leptin also increases oxidative glucose disposal in addition to primarily invoking fat metabolism [161] (see Fig. 5).
Efficient brown fat combustion reduces free radical damage and modulates inflammation [229] and, thus, is a potential mechanism responsible for leptin's and insulin's impressive brain benefits, protecting the integrity of neurons, due to these two hormones' central role in brown fat thermogenesis, promoting the hypothalamus-mediated white-to-brown fat transformation (the "browning reaction") [215] and brown fat tissue distribution around the central nervous system (CNS). A deficit of leptin, therefore, is arguably spoiling the organism's efficacy to convert WAT to BAT (meaning it has a retarding impact on the "browning reaction"), slowing down the rate of a safer form of metabolic fat burning (i.e., brown fat thermogenesis).
Garcinia cambogia supplement's dampening effect on leptin and insulin [186-188] might attenuate or, perhaps, abolish the diet nutritional supplement's observed inflammation-reducing property in the brain.
And, there is a link between insulin and leptin. Brown fat, which is activated by leptin (among other agents), plays a role in insulin secretion. And insulin regulates cell metabolism in both white and brown fat tissue [230]. Insulin, for example, summons brown fat thermogenesis by raising glucose oxidation ("glucose burning") [161], and triggering WAT browning [215]. In animal tests insulin dysfunction in brown fat cells (BAT) was correlated with defective insulin secretion from pancreatic beta cells [230].
In terms of leptin and appetite, the leptin hormone has powerful effects on the taste organ, especially in regard to foods with a sweet taste, acting as an all natural appetite suppressant (which prompted some individuals or organizations to recommend "leptin foods" or a "leptin diet" to combat the obesity epidemic). Experiments uncovered that leptin, via the hypothalamus, thwarts taste cell responses to sweet substances such as sugar (sucrose), curbing food cravings for sweets and modulating gluttony [231-233].
Further scientific backing of the idea to contemplate leptin for weight loss is that another leptin-cued mechanism of controlling feelings of hunger or food intake is the hormone's capability to raise the important metabolic intermediate malonyl-CoA (in the brain's hypothalamus), a coenzyme that had been called a "signal of plenty" [174], the deficiency of which is decidedly linked to an increase in appetite [234]. Accordingly, hydroxycitrate's dimming of malonyl-CoA levels increases appetite [243] (see Fig. 5).
Apart from lowering leptin, among garcinia cambogia side effects is the interference with malonyl-CoA synthesis (see Fig. 6), diminishing its production (thus, we have at least two physiologically accounted processes that oppose and diverge from the consistent marketing-"research" meme that garcinia cambogia extract is a natural appetite suppressant).
Here are more research data on the adverse side effects of garcinia cambogia by way of tampering with malonyl-CoA...
Some Specific Mechanisms Of Garcinia Cambogia Side Effects
–How Garcinia Cambogia Weight Loss Pills Impair Energy Metabolism And Block Insulin Secretion
"Impaired or insufficient insulin secretion results in diabetes mellitus." (Diabetes Researchers Patrik Rorsman, PhD & Matthias Braun, PhD, MD [80])
As mentioned earlier, HCA-concentrated garcinia cambogia diet pills disrupt triglyceride and cholesterol production and interfere with the most adept process of oxidative mitochondrial respiration (i.e., glucose combustion) of (pancreatic) cells via the interruption of ATP citrate lyase [3,84,107].
How exactly do garcinia cambogia side effects downregulate cellular energy metabolism and disrupt insulin release?
Citrate (a product of citric acid) is the substrate for, or the precursor of, malonyl-CoA (malonyl-coenzyme A), a key extra-mitochondrial substance of, ultimately, mitochondrial oxidative metabolism (oxidative phosphorylation) [235]. The master enzyme required for the conversion of citrate to malonyl-CoA is ATP-citrate lyase [97] –the very cytoplasmic enzyme that is downregulated by HCA (and certain essential fatty acids and saturated fatty acids [20,71,78]). More specifically, ATP citrate lyase is the constituent of the next-to-last enzymatic step in the chemical transformation of citrate-to-Acetyl CoA-to-malonyl CoA (after citrate exits the mitochondrial Krebs cycle/citric acid cycle, i.e., mitochondrial oxidation) of cellular energy metabolism [97,237,244] (see Fig. 6). (This is further corroborated by research information showing that hydroxycitrate doesn't appear to disrupt citrate synthesis but lowers the malonyl-CoA tissue levels [237]).
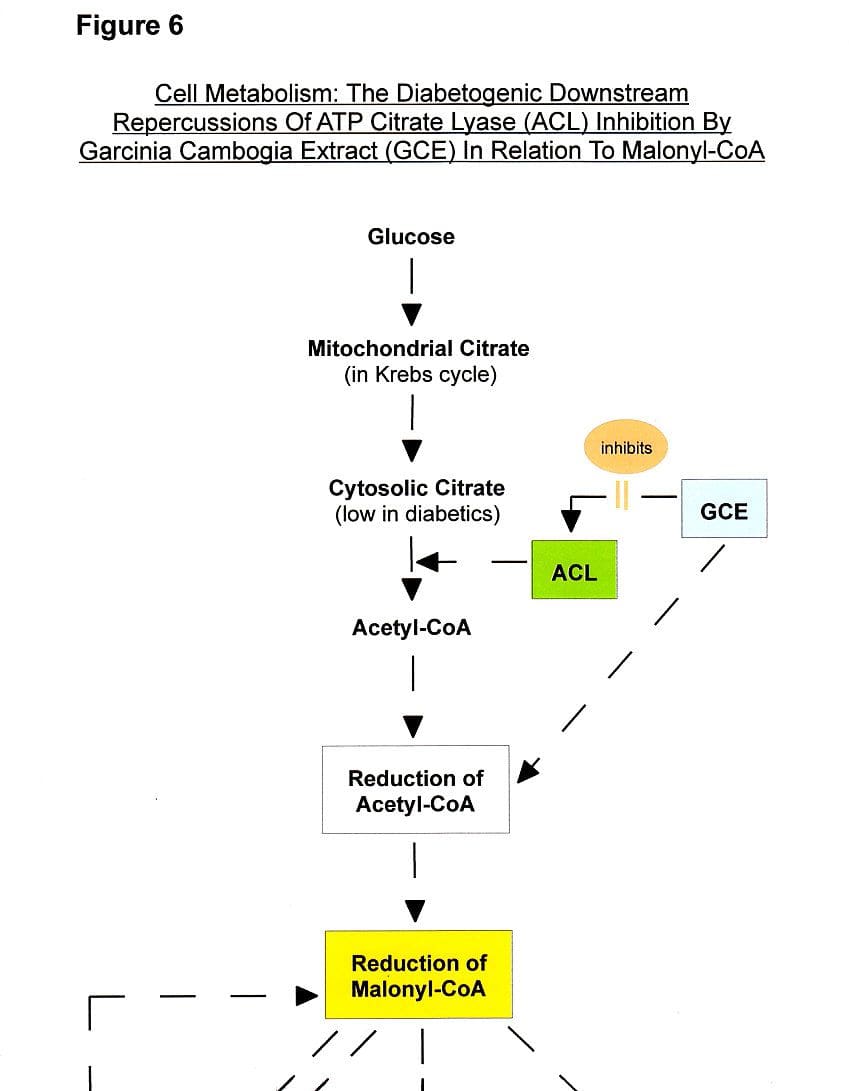
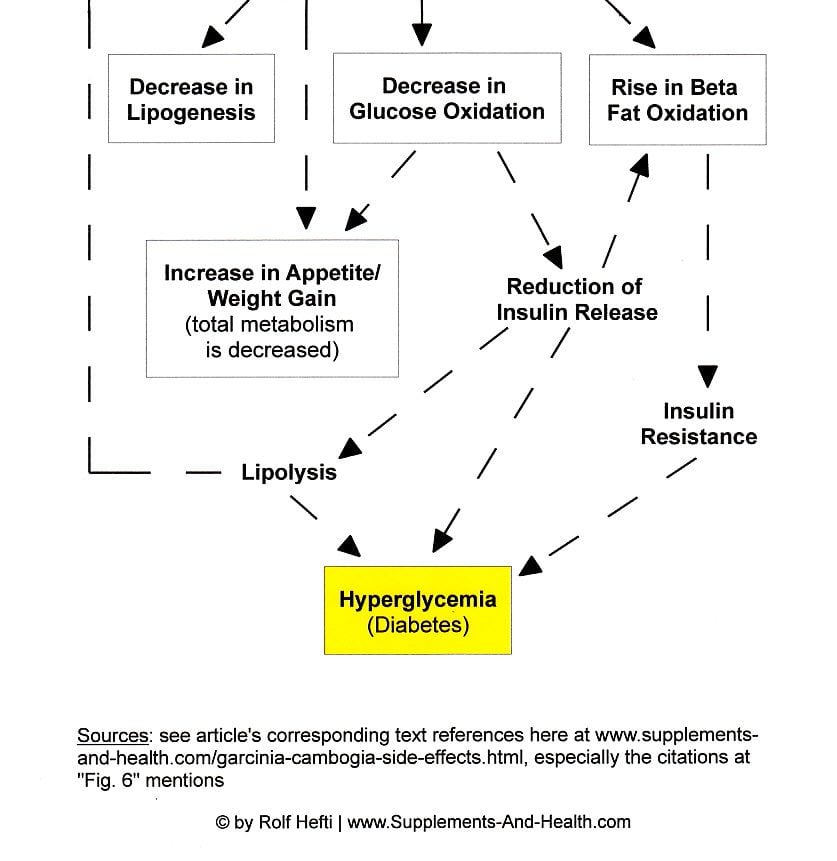
Unsurprisingly, garcinia cambogia-hydroxycitric acid weight loss
supplements lower malony-CoA [97,174,236,237]. And, the inhibition of
malonyl-CoA production (such as with garcinia cambogia supplements)
reduces glucose-induced insulin release [97] (see Fig. 6).
A chief role of
malonyl-CoA is the prevention of entry of fats from the cell's cytoplasm
into the cell's mitochondrion, to be used as a metabolic fuel (fatty
acid oxidation or beta oxidation) [237,238,338].
A low
malonyl-CoA status activates the transport of long-chain fatty acids for
metabolic fat disposal into the cell's mitochondrium [68,96,97],
whereas a high level of malonyl-CoA obstructs blood fats from getting used as a metabolic fuel by the cells' mitochondria [97,234,239,338].
Hence,
the garcinia-hydroxycitric acid supplement increases oxidative fat
metabolism by downregulating the citrate to malonyl-CoA conversion,
induced through the inhibition of the cytoplasmic ATP citrate lyase
enzyme by the "breakthrough" weight loss pill [57,97] (see Fig. 6).
Malonyl-CoA
is synthesized from both lipids and glucose [234,237]. Glucose or high
blood sugar levels propel the production of citrate, ATP citrate lyase,
and malonyl-CoA [50,71,81,240,337,338]. (In diabetes mellitus type 2
patients citrate production appears to be also poisoned because citrate
synthase activity, responsible for citrate synthesis, is reduced [241]
despite the common simultaneous existence of fasting hyperglycemia (high
fasting blood glucose level) with the disease, indicative of systemic
metabolic derangement of respiratory capacity.)
The observation of suboptimal citrate synthesis in diabetics, producing smaller pools of citrate, and the subsequent additional
impairment of the synthesis of malonyl-CoA (from a pre-existing
diminished condensation of citrate) by way of garcinia cambogia extract
intake, amounts to adding insult to injury (see Fig. 6).
Because both glucose and insulin upregulate the production of ATP citric acid lyase and malonyl-CoA, the simple carbohydrate and insulin aid in shifting free fatty acid oxidation back to glucose metabolism
via the suppression of a carnitine pathway [50,68,97,98,237,321,338].
(These physiological principles, discovered in 1977, form the basis for
the concept of the reciprocal "Randle cycle" (the "Glucose-Fatty Acid Cycle") [50,240].)
A high
malonyl-CoA value is also closely associated with reduced appetite and
physical leanness, whereas its increasing deficiency or total lack ensue
in weight gain or obesity [234] (see Fig. 6).
Incidentally, the inactivation of
the cytosolic ATP citrate lyase enzyme (with garcinia cambogia-HCA diet
products) leads to both a reduction of triglycerides (fat production)
and the activation of beta oxidation (fatty acid burning) via the
obstruction of malonyl-CoA synthesis because that coenzyme regulates
both fat production and fat burning [97,237] (see Fig. 6).
A
dysregulation of malonyl-CoA metabolism and increased oxidative fatty
acid disposal (beta oxidation) are firmly implicated with insulin
resistance [32,34,68].
Some data indicated that the combination
of metabolically functional glucose utilization and adequate leptin
content (which, as already stated, are both downregulated by the
suppression of ATP citrate lyase) elevates the synthesis of malonyl-CoA
more than do the individual parameters alone [234]. Oxidative glucose
viability appears to be an essential requirement for leptin to increase
(hypothalamic) malonyl-CoA levels [234].
In regard to blood
glucose levels in diabetes and in people without the disease, one of the
main functions of insulin is to lower, or balance, high blood sugar
values [11,47,80]. Insulin accomplishes this by enabling and supporting
the preferential burning of glucose as the metabolic fuel material
instead of fat [50,60] and the strangling of hepatic sugar production
[47] (see Fig. 3).
Insulin release, from glucose stimulation, stymies body
fat burning (free fatty acid oxidation), fat store mobilization
(lipolysis), and it increases triglyceride synthesis [19,38,60,97] (see Fig. 3).
Pancreatic beta cells normally contain high levels of triglycerides,
protecting them against oxidative DNA damage-mediated apoptosis induced
by free fatty acids [149,242].
Research data [3,81,98,99,129,235,239,337,338] found that insulin secretion is triggered and stimulated by:
- adequate malonyl-CoA production in the pancreas,
- short-term exposure to blood fats (e.g, dietary long-chain saturated fatty acids can initiate insulin release),
- sufficient NADPH index (NADPH, nicotinamide adenine dinucleotide phosphate, is derived from NADH which niacin pills raise [129,139]; NADPH is involved in cholesterol synthesis), and
- adequate glucose concentration.
One of the principal mechanisms allowing proper insulin secretion is a high aerobic metabolism –or an "acceleration of the metabolic flux"– [81], and, as already described, the most efficient fuel to accomplish that is glucose [29,97,220].
However, as explained, the use of HCA-saturated garcinia cambogia extract promotes fat burning [50,96,97,238,239] instead of metabolizing glucose, the most usable fuel substrate to increase total cellular respiration [97], requiring less oxygen [19,29] to generate cellular energy in the form of adenosine triphosphate (ATP) [220].
With functional sugar metabolism, the increased shuttling of glucose (in place of fatty acids) into the mitochondria augments the production of citrate and other metabolic intermediates such as malonyl-CoA [50,81,338], stimulating insulin release [81]. A decline in glucose-stimulated cytosolic citrate production reduces glucose-stimulated insulin secretion [337]. (Reiterating because of its importance and ease of understanding, the synthesis of malonyl-CoA from citrate is tainted by one of the main garcinia cambogia side effects, the suppression of ATP citrate lyase.)
Hence, the burning of sugar (glucose) appears to be pivotal for physiologically-sufficient insulin secretion from the pancreas. Garcinia cambogia side effects derail that biological process.
It is well-established that insulin secretion, in turn, inhibits fatty acid beta oxidation and incites the generation of malonyl-CoA, at least in muscle and liver cells [50,239,243]. In the diabetic state, with defective inadequate insulin synthesis or release from the pancreas, and high blood fat content (hyperlipidemia), the concentration of malonyl-CoA in the liver drops [96].
In skeletal muscle tissue of insulin-resistant type II diabetes patients, however, the content of malonyl coenzyme A is elevated and metabolic fat catabolism reduced –yet fatty acid oxidation remains higher and glucose oxidation lower compared to non-diabetic individuals without insulin-resistant muscle tissue [32].
How come?
The exposure to a glucose-mediated insulin load usually deters metabolic fatty acid beta oxidation but the reduced sensitivity of muscle cells to insulin exposure in cases of diabetic insulin resistance impairs and reduces the elevation of malonyl-CoA, and the chemical's subsequent functions to (1) inhibit respiratory fat burning and (2) to stimulate metabolic sugar disposal, respectively [32].
And as laid out earlier, one of the other prominent garcinia cambogia side effects –the obstruction of cholesterol synthesis– also leads to the dysfunction of the pancreas (see Fig. 4). Research evidence described how the inhibition of the synthesis of cholesterol in pancreatic beta cells ensues in a blockage, thus reduction, of insulin secretion [245,246].
In a mice study garcinia cambogia extract was observed to lower the level of insulin compared to the placebo group [186]. An experiment with HCA-garcinia cambogia extract in rats did notice a decrease in fasting insulin concentration (but without signs of development of insulin resistance) in the active study group compared to the untreated animals [140]. A trial with a garcinia cambogia extract in obese women, however, did not observe any notable fluctuation in their insulin levels over the control subjects [109].
Other investigative data attest to insulin-involving diabetogenic garcina cambogia side effects. Research evidence found that hydroxycitric acid (HCA) profoundly inhibits insulin release from beta cells in the pancreas [88,244,247]. This was corroborated by experimental findings demonstrating that decreased levels of ATP citrate lyase, the key enzyme which is crippled by HCA-garcinia cambogia extract, significantly reduced glucose consumption [86,248] (whereas HCA-garcinia cambogia extract boosts glycogen production (gluconeogenesis) [86,88]). And, an insulin deficit (as already explained) triggers gluconeogenesis [45-47,51] (see Fig. 2).
This means that a suppressed generation of malonyl-CoA and insulin secretion (induced, for example, by garcinia food supplements because these two adverse reactions are well-recorded garcinia cambogia side effects) probably nurtures the existing diabetic condition of high plasma glucose concentration by the shift in source of metabolic energy from sugar to fat [32,96,237,243], leading to hyperglycemia in a mutually-enforcing cycle in which cellular glucose usage is inhibited, insulin secretion constrained, and (accelerated) hepatic glucose synthesis (gluconeogenesis) is turned on.
In a research study on cellular fat uptake and oxidation, and insulin resistance, the authors opined that:
"[...] decreasing muscle fatty acid uptake can improve insulin sensitivity." [34]
The longtime diabetes scientists Josephine M. Forbes and Mark E. Cooper denoted in a study paper that:
"Abnormalities in energy production are thought to be major contributors to the development of diabetic complications." [29]
Other diabetes investigators commented that the biological disruption of enzymatic metabolic pathways by garcinia cambogia-derived hydroxcitrate...
"[...] is likely to have some effect on insulin sensitivity that can lead to type-2 diabetes [...]." [3] [emphasis added]
I saw that a fairly popular garcinia cambogia website, marketing and selling the diet supplement, had listed this study reference [3] on their site (for a total of only three cited study references on the entire sales page/website) supposedly favorable to the use of garcinia cambogia supplements ("it supports healthy cholesterol levels"). Yet, nowhere on that sales-oriented garcinia cambogia website is the reader of it ever told of this troubling statement by the study authors –or that the suppression of cholesterol synthesis, lowering LDL-C levels, hinders insulin release. Garcinia cambogia side effects are ignored while purported garcinia cambogia benefits are accentuated.
It is also worth noting that the merchants of the traditional medical profession routinely resort to the same type of specious argumentation and claims allegedly in favor of their highly profitable medical merchandise, using pathological markers of disease as references of benefit, in order to justify the mass use of their medical products and interventions (e.g., "statins lower cholesterol levels").
As Joel Kauffman (1937-2015), PhD, put it in his exposé "Malignant Medical Myths" (2006):
"[...] medical providers, and the public are easily fooled by the effect of drugs on some easily measured symptom whose significance has reached the level of folklore (myth). Many interventions are justified on conveniently measured parameters, such as bone density, cholesterol level, EKGs, and blood pressure." [119] [emphasis added]
Symptom manipulation is proof of therapeutic benefit or a "cure" according to disease-focused consensus medicine which in reality more often than not plays out as the ongoing management of disease (although in certain cases this might be the most feasible option). The spotlight on the manipulation of disease symptoms (markers of disease) with therapeutic regimes is a traditional trait of organized medicine. (I've written also about this topic in my article "Tougher Supplement Regulation: A Necessity Or Politics?" –direct link to it at the end of this article under Recommended next page(s).)
The purported cardiovascular health benefits of statin drugs are said to rest on their cholesterol-lowering effect –an "easily measured symptom, called the surrogate endpoint" [119]. A surrogate marker is a measured substitute that is assumed to be associated with a specific outcome. As an example, the idea that a high cholesterol level increases the odds of a heart attack and death (the cholesterol-and-heart attack theory).
So, the alleged immense cholesterol benefits of statins are deducted from the manipulation of a marker or symptom of disease (i.e., a high cholesterol reading), via the poisoning of cholesterol biosynthesis, while, in actuality, these cholesterol-lowering medicines were found to have a "98% clinical failure rate" and increase morbidity and mortality [110-124,126,127,333,344].
The same pseudo-science or medical quackery, which the traditional medical officialdom calls "evidence-based medicine" (EBM), is at work with formally sanctioned cancer drugs based on precepts of that bogus science model. Two out of three cancer drugs authorized by the US government between 2008 and 2012 received approval on the basis of surrogate endpoints [362]. After several years of follow-up no tangible benefit (i.e., longer survival) was recorded for more than 85% of the surrogate endpoint-based medications [362].
Diabetes drugs are developed and approved because they lower blood sugar levels (according to many, sugar is the purported "cause of diabetes") without a clear science-based understanding of the medications' systemic physiological effects in the body [249]. The glucose-lowering effect of some of the most widely used and "safety"-approved diabetes medications, such as Avandia (rosiglitazone), Orinase (tolbutamide), or Actos (pioglitazone), were shown to increase heart failure, myocardial infarction (=heart attack), cardiovascular mortality, and bladder cancer [249].
In a study paper by German researchers who compared the marketing literature for therapeutic products versus the scientific literature in alleged support of the interventions, they wrote:
"If study citations can be found in the promotional material, the selection of references is usually limited to those studies that offer at least some indications or aspects in favor of the advertised product." [250] [original article in German: translation & emphasis mine]
In their writeup on garcinia cambogia side effects, another marketing site of the natural weight loss product stated regarding the use of these "natural" nutritional supplements that, "If there’s anyone who would greatly benefit from this, diabetics will be it" despite the concurrent admissions in the article's content that "the results linking diabetes and garcinia cambogia remain inconclusive" and "diabetics are highly advised to take the diet supplement with caution".
Striking Similarities Between Garcinia Cambogia Side Effects And Pro-Diabetic Statins' Side Effects
"The higher the interest of the establishment, the lower our
interest. The more the authorities recommend something, the greater our
health is at risk." (Ghislaine Lanctôt, MD, in "The Medical Mafia", 2002
Edition)
For many years, statin drugs have been among the
most recommended, the most extensively used, the most heavily marketed,
and the most lucrative medical products on the planet [110,111,251].
The
statin medication Lipitor (atorvastatin) had reached the status of "the
world’s best-selling drug" [110]. Statin cholesterol drugs have attain the
accolade of "the most prescribed pharmaceuticals in history" [125]. The
statin industry earns 20 billion dollars in annual revenues as of 2013
[251]. In 2015, many millions of healthy people worldwide continue to
take cholesterol-lowering statin drugs [127], such as Zocor and Lipitor
statins.
Yet, it had been well-established that (at least some)
statins, the biggest moneymakers in the history of the medico-pharma
business, notably increase the risk of diabetes mellitus (this
includes a link between atorvastatin/Lipitor and diabetes)
[111,124,137,251-260,341-343,365-367].
The statin-diabetes link is true for both:
- allegedly sick people (e.g., with so-called cardiovascular issues such as “high cholesterol”) who had been put on statins [137,253,254,256,260,342,365,366] and
- healthy people who took statin cholesterol meds [343,367].
As an example of the latter, one such study, examining the notion of “statins for primary prevention”, reported a doubling of the diabetes risk (plus typical complications with diabetes) in healthy statin users without experiencing offsetting cardiovascular benefits [367].
The unscrupulous allopathic medical industrial complex, of course, has been trying to tap into the vast profit market of healthy people with the use of verified toxic statins [124,368,369] –justified on the entirely dogmatic, scientifically unfounded claim of “primary prevention” of disease (e.g., the primary and secondary prevention of coronary artery disease [372]) with hyped up claims such as “statins are the best life insurance against atherosclerotic events” [371] (based on the fallacious cholesterol theory of heart disease [251,368,369]).
The just cited statins-diabetes study [367] which negated the medical dogma of primary disease prevention with statin drugs showed, in essence, that statins do much more harm than good in healthy people (i.e., statins cause diabetes and proffer marginal or zero benefits). Basically, that is nothing else but to seriously poison and damage unsuspecting healthy people.
The US Food and Drug Administration (FDA), by the way, belatedly alerted the public about the highly noteworthy statin-diabetes association in early 2012 [261] after pertinent scientific study findings of potential diabetogenic activities of statins had already been published back in 2004 [262]. In 2012 the federal agency decided to make the addition to statin drug labels that these medications can cause diabetes [261].
Nonetheless, all of the disturbing relevant evidence on the statin-diabetes link hasn't stopped the Canadian Diabetes Association (CDA) from recommending in their 2013 diabetes guidelines that all patients with diabetes, age 40 and above, take statins [263,264], claiming that with statins "there is little safety concern for their long-term use" [264]. Other authoritative diabetes organizations did not stray far from such advice, as the American Diabetes Association's guidelines, had advocated very similar statin recommendations for diabetics. The FDA, too, had issued encouraging statin use propositions in their statin-diabetes type 2 information releases (despite of its 2012 announcement that statins are causing diabetes) because of the drugs' alleged heart benefits ("FDA continues to believe that the cardiovascular benefits of statins outweigh these small increased risks." [261]).
The medical Powers-That-Be primarily justify statin therapy in terms of vasculo-protective effects, such as the prevention of non-fatal myocardial infarctions and coronary artery disease (clogging of arteries/clogged arteries or atherosclerosis), supposedly because of its cholesterol-reducing property.
Yet, while diabetes is associated with a higher risk of developing cardiovascular disease (CVD), long-time independent statin drugs and cholesterol researcher Uffe Ravnskov, MD, PhD, author of many scientific papers and books exposing false statin and cholesterol beliefs (e.g., the cholesterol myth that "cholesterol causes heart disease"), documented the various study data validating that high cholesterol (hypercholesterolemia), specifically high serum LDL cholesterol, isn't a risk factor for heart disease in diabetic patients [265].
A similar account was voiced by Dwight Lundell, MD, a former heart surgeon, back in 2012:
"I trained for many years with other prominent physicians labelled “opinion makers.” Bombarded with scientific literature, continually attending education seminars, we opinion makers insisted heart disease resulted from the simple fact of elevated blood cholesterol. The only accepted therapy was prescribing medications to lower cholesterol and a diet that severely restricted fat intake. [...]. It Is Not Working! These recommendations are no longer scientifically or morally defensible." [352]
As aforementioned, both garcinia cambogia extract supplements and statin drugs disrupt endogenous cholesterol synthesis, triglyceride production, and lower leptin levels.
(Both statins and garcinia cambogia side effects on cholesterol production are initiated enzymatically. Statin cholesterol medicines disable the enzyme HMG-CoA reductase [115], garcinia cambogia extract debilitates the enzyme ATP citrate lyase. The suffocation of these enzymes leads to reduced levels of essential substrates for the internal production of the free form of cholesterol, mevalonate in the case of statins [115,120] and acetyl-CoA in the case of garcinia cambogia extract [20]. By the way, acetyl-CoA is part of the material that gets converted to HMG-CoA reductase (along the mevalonate pathway), so GCE interrupts cholesterol biosynthesis further upstream in the cholesterol pathway than statins (see Fig. 7).)
The intake of these two agents, statins and garcinia cambogia extract, causing the unhinging of cholesterol production, seems particularly ill-advised and highly dangerous in diabetics because:
- in diabetes cortisol levels are elevated [56] and cortisol depletes cholesterol [266], and
- a suspension of cholesterol synthesis in beta cells of the pancreatic islets inhibits their release of insulin [136,245,246], and the curtailment of insulin secretion is among the acknowledged side effects of statins that are associated with of a higher diabetes risk [130] (see Fig. 8).
The threat of diabetes 2 from the corruption of cholesterol synthesis, via statin or garcinia cambogia side effects, might be higher in women because animal experiments found that pharmacological amounts of estrogen (specifically estradiol) activates the LDL receptors in the liver, increasing intracellular LDL cholesterol uptake (see Fig. 4), leading to blood hypocholesterolemia (notably increased mortality was the adverse outcome after the induction of a low serum cholesterol state) [131]. So-called natural hormone replacement therapy with estrogens has long been strongly associated with heart disease, breast cancer, and other morbidities in women [26]. Some human data (e.g., a subanalysis of the JUPITER study [252] using rosuvastatin, brand name "Crestor") corroborate a significantly increased gender-specific risk of developing full-blown diabetes with statin drug therapy [127,265,267].
Plasma cholesterol's capability to sequester and neutralize endotoxins (LPS) from the gut microbiota, and numerous toxicants (e.g., carcinogenic chemicals) and injurious agents (e.g., noxious microbes) makes the substance an essential agent of detoxification and important immune system modulator, protecting the body, and especially the brain, from harmful poisons and inflammatory attacks [125,127,268,333,336] (see Fig. 4).
DIMINISHED levels of blood LDL cholesterol are linked to a HIGHER incidence of viral infections, respiratory disease, liver disease, and cancer [127,333,340]. LPS (endotoxins) are associated with considerable genomic damage (i.e., DNA strand breaks) [346].
Pneumonia rates are higher in people who received statin therapy compared to untreated controls [269]. An observational study found that Type 2 diabetics who are on statins and got admitted to a hospital for Covid-19 coronavirus respiratory disease had a significantly higher mortality rate compared to those not taking statin medications [374].
Nefariously, it appears that statin drugs actually increase the risk of infection in a hybrid highly self-serving sequence:
- they reduce the blood cholesterol condensation, which weakens immunity against inflammatory-infectious compounds;
- this enables drugs to broadly roam around in the organism via the blood stream in a more unrestricted manner (particularly with prolonged treatment with statin medications), causing infectious injuries because statins are fungal poisons (yeast toxins) [111]. (While cholesterol-decreasing statin therapeutics typically target the liver, the drugs do enter the general blood circulation.)
The significance and clinical observation that statins are linked to a
variety of inflammation-mediated autoimmune diseases (e.g., chronic fatigue
syndrome, arthritis, multiple sclerosis) [111] should hardly come as a
surprise but should be a logical expectation.
Conceivably, the
increase of the body's exposure to toxicity (promoting, for instance,
liver inflammation) by the destabilization of the endotoxin-cholesterol
axis induced via cholesterol-altering statins or garcinia cambogia side
effects, is probably magnified by the potential simultaneous reduction
in the synthesis of bile salt, a very cholesterol-rich material that
serves as an integral agent of detoxification (see Fig. 4, 7 & 8).
These
biological mechanisms (i.e., these specific ramifications of adverse
garcinia cambogia side effects) could reasonably account for, at least
as contributing factors, the past cases of liver injury that were linked to, for example, the Hydroxycut brand of garcinia cambogia slimming products –above and beyond of explanations that put the blame on issues of product contamination. A more current case of severe liver damage that has been linked to a non-Hydroxycut garcinia cambogia brand is recorded in the medical literature. It is the case of a woman who after consuming the supposedly "safe" weight reduction supplement for a few weeks came down with acute hepatitis and, subsequently, acute liver failure (that ultimately required a liver transplantation), pathologies which evidently were traced to garcinia cambogia side effects [361].
By the way, akin to toxic garcinia cambogia side effects concerning the liver, damage to this organ is also among the scientifically confirmed, serious adverse statin side effects [111,251], indicative of the physiological proximity of metabolic action of the two agents and their overlapping biological profiles.
In close relationship to the
diabetic metabolic syndrome, LPS are capable to produce metabolic
endotoxemia, a condition hallmarked by low-grade inflammation (engaging
apoptotic events) that can lead to a reduction in insulin secretion and
insulin resistance, and atherosclerosis [322,323,336] (signifying
another mechanism to promote atherosclerotic development besides through
the repercussions of the augmentation of LDL cholesterol content inside
tissues, as seen with statins [discussed earlier]). People with type 2
diabetes mellitus carry a much larger LPS load in their blood than
healthy people [336]. A high-fat diet (of refined foods high in fats) chronically and strongly augments
the plasma endotoxin content [322,323,336] (see Fig. 8).
Because
the development or causes of diabetes mellitus are strongly associated
with inflammatory damage from stressors (see the section "The Principal
Clinical Features Of Diabetes", particularly Fig. 1), such as various
types of toxins and noxious agents (encompasses diet-based omega-3 side
effects), the inhibition of cholesterol biogeneration, whether by
garcinia cambogia weight loss pills or statins (see Fig. 7), kindles the
development of the metabolic disease called "diabetes".
The
essentiality of cholesterol in the brain is further demonstrated by the
fact that the organ contains the highest cholesterol concentration
(around 25%) of any tissue in the human body [125,265] and that the
material is indispensable in the formation of functional synapses
[265,270].
A short-term human study (lasting 10 weeks) with
garcinia cambogia extract supplements failed to record a
cholesterol-depressing effect of the product in terms of plasma total
cholesterol [271]. In an animal study of similar short duration (12
weeks), however, it was observed that the administration of HCA-garcinia
cambogia diet pills significantly lowered blood cholesterol (and
triglyceride) levels compared to the control group [108]. A 12-week long
human trial using garcinia supplements combined with a fiber-rich
botanical also found that the concentrations of total cholesterol and
LDL cholesterol were significantly reduced in comparison to the placebo
arm [272]. And, the human consumption of nutritional supplements of HCA
garcinia cambogia extract, not combined with other diet products, over 8
weeks –using a decidedly higher dosage (although deemed "safe for human
consumption" [273]) of the active GCE ingredient hydroxycitric acid
(i.e., 2,800 mg/day of HCA [84]) than in the experiment of the Kim team
[271])– was shown to strikingly decrease total blood cholesterol
content, LDL cholesterol, and triglyceride levels [84,274].
As
alluded to earlier, the decline in the secretion of insulin (found among
both statin and garcinia cambogia side effects) is postulated to be a
consequence of increased pro-inflammatory and oxidative effects on
ß-cells from an amplified intracellular inflow of blood-derived LDL
cholesterol, all of which is an outcome of the hampering with
cholesterol production.
Remember that another related possible
mechanism that had been proposed of why the strangulation of internal
cholesterol biosynthesis is dangerous and can contribute to or cause
diabetes centers around the fact that cholesterol is a required substance for proper beta cell function,
and that the disruption of endogenous cholesterol genesis in beta-cells
ensues in a noticeable reduction of insulin secretion from pancreatic
islets [246] (see Fig. 4).
The dangers of statin drugs have many
people motivated to seek out natural cholesterol remedies or "natural
statins" for high cholesterol levels. A popular statin alternative is
Chinese red yeast rice (sometimes mistakenly referred to as red rice
yeast). Red yeast rice contains naturally occurring statins
[117,324,327,330].
However, these natural statins in red yeast
rice supplements:
(A) don't typically reach the pharmacological dosage level
of commonly prescribed statin drugs, and
(B) red yeast rice supplements
consist of numerous cardio-beneficial nutrients (e.g., coenzyme Q10),
thus, red yeast rice therapy appears notably less dangerous –or quite
safe– compared to statin medicines yet probably ought to remain a real
concern because...
(1) the natural health product does significantly reduce
both total cholesterol and LDL cholesterol levels,
(2) inhibits cholesterol
production in the liver,
(3) has been tied to known statins' side effects
(e.g., neuropathy, myopathy, rhabdomyolysis),
(4) hasn't been rigorously
studied in controlled long-term trials, and
(5) because serious statin side
effects can come about over time even at a low dosage (e.g., low-dose
statin therapy, lasting more than 5 years, was associated with much more
cancer deaths) [324-330,333] (see Fig. 8).
After all, all
statins are toxins made by fungi –and yeast is a fungus. (All statin
drugs are known disease-causing mold poisons (fungal toxins, a.k.a.
mycotoxins) [111].)
Moreover, and in view of that in
diabetes sugar levels are high as a rule, statin cholesterol drugs, just like
HCA-garcinia cambogia extracts, block insulin secretion from the pancreas (by disrupting and damaging beta cell function) and block cellular glucose uptake
(i.e., glucose transport via Glut proteins), resulting in hyperglycemia
[137,239,251,253,275,276] (see Fig. 4 & 8). In their lengthy
biomedical paper on conventional cholesterol treatment, the authors
commented that one of the ways statins cause an increase in the
incidence of diabetes is by "decreasing glucose consumption" [340] –one
of the well-described garcinia cambogia side effects.
In
addition, cholesterol researcher Uffe Ravnskov, MD, PhD, had illustrated
the life-saving essential quality of cholesterol and the importance of
the body's unhampered ability to produce the material, when he remarked
that:
"[...] more than twenty studies have shown that elderly
people with high cholesterol live longer than elderly people with low
cholesterol." [265]
And ironically, a high level of the allegedly “bad” cholesterol (LDL cholesterol) signifies a lower death rate, meaning higher longevity, in the majority of people over 60 years of age [368].
In observance of the known scientific facts, the (artificial) blockade of the body's natural production
of cholesterol (at a pharmacological strength grade), either via pharmacotherapy (e.g., with prescription drugs such as statins) or a heavily concentrated
single-nutrient botanical ingredient (e.g., garcinia cambogia
hydroxycitric acid) –or, conceivably, a few specific, notably
concentrated, botanical substances– is potentially (seriously)
problematic.
Another one of the garcinia cambogia side effects
associated with diabetes agitation bears great resemblance to a
pro-diabetic action of statins: while garcinia cambogia supplements
inhibit the ATP citrate lyase protein, statin cholesterol meds enhance the
inactivation of ATP citrate lyase [147], quintessentially acting as
some sort of garcinia cambogia catalyst. Both events decrease cell
proliferation and increase apoptotic beta-cell loss (see Fig. 4).
(Remember that ATP citrate lyase is commonly low –i.e., inhibited– in
diabetics [20,146].).
Diabetes medication treatment with the widely used
sulfonylureas (a class of diabetes drugs) including Orinase
(tolbutamide), were shown to promote ROS/NO-induced beta-cell apoptosis
in healthy pancreatic islet cell lines [277-280].
Besides intense
cholesterol depletion and the killing of beta cells other diabetogenic
activities of statin therapy match certain garcinia cambogia side
effects. The scientific findings about the toxic impact on triglyceride
synthesis by statin and garcinia cambogia side effects remarkably mirror
each other. Statin studies found that in those people whose
triglyceride was the most reduced had the highest all-cause mortality [281]. In juxtaposition, research data uncovered that the lower the content of FFA-induced triglycerides in pancreatic beta-cells the higher the percentage of beta-cell eradication [149].
The
disturbance of the normal biological function of cells is another
commonality between adverse statin effects (statin poisoining) and
garcinia cambogia side effects. Statins can adulterate the mitochondrial
energy system [125,282], leading to the dysfunction of the
mitochondria, inflammation of the pancreas (pancreatitis) and pancreatic
dysfunction [283-287] –attributions that, by and large, quite closely
match the diabetogenic garcinia cambogia side effects outlined in this
article.
For instance, LPS-endotoxins inhibit mitochondrial
respiration [345], and both side effects from statins and garcinia
cambogia side effects involving cholesterol biosynthesis lead to an
increase in blood endotoxin exposure (as discussed).
The rather broad similarity of adverse properties supports the reasonable premise that taking both
garcinia weight loss pills and statin medications together (eliciting
statin drug interactions with garcinia cambogia extract),
synergistically raises the risk of developing or promoting diabetes (or
complications with diabetes) via a number of delineated statin-garcinia
cambogia side effects (see Fig. 8).
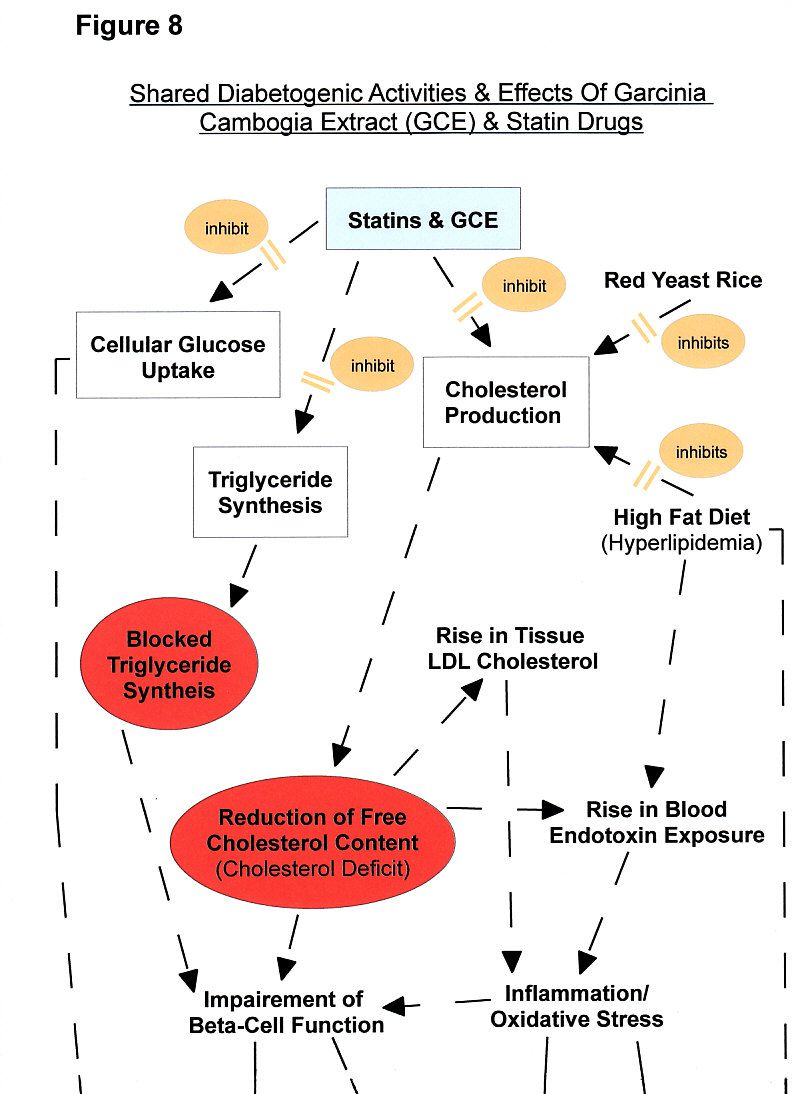
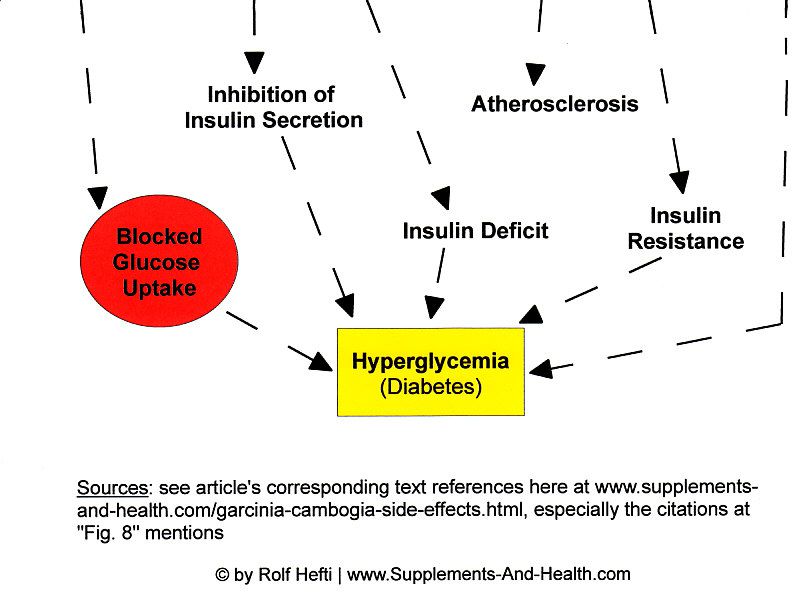
Also, one of the adverse statin drug side effects is rhabdomyolysis, a
muscle disorder that leads to the breakdown of muscle tissue,
manifested by muscle pain (myalgia) and weakness in the extremities
[110,115,251]. (Many people have been killed by statin drug-caused
rhabdomyolysis [335]). I reckon this adverse statin side effect might be
behind the observed connection between Lipitor and back pain as the
unpleasant condition frequently affects back muscles. And, other types
of back tissue accounting for back pain, could be a target for statins (such as Lipitor) as well because statin cholesterol medicines poison the energy system
of cell mitochondria [125,282], and mitochondrial dysfunction, oxidative
stress, and a pro-apoptotic pattern are tied to back disc degeneration
[331,332].
A few cases of rhabdomyolysis had been recorded in the
medical literature and linked to Hydroxycut side effects (Hydroxycut,
as you may recall, is a particular garcinia cambogia-HCA dietary
supplement) [5,288]. A reasonable explanation for the fat-burning
garcinia diet supplement's potential capability of invoking such damage
is by its amplification of inflammatory-oxidative stress (e.g., "free
radical attacks", endotoxin activation), via lipolysis activation, the
promotion of fat metabolism, the degrading of mitochondrial respiration,
and the strong stimulation of intracellular consumption of plasma LDL
cholesterol. Because both with standard statin therapy and,
specifically, in statin-induced rhabdomyolysis cases, one of the
empirically documented statins' side effects is (acute) pancreatitis
[283,285,286]. In models of acute pancreatitis, the destruction of
pancreatic tissue can occur via the induction of apoptosis [289].
The
manifold overlapping or shared adverse statin effects and garcinia
cambogia side effects pose another serious, albeit largely covert,
concern. Specifically, I'm referring to the potential drawn-out time
frame in which both statin and garcinia cambogia side effects manifest
themselves in clinical symptomatology and morbidity.
Peter Langsjoen, MD, raised awareness about that when he stated:
"Statins
may be the perfect and most insidious human toxin in that adverse
effects are often delayed by years and come about gradually." [290]
Statin or garcinia cambogia side effects may sneak up on the products' users sort of like a thief in the night.
Why Do Medical Authorities & Other Recognized Health Experts Make Health Claims In Favor Of Products And Procedures That The Actual Scientific Data Don't Support?
"[...] perception requires interaction with the object [...]." (Ray Peat, PhD, 1936-2022, US Biologist, in 1976)
The expression "knowledge is power" [291] has become common use in many societies but knowledge (or information) is only real power if it is accurate, known, accepted, and applied.
Acquiring and verifying knowledge means active participation, as in a pro-active search for, or exposure to, various types and sources of knowledge. This is particularly a necessary requirement in today's authoritarian corporatism-dominated cultures that are widespread across the globe. The application of perceived information calls for the initiation of action.
This means that the elements of knowledge potential, that is...
- the acquisition of awareness about information,
- the verification of the validity of the information, and
- the acceptance and utilization of information
... demand active personal involvement (i.e., a conscious effort).
Typically, traditional physicians don't critically examine the original medical literature for themselves when making decisions and patient recommendations about various therapeutic products and interventions [250,292-294].
Is there any reason, or good evidence, at hand to think that this would be any different with the towering Dr. Oz or most other (highly publicized) medical doctors or popular media pundits from the world of media medicine when recommending medical products or alternative health products?
An individual educated as both a medical doctor and a scientist, Michael Anchors, MD, PhD, proffered an explanation as to why doctors don't usually read the scientific literature:
"[...] few physicians read clinical studies [...]. Few know how. The skill is not taught in medical school. I was trained as both an M.D. and a Ph.D. I have seen both patterns of education. [...]. Doctors [...] get their information from the people who give them notepads and stethoscopes. American doctors are not paid to study; they are paid to work. [...]. [...] the only way to become a real expert is by reading scientific evidence." [294]
This strengthens the notion that a major role of a physician is as an (unwitting or witting) sales tool of the corporate industry he/she belongs to (i.e., allopathic medicine) rather than as a carrier of accurate scientific knowledge (i.e., "a real expert") about the true value of the medical regimes he/she administers or prescribes to patients.
The lack of most traditional medical doctors to pro-actively investigate the evidence on therapeutic interventions sanctioned and commissioned by the leadership of their affiliated medical industry body, or the popular culture, is further evident in their unwitting acceptance of numerous medical myths as solid facts.
In a 2007 publication of the British Medical Journal, two physicians reported after an examination of the medical literature that many popular beliefs, commonly accepted even by many medical doctors, were either unproven or untrue [295].
Among the often-held assumptions or "common knowledge" the study authors scrutinized were beliefs such as "You need 8 glasses of water a day" or "eating turkey makes you drowsy" [295] –notions which years later are still widely accepted by many individuals as factually accurate. (An aside: The "turkey-drowsiness" belief is based on the notion that the amino acid tryptophan is responsible for the effect because turkey is among the foods high in tryptophan. In my article "Tryptophan For Sleep –One Of The Good Natural Sleeping Aids?" I presented research data on tryptophan supplements, which typically contain much higher amounts of the nutrient than what's available in food items, that showed the products aren't particularly helpful for insomnia, making it rather unlikely that this substance is the predominant culprit for the drowsiness effect some people have experienced when eating tryptophan foods such as turkey.)
Study author Rachel Vreeman, MD, noted that:
"[...] staying current is not just a matter of adding new knowledge onto the things we already believe. Sometimes you really have to look back on things already in your head or things you already believe to be true, and reinvestigate, or investigate for the first time, whether those things are true.”
And co-study author Aaron Carroll, MD, opined that:
“Until someone takes the time to question and look for evidence, medical myths will remain accepted beliefs."
Instead of actively perusing the original scientific literature in the conception of practice guidelines and the provision of useful therapeutic medical advice for patients, the majority of conventional physicians rely on, or act based on:
- the information they receive from salespeople of the pharmaceutical companies or from hospital consultants,
- condensed synoptic versions of research findings disseminated by medical societies and professional medical trade organizations, or newspapers,
- self-serving economic incentives, or
- a need to be liked by patients [250,292,293,296,297].
But frequently, and exemplifying a perpetual global issue, the messages and information contained in pharmaceutical marketing literature, dispensed by drug industry representatives (or through other means such as (online) direct-to-consumer advertising (DTCA) by drug companies [298,299]), or the study abstracts of medical publications, don't correlate with or reflect the true scientific facts contained in the body content of the original study papers or the drug advertisements don't contain any research references at all –and, in the context of an obvious conflict-of-interests (vested interests), a large portion of the "scientific" studies aggregated in the medical literature is funded by the business of orthodox medicine itself so that deception, as in the fabrication of critically biased or fraudulent research data in favor of medical interventions, is quite common [110,118,119,124,127,249,250,265,300-312,340,344,370].
In "Malignant Medical Myths" (2006) author Joel M. Kauffman (1937-2015), PhD, wrote:
"While many physicians and other medical providers mean well, the information they use to make recommendations for many common conditions is often outdated, biased, flawed, and sometimes is based on outright fraud. Many medical tests and treatments are not based on sound research [...] but on the pitches of opinion leaders paid by those who would profit from their use." [119]
Drawn from their investigative data published in 2004 [250], some German scientists explained that three primary areas in the manipulation of facts ("Faktenmanipulation") account for the discrepancy between medical product advertisements and the actual scientific data contained in original study publications:
- a false rendition of study content,
- a constriction of crucial information presented in the cited studies (e.g., the scope of drug side effects), and
- the manufacturing of statements that cannot be found in, or comply with what's been furnished in, the original study papers (e.g., claims of remedial benefits are inflated).
These observations had been documented for a very long time in the medical research literature, and the investigative findings the German scientists had established are still completely applicable and fact-based a decade later [124,249,309] –and thereafter.
Indicating the ample depth of the corrupt mainstream medical system, it should be kept in mind that the problem of "Faktenmanipulation" is even more complex, pernicious, and overlapping in terms of industry claims and study data. Simply because the real dangers of a lucrative product or intervention, or other opposing clinical data jeopardizing their sales, are frequently inadequately quantified or mentioned in the actual research studies or notable eligible studies with negative findings never even get published [115,118,119,124,127,132,249,265,281,302,304,308, 312,313,370], producing, what is known as, "publication bias".
A personal admission of Michael Anchors, MD, PhD, in 2012 contests to that:
"Nowadays, most research projects at the NIH [=U.S. National Institutes of Health], where I used to work, are NIH/pharma company partnerships. The content of the big studies legally belong to the pharmaceutical companies. They can publish it, alter it or suppress it at will. What do you suppose they do?" [294] [explanation added]
A good illustration of the discrepancy between medical claims and the medical literature are psychotropic medications, such as the SSRI antidepressants, which are based on the serotonin theory –that is, the authoritarian dogma that serotonin is “the happy hormone”. SSRI drugs, such as the renowned medication Prozac, to supposedly treat "the serotonin blues", have long been blockbuster goods for the big business of modern medicine, having enjoyed a steep commercial ascent during the 1980s and 90s.
Notwithstanding, in 2005, for example, two researchers wrote in their study paper published in the journal PLOS Medicine:
"The incongruence between the scientific literature and the claims made in FDA-regulated SSRI advertisements is remarkable, and possibly unparalleled." [339]
Despite that the actual serotonin truth deviates from the serotonin myth (i.e., serotonin is "the happiness hormone"), the medical profession has been widely promoting and, thus, hugely profiting from the utilization of the officially validated SSRI medications to this day.
(For further information on the serotonin-depression mantra and the side effects of tryptophan and serotonin see my essay "Tryptophan Side Effects: L-Tryptophan Is Far From Harmless" (direct link to it at the end of this article under Recommended next pages.)
To take another example of the orthodox medical fraternity: statin drugs, which are among the best sold and most widely consumed medications in industrialized nations. As broadly prescribed medications they've been sanctioned by research data of "evidence-based medicine" and are government-approved for safety and efficacy. Modern corporate medicine had pronounced that statins are "wonder drugs" or "miracle drugs" and are "the most powerful inventions to prevent cardiovascular events" (based on the cholesterol-heart disease hypothesis, a disproved medical dogma) as well as other claims [115,127].
In a review paper of officially deemed "substantial" evidence-based studies (e.g., randomized controlled trials) relating to "cardiovascular primary prevention" and "statin side effects" the authors wrote:
"There is a categorical lack of clinical evidence to support the use of statin therapy in primary prevention." [251] [emphasis added]
And...
"[...] there is ample evidence to show that statins actually augment cardiovascular risk in women, patients with Diabetes Mellitus and in the young. Furthermore statins are associated with triple the risk of coronary artery and aortic artery calcification." [251] [emphasis added]
And...
"What is even more disparaging is that not only has there been a failure to report on these negative side-effects of statins, there has actually been active discouragement to publish any negative studies on statins." [251] [emphasis added]
And...
“[...] findings on statin major adverse effects had been under-reported and the way in which they withheld from the public, and even concealed, is a scientific farce.” [251] [emphasis added]
Analogously, in a review study paper of statin trials, the authors (among them the noted independent medical researcher, Uffe Ravnskov, MD, PhD, who had published and written numerous works on statins and cholesterol), concluded with:
"[...] the presentation of statin trial findings can be characterized as a deceptive strategy in which negligible benefits of statin treatment have been amplified with the use of relative risk statistics, and that serious adverse effects are either ignored or explained away as a chance occurrences." [127] [emphasis added]
Some of the most genuine evidence has linked statin drug use with “serious adverse effects”, such as muscle disorders, liver damage, joint problems (e.g., arthritis), cataracts, nerve damage, birth defects, arterial calcification, pancreatitis, erectile dysfunction (“impotence”), low libido/loss of libido, memory loss, brain dysfunction, suicide, violence, diabetes, autoimmune diseases (fibromyalgia, multiple sclerosis, etc.), and with an increased risk of cancer and –as mentioned earlier– with higher mortality (statin cholesterol drugs only slightly lower the risk of non-fatal heart attacks) [110-127,251,253-260,281-286,333,341-344,365-367,370].
As an example, in the statin “CARE trial” (pravastatin study) [373], there was a highly significant increase in the development of breast cancer among statin-treated women compared to women of the control group [115,370] (a disturbing relevant finding that's entirely omitted in the study's abstract and downplayed by the trial's authors in their paper). Even more startling, Uffe Ravnskov, MD, PhD, noted in the year 2000 that, curiously, in subsequent statin studies (after the CARE study) "all patients with cancer [...] have been excluded from the trials" [115]. To deliberately hide a most serious statin side effect?
Here's yet another example of the enormous institutional investment of the industry of modern allopathic medicine in their highly profitable products and services: "preventative" cancer screening tests (e.g., breast cancer screening procedures such as mammography).
The widely disseminated narrative of the ruling medical authorities and the so-called cancer charities has continuously been that early detection by cancer screening "saves lives" and is, thus, highly beneficial.
Yet, the most reliable research data on medical screening, derived from meta-analyses and randomized trials, expose that the mass use of standard cancer detection technologies in asymptomatic (=presumed healthy) adults do little to prevent deaths [315,316]. In other words, the vast majority of traditional "preventive" screening tests do not save lives.
The authors of one of these studies voiced that:
"Among currently available screening tests for diseases where death is a common outcome, reductions in disease-specific mortality are uncommon [...]." [316] [emphasis added]
And, it is also common for randomized studies on cancer screening to omit to properly cite the serious harms from medical screening tests [315,317].
(For more breast cancer information and the actual facts on mammogram screening see my e-book "The Mammogram Myth" –direct link to it at the end of this article under Recommended next pages.)
This knowledge hatches some important questions:
- Are these examples solid proof that the medical marketplace is shaped (i.e., manipulated) in a way to favorably accommodate the commercial interests of big medicine?
- Is this unmistakable proof that the massive traditional medical business has been misleading and hoodwinking the public on a routine basis?
- Is it reasonable to think that the broad use or administration of numerous other "advanced" medical interventions, promulgated as being highly beneficial and as having inconsequential dangers by the mainstream medical establishment, is not warranted by the actual scientific evidence?
The deep realization of these realities about the orthodox medical
enterprise explains such rather discouraging, yet accurate, statements
as that of Ralph K. Campbell, MD, in 2014:
"We should not
accept the contents of an advertisement without examining the facts. But
transparency, by design, is lacking, making it difficult to get at the
concealed truth." [314]
Michel de Lorgeril, MD, a cardiologist and research scientist, described the false medical script of the “statin miracle” and the deceptive “cholesterol saga” as "the most extraordinary medical and scientific scam ever set up in modern and postmodern society" [124].
Alongside propagandized medical "miracle drugs" or "wonder drugs" (and "breakthrough" cancer screening tests) we have, in societies of consumerism, propagandized “wonder supplements” in the form of, for example, "miracle diet pills" such as "breakthrough" or "miracle" garcinia cambogia weight loss supplements or other "research verified" weight reduction products.
In the
research literature on weight loss pills we encounter similar or the
same shady dynamics as described by the German researchers (e.g., the
true health risks of diet pills are underemphasized, minimized, or
disregarded) because, akin to the corrupt situation in medical research,
numerous study investigations on the garcinia cambogia weight loss
products (and other diet pills) are conducted by people with significant
competing moneyed interests (conflict-of-interests) linked to the diet
supplement industry [318]. (One such example is a positive garcinia
cambogia extract study I had mentioned early on in this piece –see
reference #10.)
Unfortunately, these objectivity-compromising vested competing interests among study authors remain most often unacknowledged in the marketing literature and the messages of the vitamin world, such as:
- general product advertisements,
- the information material of product write-ups (e.g., a typical online garcinia cambogia review), or
- the narratives of promotional websites for garcinia cambogia supplements and sales sites peddling "Dr. Oz vitamins" (allegedly not authorized by the famed physician), or of popular medical talk shows such as "The Dr. Oz Show" or "The Doctors" [319].
For example, in the episode of the Dr. Oz TV Show where the famous physician praised the "fat buster"/"breakthrough" diet pill garcinia cambogia extract, one of the featured garcinia researchers is Dr. Harry Preuss [1]. Preuss had authored many garcinia cambogia studies, some of them as the lead author –such as the one I cited in the article you're reading [274]. Yet in that study (and others), Preuss and his co-authors failed to disclose conflict-of-interests (COI), such as between them and the product manufacturer or that the study had been sponsored by the product maker [318]. And, not unlike a domino effect, Doctor Oz, whom many people find very trustworthy, genuine, and convincing, also omitted to mention these relationships in that particular episode of the Dr. Oz TV Show [1].
In corporate cultures where the public is routinely lied to by the "authorities" one also increasingly finds individuals who ask questions like "is garcinia cambogia a hoax?" or "are Dr. Oz's garcinia cambogia claims legitimate?" before committing to official marketing narratives.
What the public most certainly deserves to know, and must know, is that studies compromised by COI "may over-state product safety and effectiveness" and that "a lack of funding source declaration reduces validity of findings" [318].
An investigative analysis of the health recommendations and bold statements made in the very successful internationally syndicated Dr. Oz TV Show found that more than half of the advice or health claims (includes the ample sphere of Dr. Oz weight loss tips) were not backed by considerable scientific evidence or were contradicted by research data, and that potential harms of the recommendations were "less commonly mentioned" [319].
Therefore...
Usually, a topic-relevant balanced overview of the scientific literature is missing in the marketing material and messages for both medical and alternative therapeutic products and procedures, challenging or obstructing the ability of the general public for informed decision making.
The currently (2014/2015 and prior years) existing (total) lack of reference to pertinent medical evidence on pro-diabetic garcinia cambogia side effects in the commercial announcements for this diet supplement, whether in print material, on television, online, or otherwise, is in line with this overall trend in commercialized societies.
Concluding Thoughts On Diabetes-Activating Garcinia Cambogia Side Effects
"[...] if a scientific hypothesis is sound, it must agree with all observations. A hypothesis is not like a sports event, where the team with the greatest number of points wins the game. Even one observation that does not support a hypothesis is enough to disprove it. The proponents of a scientific idea have the burden of proof on their shoulders. The opponent does not have to present an alternative idea; his task is only to find the weakness in the hypothesis. If there is only one proof against it, one proof that cannot be denied and that is based on reliable scientific observations, the hypothesis must be rejected." (Uffe Ravnskov, MD, PhD, Independent Researcher)
According to official diabetes type 2 information published by the Centers for Disease Control and Prevention (CDC) in 2014, diabetes mellitus type 2 affects a bit over 29 million people (or around 10% of the population), of which roughly 28% are undiagnosed [12]. Moreover, 86 million people have prediabetes (sometimes called "impaired glucose metabolism") whereas 90% of them don't know they have the condition [12]. Millions of adults have the metabolic syndrome that predisposes them to diabetes and other chronic degenerative diseases [90].
An adult diabetic has a 50% greater risk of death than an adult without diabetes [12]. Having diabetes greatly increases premature mortality from heart disease (e.g., heart attacks), stroke, infectious diseases, certain cancers, and suicides [12,320]. Per data from 2010, diabetes is a top leading cause of death in the US [12].
One revealing implication of these data: since statins are among the causes of diabetes mellitus and diabetes significantly increases the risk of cardiovascular disease (e.g., atherosclerosis, deaths from heart attacks), statins cause the very disease official licensed medicine alleges these drugs will prevent. This chain-of-events would coherently explain (at least in part) the data that statins are notably associated with increased cardiovascular disease events [251,334,360].
Diabetes is also associated with a higher incidence of renal failure, blindness, lower-limb amputations, and mental disorders [12,320].
So, is it safe for diabetics to take garcinia cambogia extract?
The research data chronicled in this treatise, per my understanding thereof, do not confirm at all that there are no serious garcinia cambogia side effects, that garcinia diet supplements are safe, or that they offer benefits for diabetics and ought to be recommended for them (i.e., a diet for diabetes should not include the consumption of HCA-garcinia cambogia extract).
In short, the hypothesis or notion that garcinia cambogia extract is a beneficial agent for diabetes is not scientifically "sound" (see Ravenskov's quote at the start of this section).
Instead, the information suggests with rather compelling significance that in diabetics (or prediabetics), in obese or overweight individuals, or in people on a high fat diet (of highly processed foods), whose ATP citrate lyase index is traditionally low from an increase in blood fats, garcinia-hydroxycitric acid, by way of...
- ATP citrate lyase inhibition,
- its reduction of both insulin and leptin,
- its interference with triglyceride and cholesterol production, and
- its re-direction of optimal energy fuel consumption,
... is likely to lead to the (further) disruption of insulin release, hyperglycemia, and the promotion, or initiation, of oxidative stress in the brain and pancreas, and ß-cell failure or destruction. Therefore, the regular consumption of HCA-laden garcinia cambogia extract isn't a general viable modality among therapeutic interventions for diabetes. (Keep in mind that some of the data on the significant statin-diabetes connection also revealed that the diabetes risk increases in relatively healthy and presumably very healthy people who've been eating the drug over an extended period of time [343,367], which doesn't exempt the possibility that diabetes-inciting garcinia cambogia side effects raise that risk as well).
Last but not least, the exploration of diabetogenic garcinia cambogia
side effects begs the question whether other "magic" or "miracle diet pills" and slimming supplements that
operate physiologically as a "fat burner" may have comparable
(unacknowledged) degenerative consequences.
And ironically, as far as garcinia cambogia benefits go –and alleged benefits of diet supplements in general– positive weight loss effects might conceivably not be primarily due the actual ingredients disclosed on the labels of the diet products. Rather, the purported slimming benefits could possibly be the result of therapeutic pharmacological drugs (or other materials) that are not disclosed on the supplement ingredient labels. Because (“miracle”) diet supplements are among the top contaminated supplements on the (US) market (see my article "Health Risks From Dietary Supplements | Contaminated Supplements" –direct link to it at the end of this article under Recommended next pages). One could call this a little-known ugly truth about diet supplements.
In summary, in the very people garcinia cambogia weight loss diet pills are typically recommended for –that is, overweight or obese people both of whom have an increased diabetes risk or are frequently diabetics– the weight loss product should probably not be used (particularly on a long-term schedule) because garcinia cambogia side effects are likely contributing to the development of diabetes (or prediabetes), or are exacerbating an existing diabetic state.
(Originally published: 20-April-2015 | Revised: 2-Aug-2021)
(To stay up-to-date on the release of my very latest articles subscribe to my Free Newsletter)
===================
Recommended next page(s):
===================
- Tryptophan Side Effects: L-Tryptophan Is Far From Harmless
- Health Risks From Dietary Supplements | Contaminated Supplements
- Side Effects Of Dietary Supplements | The Dangers Of Supplements!
- Facts About Dietary Supplements: Supplement-Drug Interactions
- Mammograms: Dangerous! Mammography Risks, Myths & Breast Cancer Facts ("The Mammogram Myth")
- Tougher Supplement Regulation: A Necessity Or Politics?
========================================
Article
Index On The Politics Of Nutritional Supplements
-How You Get Deceived & Misled
-Revealing Hidden Facts About Vitamins & Supplements
========================================
References
- https://web.archive.org/web/20121107130235/
http://www.doctoroz.com/videos/garcinia-cambogia-newest-fastest-fat-buster-pt-1 & https://www.youtube.com/watch?v=xWUpTfQwU4k [accessed 1-Jan-2015] - Sullivan AC, Singh M, Srere PA, Glusker JP, "Reactivity and inhibitor potential of hydroxycitrate isomers with citrate synthase, citrate lyase, and ATP citrate lyase", J Biol Chem. 1977 Nov 10;252(21):7583-90.
- Jena BS, Jayaprakasha GK, Singh RP, Sakariah KK, "Chemistry and biochemistry of (-)-hydroxycitric acid from Garcinia", J Agric Food Chem. 2002 Jan 2;50(1):10-22.
- U.S. Food And Drug Administration (FDA), "FTS-HHS FDA: Hydroxycut Dietary Supplement - FDA Warns Consumers to Stop Using Hydroxycut Products, Risk of Liver Injury", Transcript of FDA's Media Briefing on Hydroxycut Dietary Supplement, www.fda.gov, 1-May-2009
- Carol ML, "Hydroxycut weight loss dietary supplements: a contributing factor in the development of exertional rhabdomyolysis in three U.S. Army soldiers", Mil Med. 2013 Sep;178(9):e1039-42. doi: 10.7205/MILMED-D-13-00133.
- Chuah LO, Yeap SK, Ho WY, Beh BK, Alitheen NB, "In vitro and in vivo toxicity of garcinia or hydroxycitric Acid: a review", Evid Based Complement Alternat Med. 2012;2012:197920.
- Balázs A, "Role of phytotherapy in the prevention and treatment of obesity", [Article in Hungarian], Orv Hetil. 2010 May 9;151(19):763-73. doi: 10.1556/OH.2010.28812.
- Cherewatenko V, Perry P, "The Diabetes Cure: A Natural Plan That Can Slow, Stop, Even Cure Type 2 Diabetes", 1999
- Wielinga PY, Wachters-Hagedoorn RE, Bouter B, van Dijk TH, Stellaard F, Nieuwenhuizen AG, Verkade HJ, Scheurink AJ, "Hydroxycitric acid delays intestinal glucose absorption in rats", Am J Physiol Gastrointest Liver Physiol. 2005 Jun;288(6):G1144-9.
- Talpur N, Echard BW, Yasmin T, Bagchi D, Preuss HG, "Effects of niacin-bound chromium, Maitake mushroom fraction SX and (-)-hydroxycitric acid on the metabolic syndrome in aged diabetic Zucker fatty rats", Mol Cell Biochem. 2003 Oct;252(1-2):369-77.
- Kanzaki M, Pessin JE, "Signal integration and the specificity of insulin action", Cell Biochem Biophys. 2001;35(2):191-209.
- Centers for Disease Control and Prevention (CDC), "National Diabetes Statistics Report: Estimates of Diabetes and Its Burden in the United States, 2014", Atlanta, GA: US Department of Health and Human Services, 2014.
- Warren S, "The Pathology of Diabetes Mellitus", Philadelphia, Lea and Febiger, 1930
- Walker M, "Obesity, insulin resistance, and its link to non-insulin-dependent diabetes mellitus", Metabolism. 1995 Sep;44(9 Suppl 3):18-20.
- Girard J, "Role of free fatty acids in the insulin resistance of non-insulin-dependent diabetes", [Article in French], Diabete Metab. 1995 Apr;21(2):79-88.
- Gerich JE, "The genetic basis of type 2 diabetes mellitus: impaired insulin secretion versus impaired insulin sensitivity", Endocr Rev. 1998 Aug;19(4):491-503.
- Evans JL, Maddux BA, Goldfine ID, "The molecular basis for oxidative stress-induced insulin resistance", Antioxid Redox Signal. 2005 Jul-Aug;7(7-8):1040-52.
- Kahn SE, Hull RL, Utzschneider KM, "Mechanisms linking obesity to insulin resistance and type 2 diabetes", Nature. 2006 Dec 14;444(7121):840-6.
- Peat R, “Glucose and sucrose for diabetes”, Ray Peat's Newsletter, www.raypeat.com, Nov-2009
- Chu KY, Lin Y, Hendel A, Kulpa JE, Brownsey RW, Johnson JD, "ATP-citrate lyase reduction mediates palmitate-induced apoptosis in pancreatic beta cells", J Biol Chem. 2010 Oct 15;285(42):32606-15.
- Szendroedi J, Phielix E, Roden M, "The role of mitochondria in insulin resistance and type 2 diabetes mellitus", Nat Rev Endocrinol. 2011 Sep 13;8(2):92-103. doi: 10.1038/nrendo.2011.138.
- Kleinridders A, Lauritzen HP, Ussar S, Christensen JH, Mori MA, Bross P, Kahn CR, "Leptin regulation of Hsp60 impacts hypothalamic insulin signaling", J Clin Invest. 2013 Nov 1;123(11):4667-80.
- Opie EL, "A Case Of Joslin Haemochromatosis: The Relation Of Haemochromatosis To Bronzed Diabetes", J Exp Med. 1899 May 1;4(3-4):279-306.
- Joslin EP, "The Relation Of Trauma To Diabetes", Ann Surg. 1943 Apr;117(4):607-22.
- Zhang Y, Tatsuno T, Carney JM, Mattson MP, "Basic FGF, NGF, and IGFs protect hippocampal and cortical neurons against iron-induced degeneration", J Cereb Blood Flow Metab. 1993 May;13(3):378-88.
- Peat R, "From PMS to MENOPAUSE: Female Hormones in Context", 1997
- Mattson MP, "Modification of ion homeostasis by lipid peroxidation: roles in neuronal degeneration and adaptive plasticity", Trends Neurosci. 1998 Feb;21(2):53-7.
- Pitocco D, Tesauro M, Alessandro R, Ghirlanda G, Cardillo C, "Oxidative stress in diabetes: implications for vascular and other complications", Int J Mol Sci. 2013 Oct 30;14(11):21525-50. doi: 10.3390/ijms141121525.
- Forbes JM, Cooper ME, "Mechanisms of diabetic complications", Physiol Rev. 2013 Jan;93(1):137-88. doi: 10.1152/physrev.00045.2011.
- Johnston DI, "Management of diabetes mellitus", Arch Dis Child. 1989 Apr;64(4):622-8.
- Taskinen MR, Bogardus C, Kennedy A, Howard BV, "Multiple disturbances of free fatty acid metabolism in noninsulin-dependent diabetes. Effect of oral hypoglycemic therapy", J Clin Invest. 1985 Aug;76(2):637-44.
- Bandyopadhyay GK, Yu JG, Ofrecio J, Olefsky JM, "Increased malonyl-CoA levels in muscle from obese and type 2 diabetic subjects lead to decreased fatty acid oxidation and increased lipogenesis; thiazolidinedione treatment reverses these defects", Diabetes. 2006 Aug;55(8):2277-85.
- Snell-Bergeon JK, Chartier-Logan C, Maahs DM, et al., "Adults with type 1 diabetes eat a high-fat atherogenic diet that is associated with coronary artery calcium", Diabetologia. 2009 May;52(5):801-9. doi: 10.1007/s00125-009-1280-4.
- Zhang L, Keung W, Samokhvalov V, Wang W, Lopaschuk GD, "Role of fatty acid uptake and fatty acid beta-oxidation in mediating insulin resistance in heart and skeletal muscle", Biochim Biophys Acta. 2010 Jan;1801(1):1-22.
- Sun D, Kintner D, Fitzpatrick JH, Emoto SE, Braquet PG, Bazan NG, Gilboe DD, "The effect of a free radical scavenger and platelet-activating factor antagonist on FFA accumulation in post-ischemic canine brain", Neurochem Res. 1994 Apr;19(4):525-8.
- Wang YX, Li Y, Sun AM, Wang FJ, Yu GP, "Hypolipidemic and antioxidative effects of aqueous enzymatic extract from rice bran in rats fed a high-fat and -cholesterol diet", Nutrients. 2014 Sep 16;6(9):3696-710. doi: 10.3390/nu6093696.
- Moraes JC, Coope A, Morari J, et al., "High-fat diet induces apoptosis of hypothalamic neurons", PLoS One. 2009;4(4):e5045. doi: 10.1371/journal.pone.0005045. Epub 2009 Apr 2.
- Thaler JP, Schwartz MW, "Minireview: Inflammation and obesity pathogenesis: the hypothalamus heats up", Endocrinology. 2010 Sep;151(9):4109-15. doi: 10.1210/en.2010-0336.
- Thaler JP, Yi CX, Schur EA, et al., "Obesity is associated with hypothalamic injury in rodents and humans", J Clin Invest. 2012 Jan 3;122(1):153-62. doi: 10.1172/JCI59660.
- Cannon WB, "The Wisdom Of The Body", 1939
- Selye H, "The Stress Of Life", Revised/Updated Edition, 1976
- Miles JM, Haymond MW, Gerich JE, "Effects of free fatty acids, insulin, glucagon and adrenaline on ketone body production in humans", Ciba Found Symp. 1982;87:192-213.
- Millet L, Barbe P, Lafontan M, Berlan M, Galitzky J, "Catecholamine effects on lipolysis and blood flow in human abdominal and femoral adipose tissue", J Appl Physiol (1985). 1998 Jul;85(1):181-8.
- de Glisezinski I, Larrouy D, Bajzova M, et al., "Adrenaline but not noradrenaline is a determinant of exercise-induced lipid mobilization in human subcutaneous adipose tissue", J Physiol. 2009 Jul 1;587(Pt 13):3393-404. doi: 10.1113/jphysiol.2009.168906.
- Bloom SR, Daniel PM, Johnston DI, Ogawa O, Pratt OE, "Release of glucagon, induced by stress", Q J Exp Physiol Cogn Med Sci. 1973 Jan;58(1):99-108.
- Iversen J, "Adrenergic receptors and the secretion of glucagon and insulin from the isolated, perfused canine pancreas", J Clin Invest. 1973 Sep;52(9):2102-16.
- Sonksen P, Sonksen J, "Insulin: understanding its action in health and disease", Br J Anaesth. 2000 Jul;85(1):69-79.
- Fanelli CG, De Feo P, Porcellati F, et al., "Adrenergic mechanisms contribute to the late phase of hypoglycemic glucose counterregulation in humans by stimulating lipolysis", J Clin Invest. 1992 Jun;89(6):2005-13.
- Fanelli C, Calderone S, Epifano L, et al., "Demonstration of a critical role for free fatty acids in mediating counterregulatory stimulation of gluconeogenesis and suppression of glucose utilization in humans", J Clin Invest. 1993 Oct;92(4):1617-22.
- Frayn KN, "The glucose-fatty acid cycle: a physiological perspective", Biochem Soc Trans. 2003 Dec;31(Pt 6):1115-9.
- Kashiwagi A, "Rationale and hurdles of inhibitors of hepatic gluconeogenesis in treatment of diabetes mellitus", Diabetes Res Clin Pract. 1995 Aug;28 Suppl:S195-200.
- Burcelin R, Eddouks M, Maury J, Kande J, Assan R, Girard J, "Excessive glucose production, rather than insulin resistance, accounts for hyperglycaemia in recent-onset streptozotocin-diabetic rats", Diabetologia. 1995 Mar;38(3):283-90.
- Delarue J, LeFoll C, Corporeau C, Lucas D, "N-3 long chain polyunsaturated fatty acids: a nutritional tool to prevent insulin resistance associated to type 2 diabetes and obesity?", Reprod Nutr Dev. 2004 May-Jun;44(3):289-99.
- McCarty MF, "Utility of metformin as an adjunct to hydroxycitrate/carnitine for reducing body fat in diabetics", Med Hypotheses. 1998 Nov;51(5):399-403.
- Widmaier EP, Plotsky PM, Sutton SW, Vale WW, "Regulation of corticotropin-releasing factor secretion in vitro by glucose", Am J Physiol. 1988 Sep;255(3 Pt 1):E287-92.
- Hall SE, Saunders J, Sönksen PH, "Glucose and free fatty acid turnover in normal subjects and in diabetic patients before and after insulin treatment", Diabetologia. 1979 May;16(5):297-306.
- McCarty MF, "Promotion of hepatic lipid oxidation and gluconeogenesis as a strategy for appetite control", Med Hypotheses. 1994 Apr;42(4):215-25.
- McCarty MF, "Inhibition of citrate lyase may aid aerobic endurance", Med Hypotheses. 1995 Sep;45(3):247-54.
- Peat R, “Diabetes, scleroderma, oils and hormones”, Ray Peat's Newsletter, www.raypeat.com, 2006
- Randle PJ, Garland PB, Hales CN, Newsholme EA, "The glucose fatty-acid cycle. Its role in insulin sensitivity and the metabolic disturbances of diabetes mellitus", Lancet. 1963 Apr 13;1(7285):785-9.
- Postgrad Med J., "Hormones and lipid metabolism", [No authors listed], 1972 Oct;48(564):616-25.
- Ferrannini E, Barrett EJ, Bevilacqua S, DeFronzo RA, "Effect of fatty acids on glucose production and utilization in man", J Clin Invest. 1983 Nov;72(5):1737-47.
- Golay A, Felber JP, Jallut D, Munger R, Ruiz J, Jéquier E, "Effect of lipid oxidation on the regulation of glucose utilization in obese patients", Acta Diabetol. 1995 Mar;32(1):44-8.
- Burns SF, Kelsey SF, Arslanian SA, "Effects of an intravenous lipid challenge and free fatty acid elevation on in vivo insulin sensitivity in African American versus Caucasian adolescents", Diabetes Care. 2009 Feb;32(2):355-60. doi: 10.2337/dc08-1102.
- Dirkx E, Schwenk RW, Glatz JF, Luiken JJ, van Eys GJ, "High fat diet induced diabetic cardiomyopathy", Prostaglandins Leukot Essent Fatty Acids. 2011 Nov;85(5):219-25. doi: 10.1016/j.plefa.2011.04.018.
- Grundleger ML, Thenen SW, "Decreased insulin binding, glucose transport, and glucose metabolism in soleus muscle of rats fed a high fat diet", Diabetes. 1982 Mar;31(3):232-7.
- Arslanian SA, Kalhan SC, "Correlations between fatty acid and glucose metabolism. Potential explanation of insulin resistance of puberty", Diabetes. 1994 Jul;43(7):908-14.
- Turcotte LP, Fisher JS, "Skeletal muscle insulin resistance: roles of fatty acid metabolism and exercise", Phys Ther. 2008 Nov;88(11):1279-96. doi: 10.2522/ptj.20080018.
- Hue L, Taegtmeyer H, "The Randle cycle revisited: a new head for an old hat", Am J Physiol Endocrinol Metab. 2009 Sep;297(3):E578-91.
- Bonen A, Tandon NN, Glatz JF, Luiken JJ, Heigenhauser GJ, "The fatty acid transporter FAT/CD36 is upregulated in subcutaneous and visceral adipose tissues in human obesity and type 2 diabetes", Int J Obes (Lond). 2006 Jun;30(6):877-83.
- Schwartz RS, Abraham S, "Regulation of mouse hepatic ATP-citrate lyase activity by dietary fat. Evidence for the presence of inactive enzyme", Biochim Biophys Acta. 1982 Jan 12;714(1):101-13.
- Hwang SG, Yano H, Kawashima R, "Influence of dietary medium- and long-chain triglycerides on fat deposition and lipogenic enzyme activities in rats", J Am Coll Nutr. 1993 Dec;12(6):643-50.
- Eder K, Kirchgessner M, "The effect of dietary vitamin E supply and a moderately oxidized oil on activities of hepatic lipogenic enzymes in rats", Lipids. 1998 Mar;33(3):277-83.
- Shimabukuro M, Zhou YT, Lee Y, Unger RH, "Troglitazone lowers islet fat and restores beta cell function of Zucker diabetic fatty rats", J Biol Chem. 1998 Feb 6;273(6):3547-50.
- Unger RH, "Lipotoxic diseases", Annu Rev Med. 2002;53:319-36.
- Joseph JW, Koshkin V, Saleh MC, et al., "Free fatty acid-induced beta-cell defects are dependent on uncoupling protein 2 expression", J Biol Chem. 2004 Dec 3;279(49):51049-56.
- Unger RH, Clark GO, Scherer PE, Orci L, "Lipid homeostasis, lipotoxicity and the metabolic syndrome", Biochim Biophys Acta. 2010 Mar;1801(3):209-14. doi: 10.1016/j.bbalip.2009.10.006. Epub 2009 Nov 27.
- Cnop M, Abdulkarim B, Bottu G, et al., "RNA sequencing identifies dysregulation of the human pancreatic islet transcriptome by the saturated fatty acid palmitate", Diabetes. 2014 Jun;63(6):1978-93. doi: 10.2337/db13-1383. Epub 2013 Dec 30.
- Cunha DA, Gurzov EN, Naamane N, et al., "JunB protects ß-cells from lipotoxicity via the XBP1-AKT pathway", Cell Death Differ. 2014 Aug;21(8):1313-24. doi: 10.1038/cdd.2014.53.
- Rorsman P, Braun M, "Regulation of insulin secretion in human pancreatic islets", Annu Rev Physiol. 2013;75:155-79. doi: 10.1146/annurev-physiol-030212-183754. Epub 2012 Sep 4.
- Schuit FC, Huypens P, Heimberg H, Pipeleers DG, "Glucose sensing in pancreatic beta-cells: a model for the study of other glucose-regulated cells in gut, pancreas, and hypothalamus", Diabetes. 2001 Jan;50(1):1-11.
- Sullivan C, Triscari J, "Metabolic regulation as a control for lipid disorders. I. Influence of (--)-hydroxycitrate on experimentally induced obesity in the rodent", Am J Clin Nutr. 1977 May;30(5):767-76.
- Heymsfield SB, Allison DB, Vasselli JR, Pietrobelli A, Greenfield D, Nunez C, "Garcinia cambogia (hydroxycitric acid) as a potential antiobesity agent: a randomized controlled trial", JAMA. 1998 Nov 11;280(18):1596-600.
- Preuss HG, Rao CV, Garis R, Bramble JD, Ohia SE, Bagchi M, Bagchi D, "An overview of the safety and efficacy of a novel, natural(-)-hydroxycitric acid extract (HCA-SX) for weight management", J Med. 2004;35(1-6):33-48.
- Márquez F, Babio N, Bulló M, Salas-Salvadó J, "Evaluation of the safety and efficacy of hydroxycitric acid or Garcinia cambogia extracts in humans", Crit Rev Food Sci Nutr. 2012;52(7):585-94.
- Ishihara K, Oyaizu S, Onuki K, Lim K, Fushiki T, "Chronic (-)-hydroxycitrate administration spares carbohydrate utilization and promotes lipid oxidation during exercise in mice", J Nutr. 2000 Dec;130(12):2990-5.
- Downs BW, Bagchi M, Subbaraju GV, Shara MA, Preuss HG, Bagchi D, "Bioefficacy of a novel calcium-potassium salt of (-)-hydroxycitric acid", Mutat Res. 2005 Nov 11;579(1-2):149-62.
- Cheng IS, Huang SW, Lu HC, Wu CL, Chu YC, Lee SD, Huang CY, Kuo CH, "Oral hydroxycitrate supplementation enhances glycogen synthesis in exercised human skeletal muscle", Br J Nutr. 2012 Apr;107(7):1048-55.
- Brownlee M, "Biochemistry and molecular cell biology of diabetic complications", Nature. 2001 Dec 13;414(6865):813-20.
- Ford ES, Giles WH, Dietz WH, "Prevalence of the metabolic syndrome among US adults: findings from the third National Health and Nutrition Examination Survey", JAMA. 2002 Jan 16;287(3):356-9.
- Israël M, Schwartz L, "The metabolic advantage of tumor cells", Mol Cancer. 2011 Jun 7;10:70. doi: 10.1186/1476-4598-10-70.
- Li J, O W, Li W, Jiang ZG1, Ghanbari HA, "Oxidative stress and neurodegenerative disorders", Int J Mol Sci. 2013 Dec 16;14(12):24438-75. doi: 10.3390/ijms141224438.
- Kanter JE, Bornfeldt KE, "Inflammation and diabetes-accelerated atherosclerosis: myeloid cell mediators", Trends Endocrinol Metab. 2013 Mar;24(3):137-44. doi: 10.1016/j.tem.2012.10.002. Epub 2012 Nov 13.
- Bornfeldt KE, "2013 Russell Ross memorial lecture in vascular biology: cellular and molecular mechanisms of diabetes mellitus-accelerated atherosclerosis", Arterioscler Thromb Vasc Biol. 2014 Apr;34(4):705-14. doi: 10.1161/ATVBAHA.113.301928.
- Zhou YP, Grill VE, "Long-term exposure of rat pancreatic islets to fatty acids inhibits glucose-induced insulin secretion and biosynthesis through a glucose fatty acid cycle", J Clin Invest. 1994 Feb;93(2):870-6.
- Foster DW, McGarry JD, "The regulation of ketogenesis", Ciba Found Symp. 1982;87:120-31.
- Corkey BE, Deeney JT, Yaney GC, Tornheim K, Prentki M, "The role of long-chain fatty acyl-CoA esters in beta-cell signal transduction", J Nutr. 2000 Feb;130(2S Suppl):299S-304S.
- Randle PJ, "Regulatory interactions between lipids and carbohydrates: the glucose fatty acid cycle after 35 years", Diabetes Metab Rev. 1998 Dec;14(4):263-83.
- Girard J, "Fatty acids and beta cells", [Article in French], Diabetes Metab. 2000 Jun;26 Suppl 3:6-9.
- Greenough WB 3rd, Crespin SR, Steinberg D, "Hypoglycaemia and hyperinsulinaemia in response to raised free-fatty-acid levels", Lancet. 1967 Dec 23;2(7530):1334-6.
- Kusminski CM, Shetty S, Orci L, Unger RH, Scherer PE, "Diabetes and apoptosis: lipotoxicity", Apoptosis. 2009 Dec;14(12):1484-95. doi: 10.1007/s10495-009-0352-8.
- Frohnert BI, Jacobs DR Jr, Steinberger J, Moran A, Steffen LM, Sinaiko AR, "Relation between serum free fatty acids and adiposity, insulin resistance, and cardiovascular risk factors from adolescence to adulthood", Diabetes. 2013 Sep;62(9):3163-9. doi: 10.2337/db12-1122.
- Nagalski A, Bryla J, "Niacin in therapy", [Article in Polish], Postepy Hig Med Dosw (Online). 2007 May 15;61:288-302.
- Copp EF, "Effects Of Insulin Treatment On Experimental Diabetes Of Dogs", Cal West Med. 1926 May;24(5):618-21.
- Robertson RP, Harmon J, Tran PO, Poitout V, "Beta-cell glucose toxicity, lipotoxicity, and chronic oxidative stress in type 2 diabetes", Diabetes. 2004 Feb;53 Suppl 1:S119-24.
- Endemann G, Brunengraber H, "The source of acetyl coenzyme A for acetylcholine synthesis in the perfused rat phrenic nerve-hemidiaphragm", J Biol Chem. 1980 Dec 10;255(23):11091-3.
- Leray V, Dumon H, Martin L, Siliart B, Sergheraert R, Biourge V, Nguyen P, "No effect of conjugated linoleic acid or Garcinia cambogia on fat-free mass, and energy expenditure in normal cats", J Nutr. 2006 Jul;136(7 Suppl):1982S-1984S.
- Amin KA, Kamel HH, Abd Eltawab MA, "The relation of high fat diet, metabolic disturbances and brain oxidative dysfunction: modulation by hydroxy citric acid", Lipids Health Dis. 2011 May 14;10:74. doi: 10.1186/1476-511X-10-74.
- Vasques CA, Schneider R, Klein-Júnior LC, Falavigna A, Piazza I, Rossetto S, "Hypolipemic Effect of Garcinia cambogia in Obese Women", Phytother Res. 2014 Jun;28(6):887-91. doi: 10.1002/ptr.5076. Epub 2013 Oct 17.
- Peskin BS, Sim D, Carter MJ, "The Failure of Vytorin and Statins to Improve Cardiovascular Health: Bad Cholesterol or Bad Theory?", Journal of American Physicians and Surgeons (J Am Phys Surg), Vol. 9, No. 3, Pp. 82-87, Fall 2008
- Yoseph J, Yoseph H, "How Statin Drugs Really Lower Cholesterol and Kill You One Cell at a Time", 2012
- Report of the Committee of Principal Investigators, “W.H.O. cooperative trial on primary prevention of ischaemic heart disease using clofibrate to lower serum cholesterol: mortality follow-up”, Lancet. 1980 Aug 23;2(8191):379-85.
- Report of the Committee of Principal Investigators, “WHO cooperative trial on primary prevention of ischaemic heart disease with clofibrate to lower serum cholesterol: final mortality follow-up”, Lancet. 1984 Sep 15;2(8403):600-4.
- Kaplan NM, “Lipid intervention trials in primary prevention: a critical review”, Clin Exp Hypertens A. 1992;14(1-2):109-18.
- Ravnskov U, "The Cholesterol Myths: Exposing the Fallacy that Saturated Fat and Cholesterol Cause Heart Disease", 2000
- LaRosa JC, Grundy SM, Waters DD, et al., “Intensive lipid lowering with atorvastatin in patients with stable coronary disease”, N Engl J Med. 2005 Apr 7;352(14):1425-35.
- Graveline D, "Statin Drugs Side Effects and the Misguided War on Cholesterol", 2004
- Kauffman JM, "Bias in recent papers on diets and drugs in peer-reviewed medical journals", Journal of American Physicians and Surgeons (J Am Phys Surg), Vol. 9, No. 1, Pp. 11-14, Spring 2004
- Kauffman JM, ''Malignant Medical Myths: Why Medical Treatment Causes 200,000 Deaths in the USA each Year, and How to Protect Yourself", 2006
- Kendrick M, "The Great Cholesterol Con", 2008
- Alsheikh-Ali AA, Maddukuri PV, Han H, Karas RH, "Effect of the magnitude of lipid lowering on risk of elevated liver enzymes, rhabdomyolysis, and cancer: insights from large randomized statin trials", J Am Coll Cardiol. 2007 Jul 31;50(5):409-18.
- Nago N, Ishikawa S, Goto T, Kayaba K, "Low cholesterol is associated with mortality from stroke, heart disease, and cancer: the Jichi Medical School Cohort Study", J Epidemiol. 2011;21(1):67-74. Epub 2010 Dec 11.
- Cabrera MA, de Andrade SM, Dip RM, "Lipids and all-cause mortality among older adults: a 12-year follow-up study", ScientificWorldJournal. 2012;2012:930139. doi: 10.1100/2012/930139.
- de Lorgeril M, "Cholesterol and statins: Sham science and bad medicine", Kindle Edition, 2014
- Marshall TM, "New Insights into the Statin-Cholesterol Controversy", Journal of American Physicians and Surgeons (J Am Phys Surg), Vol. 9, No. 2, Pp. 42-46, Summer 2014
- Ravnskov U, Rosch PJ, McCully KS, "Statins Do Not Protect Against Cancer: Quite the Opposite", J Clin Oncol. 2015 Jan 20. pii: JCO.2014.58.9564. [Epub ahead of print]
- Diamond DM, Ravnskov U, "How statistical deception created the appearance that statins are safe and effective in primary and secondary prevention of cardiovascular disease", Expert Rev Clin Pharmacol. 2015 Mar;8(2):201-10. doi: 10.1586/17512433.2015.1012494.
- Canner PL, Berge KG, Wenger NK, Stamler J, Friedman L, Prineas RJ, Friedewald W, "Fifteen year mortality in Coronary Drug Project patients: long- term benefit with niacin", J Am Coll Cardiol. 1986 Dec;8(6):1245-55.
- Hoffer A, "Vitamin B3: Niacin and its Amide", Townsend Letter for Doctors & Patients, www.townsendletter.com, Issue No. 147, Pp. 30-39, 1995
- Sampson UK, Linton MF, Fazio S, "Are statins diabetogenic?", Curr Opin Cardiol. 2011 Jul;26(4):342-7. doi: 10.1097/HCO.0b013e3283470359.
- Feingold KR, Funk JL, Moser AH, Shigenaga JK, Rapp JH, Grunfeld C, "Role for circulating lipoproteins in protection from endotoxin toxicity", Infect Immun. 1995 May;63(5):2041-6.
- Colpo A, "LDL cholesterol: "bad" cholesterol, or bad science?", J Am Phys Surg. 2005;10:83-89.
- Nakata M, Uto N, Maruyama I, Yada T, "Nitric oxide induces apoptosis via Ca2+-dependent processes in the pancreatic beta-cell line MIN6", Cell Struct Funct. 1999 Dec;24(6):451-5.
- Donath MY, Böni-Schnetzler M, Ellingsgaard H, Ehses JA, "Islet inflammation impairs the pancreatic beta-cell in type 2 diabetes", Physiology (Bethesda). 2009 Dec;24:325-31. doi: 10.1152/physiol.00032.2009.
- Kruit JK, Kremer PH, Dai L, et al., "Cholesterol efflux via ATP-binding cassette transporter A1 (ABCA1) and cholesterol uptake via the LDL receptor influences cholesterol-induced impairment of beta cell function in mice", Diabetologia. 2010 Jun;53(6):1110-9. doi: 10.1007/s00125-010-1691-2.
- Langhi C, Cariou B, "Cholesterol metabolism and beta-cell function", [Article in French], Med Sci (Paris). 2010 Apr;26(4):385-90. doi: 10.1051/medsci/2010264385.
- Carter AA, Gomes T, Camacho X, Juurlink DN, Shah BR, Mamdani MM, "Risk of incident diabetes among patients treated with statins: population based study", BMJ. 2013 May 23;346:f2610. doi: 10.1136/bmj.f2610.
- Kruit JK, Brunham LR, Verchere CB, Hayden MR, "HDL and LDL cholesterol significantly influence beta-cell function in type 2 diabetes mellitus", Curr Opin Lipidol. 2010 Jun;21(3):178-85. doi: 10.1097/MOL.0b013e328339387b.
- Hoffer A, Saul A, Foster HD, "Niacin: The Real Story", 2012
- Asghar M, Monjok E, Kouamou G, Ohia SE, Bagchi D, Lokhandwala MF, "Super CitriMax (HCA-SX) attenuates increases in oxidative stress, inflammation, insulin resistance, and body weight in developing obese Zucker rats", Mol Cell Biochem. 2007 Oct;304(1-2):93-9.
- Mukherjee R, Criddle DN, Gukovskaya A, Pandol S, Petersen OH, Sutton R, "Mitochondrial injury in pancreatitis", Cell Calcium. 2008 Jul;44(1):14-23. doi: 10.1016/j.ceca.2007.11.013.
- Krüger K, Mooren FC, "Exercise-induced leukocyte apoptosis", Exerc Immunol Rev. 2014;20:117-34.
- Roma LP, Bosqueiro JR, Cunha DA, et al., "Protection of insulin-producing cells against toxicity of dexamethasone by catalase overexpression", Free Radic Biol Med. 2009 Nov 15;47(10):1386-93. doi: 10.1016/j.freeradbiomed.2009.08.010.
- Logue SE, Martin SJ, "Caspase activation cascades in apoptosis", Biochem Soc Trans. 2008 Feb;36(Pt 1):1-9. doi: 10.1042/BST0360001.
- Berne C, "Nicotinamide adenine dinucleotide phosphate-converting enzymes and adenosine triphosphate citrate lyase in some tissues and organs of New Zealand obese mice with special reference to the enzyme pattern of the pancreatic islets", J Histochem Cytochem. 1975 Sep;23(9):660-5.
- MacDonald MJ, Longacre MJ, Langberg EC, et al., "Decreased levels of metabolic enzymes in pancreatic islets of patients with type 2 diabetes", Diabetologia. 2009 Jun;52(6):1087-91. doi: 10.1007/s00125-009-1319-6.
- Hanai J, Doro N, Sasaki AT, Kobayashi S, Cantley LC, Seth P, Sukhatme VP, "Inhibition of lung cancer growth: ATP citrate lyase knockdown and statin treatment leads to dual blockade of mitogen-activated protein kinase (MAPK) and phosphatidylinositol-3-kinase (PI3K)/AKT pathways", J Cell Physiol. 2012 Apr;227(4):1709-20. doi: 10.1002/jcp.22895.
- Tiedge M, Lortz S, Drinkgern J, Lenzen S, "Relation between antioxidant enzyme gene expression and antioxidative defense status of insulin-producing cells", Diabetes. 1997 Nov;46(11):1733-42.
- Cnop M, Hannaert JC, Hoorens A, Eizirik DL, Pipeleers DG, "Inverse relationship between cytotoxicity of free fatty acids in pancreatic islet cells and cellular triglyceride accumulation", Diabetes. 2001 Aug;50(8):1771-7.
- Ceriello A, Morocutti A, Mercuri F, Quagliaro L, Moro M, Damante G, Viberti GC, "Defective intracellular antioxidant enzyme production in type 1 diabetic patients with nephropathy", Diabetes. 2000 Dec;49(12):2170-7.
- Kornacker MS, Lowenstein JM, "Citrate and the conversion of carbohydrate into fat. Activities of citrate-cleavage enzyme and acetate thiokinase in livers of normal and diabetic rats", Biochem J. 1965 Jun;95:832-7.
- Fukuda H, Katsurada A, Iritani N, "Effects of nutrients and hormones on gene expression of ATP citrate-lyase in rat liver", Eur J Biochem. 1992 Oct 1;209(1):217-22.
- Hasan NM, Longacre MJ, Seed Ahmed M, et al., "Lower succinyl-CoA:3-ketoacid-CoA transferase (SCOT) and ATP citrate lyase in pancreatic islets of a rat model of type 2 diabetes: knockdown of SCOT inhibits insulin release in rat insulinoma cells", Arch Biochem Biophys. 2010 Jul;499(1-2):62-8. doi: 10.1016/j.abb.2010.05.007.
- Guo Z, Jiang H, Xu X, Duan W, Mattson MP, "Leptin-mediated cell survival signaling in hippocampal neurons mediated by JAK STAT3 and mitochondrial stabilization", J Biol Chem. 2008 Jan 18;283(3):1754-63.
- Montague CT, Farooqi IS, Whitehead JP, et al., "Congenital leptin deficiency is associated with severe early-onset obesity in humans", Nature. 1997 Jun 26;387(6636):903-8.
- Leroy P, Dessolin S, Villageois P, Moon BC, Friedman JM, Ailhaud G, Dani C, "Expression of ob gene in adipose cells. Regulation by insulin", J Biol Chem. 1996 Feb 2;271(5):2365-8.
- Bray GA, Greenway FL, "Pharmacological treatment of the overweight patient", Pharmacol Rev. 2007 Jun;59(2):151-84.
- Pelleymounter MA, Cullen MJ, Baker MB, Hecht R, Winters D, Boone T, Collins F, "Effects of the obese gene product on body weight regulation in ob/ob mice", Science. 1995 Jul 28;269(5223):540-3.
- Halaas JL, Gajiwala KS, Maffei M, et al., "Weight-reducing effects of the plasma protein encoded by the obese gene", Science. 1995 Jul 28;269(5223):543-6.
- Arch JR, "The discovery of drugs for obesity, the metabolic effects of leptin and variable receptor pharmacology: perspectives from beta3-adrenoceptor agonists", Naunyn Schmiedebergs Arch Pharmacol. 2008 Aug;378(2):225-40
- Borer KT, "Counterregulation of insulin by leptin as key component of autonomic regulation of body weight", World J Diabetes. 2014 Oct 15;5(5):606-29. doi: 10.4239/wjd.v5.i5.606.
- Beltowski J, Wójcicka G, Jamroz A, "Leptin decreases plasma paraoxonase 1 (PON1) activity and induces oxidative stress: the possible novel mechanism for proatherogenic effect of chronic hyperleptinemia", Atherosclerosis. 2003 Sep;170(1):21-9.
- Matarese G, "Leptin and the immune system: how nutritional status influences the immune response", Eur Cytokine Netw. 2000 Mar;11(1):7-14.
- Faggioni R, Feingold KR, Grunfeld C, "Leptin regulation of the immune response and the immunodeficiency of malnutrition", FASEB J. 2001 Dec;15(14):2565-71.
- Mancuso P, Gottschalk A, Phare SM, Peters-Golden M, Lukacs NW, Huffnagle GB, "Leptin-deficient mice exhibit impaired host defense in Gram-negative pneumonia", J Immunol. 2002 Apr 15;168(8):4018-24.
- Rosenbaum M, Leibel RL, "20 years of leptin: role of leptin in energy homeostasis in humans", J Endocrinol. 2014 Oct;223(1):T83-96. doi: 10.1530/JOE-14-0358.
- Sierra-Honigmann MR, Nath AK, Murakami C, et al., "Biological action of leptin as an angiogenic factor", Science. 1998 Sep 11;281(5383):1683-6.
- Bonior J, Jaworek J, Konturek SJ, Pawlik WW, "Leptin is the modulator of HSP60 gene expression in AR42J cells", J Physiol Pharmacol. 2006 Nov;57 Suppl 7:135-43.
- Islam MS, Morton NM, Hansson A, Emilsson V, "Rat insulinoma-derived pancreatic beta-cells express a functional leptin receptor that mediates a proliferative response", Biochem Biophys Res Commun. 1997 Sep 29;238(3):851-5.
- Chetboun M, Abitbol G, Rozenberg K, et al., "Maintenance of redox state and pancreatic beta-cell function: role of leptin and adiponectin", J Cell Biochem. 2012 Jun;113(6):1966-76. doi: 10.1002/jcb.24065.
- Bernal-Mizrachi E, Kulkarni RN, Scott DK, Mauvais-Jarvis F, Stewart AF, Garcia-Ocaña A, "Human ß-cell proliferation and intracellular signaling part 2: still driving in the dark without a road map", Diabetes. 2014 Mar;63(3):819-31. doi: 10.2337/db13-1146.
- Kamohara S, Burcelin R, Halaas JL, Friedman JM, Charron MJ, "Acute stimulation of glucose metabolism in mice by leptin treatment", Nature. 1997 Sep 25;389(6649):374-7.
- Koch C, Augustine RA, Steger J, et al., "Leptin rapidly improves glucose homeostasis in obese mice by increasing hypothalamic insulin sensitivity", J Neurosci. 2010 Dec 1;30(48):16180-7. doi: 10.1523/JNEUROSCI.3202-10.2010.
- Prentki M, Corkey BE, "Are the beta-cell signaling molecules malonyl-CoA and cystolic long-chain acyl-CoA implicated in multiple tissue defects of obesity and NIDDM?", Diabetes. 1996 Mar;45(3):273-83.
- Wang MY, Chen L, Clark GO, et al., "Leptin therapy in insulin-deficient type I diabetes", Proc Natl Acad Sci U S A. 2010 Mar 16;107(11):4813-9.
- Unger RH, Roth MG, "A New Biology of Diabetes Revealed by Leptin", Cell Metab. 2015 Jan 6;21(1):15-20. doi: 10.1016/j.cmet.2014.10.011. Epub 2014 Nov 20.
- Mueller WM, Gregoire FM, Stanhope KL, et al., "Evidence that glucose metabolism regulates leptin secretion from cultured rat adipocytes", Endocrinology. 1998 Feb;139(2):551-8.
- Havel PJ, "Role of adipose tissue in body-weight regulation: mechanisms regulating leptin production and energy balance", Proc Nutr Soc. 2000 Aug;59(3):359-71.
- Wellhoener P, Fruehwald-Schultes B, Kern W, et al., "Glucose metabolism rather than insulin is a main determinant of leptin secretion in humans", J Clin Endocrinol Metab. 2000 Mar;85(3):1267-71.
- Yannakoulia M, Yiannakouris N, Blüher S, Matalas AL, Klimis-Zacas D, Mantzoros CS, "Body fat mass and macronutrient intake in relation to circulating soluble leptin receptor, free leptin index, adiponectin, and resistin concentrations in healthy humans", J Clin Endocrinol Metab. 2003 Apr;88(4):1730-6.
- Levy JR, Stevens W, "Plasma hyperosmolality stimulates leptin secretion acutely by a vasopressin-adrenal mechanism", Am J Physiol Endocrinol Metab. 2004 Aug;287(2):E263-8.
- Friedman J, "20 years of leptin: leptin at 20: an overview", J Endocrinol. 2014 Oct;223(1):T1-8. doi: 10.1530/JOE-14-0405. Epub 2014 Aug 13.
- Moon HS, Matarese G, Brennan AM, et al., "Efficacy of metreleptin in obese patients with type 2 diabetes: cellular and molecular pathways underlying leptin tolerance", Diabetes. 2011 Jun;60(6):1647-56. doi: 10.2337/db10-1791.
- Sinha MK, Caro JF, "Clinical aspects of leptin", Vitam Horm. 1998;54:1-30.
- Caro JF, Kolaczynski JW, Nyce MR, et al., "Decreased cerebrospinal-fluid/serum leptin ratio in obesity: a possible mechanism for leptin resistance", Lancet. 1996 Jul 20;348(9021):159-61.
- Hayamizu K, Hirakawa H, Oikawa D, Nakanishi T, Takagi T, Tachibana T, Furuse M, "Effect of Garcinia cambogia extract on serum leptin and insulin in mice", Fitoterapia. 2003 Apr;74(3):267-73.
- Kim KY, Lee HN, Kim YJ, Park T, "Garcinia cambogia extract ameliorates visceral adiposity in C57BL/6J mice fed on a high-fat diet", Biosci Biotechnol Biochem. 2008 Jul;72(7):1772-80
- Brault M, Ray J, Gomez YH, Mantzoros CS, Daskalopoulou SS, "Statin treatment and new-onset diabetes: a review of proposed mechanisms", Metabolism. 2014 Jun;63(6):735-45. doi: 10.1016/j.metabol.2014.02.014.
- Söderberg S, Ahrén B, Jansson JH, Johnson O, Hallmans G, Asplund K, Olsson T, "Leptin is associated with increased risk of myocardial infarction", J Intern Med. 1999 Oct;246(4):409-18.
- Wallace AM, McMahon AD, Packard CJ, Kelly A, Shepherd J, Gaw A, Sattar N, "Plasma leptin and the risk of cardiovascular disease in the west of Scotland coronary prevention study (WOSCOPS)", Circulation. 2001 Dec 18;104(25):3052-6.
- Life Extension Foundation, "Disease Prevention And Treatment - Scientific Protocols That Integrate Mainstream And Alternative Medicine", Expanded 4th Edition, 2003
- Yamagishi SI, Edelstein D, Du XL, Kaneda Y, Guzmán M, Brownlee M, "Leptin induces mitochondrial superoxide production and monocyte chemoattractant protein-1 expression in aortic endothelial cells by increasing fatty acid oxidation via protein kinase A", J Biol Chem. 2001 Jul 6;276(27):25096-100.
- Maeso Fortuny MC, Brito Díaz B, Cabrera de León A, "Leptin, estrogens and cancer", Mini Rev Med Chem. 2006 Aug;6(8):897-907.
- Whitfield JF, "Parathyroid hormone and leptin--new peptides, expanding clinical prospects", Expert Opin Investig Drugs. 2005 Mar;14(3):251-64.
- Sundell J, Huupponen R, Raitakari OT, Nuutila P, Knuuti J, "High serum leptin is associated with attenuated coronary vasoreactivity", Obes Res. 2003 Jun;11(6):776-82.
- Gonzalez M, Lind L, Söderberg S, "Leptin and endothelial function in the elderly: the Prospective Investigation of the Vasculature in Uppsala Seniors (PIVUS) study", Atherosclerosis. 2013 Jun;228(2):485-90. doi: 10.1016/j.atherosclerosis.2013.03.018.
- Morioka T, Emoto M, Yamazaki Y, et al., "Leptin is associated with vascular endothelial function in overweight patients with type 2 diabetes", Cardiovasc Diabetol. 2014 Jan 10;13:10. doi: 10.1186/1475-2840-13-10.
- Purdham DM, Zou MX, Rajapurohitam V, Karmazyn M, "Rat heart is a site of leptin production and action", Am J Physiol Heart Circ Physiol. 2004 Dec;287(6):H2877-84. Epub 2004 Jul 29.
- Maffei M, Fei H, Lee GH, et al., "Increased expression in adipocytes of ob RNA in mice with lesions of the hypothalamus and with mutations at the db locus", Proc Natl Acad Sci U S A. 1995 Jul 18;92(15):6957-60.
- Knight ZA, Hannan KS, Greenberg ML, Friedman JM, "Hyperleptinemia is required for the development of leptin resistance", PLoS One. 2010 Jun 29;5(6):e11376. doi: 10.1371/journal.pone.0011376.
- Frühbeck G, Aguado M, Gómez-Ambrosi J, Martínez JA, "Lipolytic effect of in vivo leptin administration on adipocytes of lean and ob/ob mice, but not db/db mice", Biochem Biophys Res Commun. 1998 Sep 8;250(1):99-102.
- Frühbeck G, Gómez-Ambrosi J, "Modulation of the leptin-induced white adipose tissue lipolysis by nitric oxide", Cell Signal. 2001 Nov;13(11):827-33.
- Beltowski J, Wójcicka G, Jamroz A, "Stimulatory effect of leptin on nitric oxide production is impaired in dietary-induced obesity", Obes Res. 2003 Dec;11(12):1571-80.
- Commins SP, Watson PM, Padgett MA, Dudley A, Argyropoulos G, Gettys TW, "Induction of uncoupling protein expression in brown and white adipose tissue by leptin", Endocrinology. 1999 Jan;140(1):292-300.
- Commins SP, Watson PM, Frampton IC, Gettys TW, "Leptin selectively reduces white adipose tissue in mice via a UCP1-dependent mechanism in brown adipose tissue", Am J Physiol Endocrinol Metab. 2001 Feb;280(2):E372-7.
- Nedergaard J, Bengtsson T, Cannon B, "Unexpected evidence for active brown adipose tissue in adult humans", Am J Physiol Endocrinol Metab. 2007 Aug;293(2):E444-52.
- Asensio CS, Arsenijevic D, Lehr L, Giacobino JP, Muzzin P, Rohner-Jeanrenaud F, "Effects of leptin on energy metabolism in beta-less mice", Int J Obes (Lond). 2008 Jun;32(6):936-42. doi: 10.1038/ijo.2008.13.
- Lehr L, Canola K, Léger B, Giacobino JP, "Differentiation and characterization in primary culture of white adipose tissue brown adipocyte-like cells", Int J Obes (Lond). 2009 Jun;33(6):680-6
- Schulz TJ, Tseng YH, "Brown adipose tissue: development, metabolism and beyond", Biochem J. 2013 Jul 15;453(2):167-78. doi: 10.1042/BJ20130457.
- Cypess AM, Kahn CR, "The role and importance of brown adipose tissue in energy homeostasis", Curr Opin Pediatr. 2010 Aug;22(4):478-84. doi: 10.1097/MOP.0b013e32833a8d6e.
- Haas B, Schlinkert P, Mayer P, Eckstein N, "Targeting adipose tissue", Diabetol Metab Syndr. 2012 Oct 27;4(1):43. doi: 10.1186/1758-5996-4-43.
- Ricquier D, "To burn or to store", [Article in French], Ann Endocrinol (Paris). 2002 Dec;63(6 Pt 2):S7-14.
- Cinti S, "Between brown and white: novel aspects of adipocyte differentiation", Ann Med. 2011 Mar;43(2):104-15. doi: 10.3109/07853890.2010.535557.
- Keipert S, Jastroch M, "Brite/beige fat and UCP1 - is it thermogenesis?", Biochim Biophys Acta. 2014 Jul;1837(7):1075-82. doi: 10.1016/j.bbabio.2014.02.008
- Dodd GT, Decherf S, Loh K, et al., "Leptin and Insulin Act on POMC Neurons to Promote the Browning of White Fat", Cell. 2015 Jan 15;160(1-2):88-104. doi: 10.1016/j.cell.2014.12.022.
- Virtanen KA, Lidell ME, Orava J, et al., "Functional brown adipose tissue in healthy adults", N Engl J Med. 2009 Apr 9;360(15):1518-25. doi: 10.1056/NEJMoa0808949.
- Wu J, Cohen P, Spiegelman BM, "Adaptive thermogenesis in adipocytes: is beige the new brown?", Genes Dev. 2013 Feb 1;27(3):234-50. doi: 10.1101/gad.211649.112.
- Yo K, Yu YM, Zhao G, et al., "Brown adipose tissue and its modulation by a mitochondria-targeted peptide in rat burn injury-induced hypermetabolism", Am J Physiol Endocrinol Metab. 2013 Feb 15;304(4):E331-41. doi: 10.1152/ajpendo.00098.2012
- Bukowiecki LJ, Lupien J, Folléa N, Jahjah L, "Effects of sucrose, caffeine, and cola beverages on obesity, cold resistance, and adipose tissue cellularity", Am J Physiol. 1983 Apr;244(4):R500-7.
- Gordon RS Jr, Cherkes A, "Unesterified fatty acid in human blood plasma", J Clin Invest. 1956 Feb;35(2):206-12.
- Zhou Z, Yon Toh S, Chen Z, Guo K, Ng CP, Ponniah S, Lin SC, Hong W, Li P, "Cidea-deficient mice have lean phenotype and are resistant to obesity", Nat Genet. 2003 Sep;35(1):49-56.
- Hamann A, Flier JS, Lowell BB, "Obesity after genetic ablation of brown adipose tissue", Z Ernährungswiss. 1998;37 Suppl 1:1-7.
- Ishigaki Y, Katagiri H, Yamada T, et al., "Dissipating excess energy stored in the liver is a potential treatment strategy for diabetes associated with obesity", Diabetes. 2005 Feb;54(2):322-32.
- Cao L, Choi EY, Liu X, Martin A, Wang C, Xu X, During MJ, "White to brown fat phenotypic switch induced by genetic and environmental activation of a hypothalamic-adipocyte axis", Cell Metab. 2011 Sep 7;14(3):324-38. doi: 10.1016/j.cmet.2011.06.020.
- Vallerand AL, Lupien J, Bukowiecki LJ, "Cold exposure reverses the diabetogenic effects of high-fat feeding", Diabetes. 1986 Mar;35(3):329-34.
- Cypess AM, Lehman S, Williams G, et al., "Identification and importance of brown adipose tissue in adult humans", N Engl J Med. 2009 Apr 9;360(15):1509-17. doi: 10.1056/NEJMoa0810780.
- van Marken Lichtenbelt WD, Vanhommerig JW, Smulders NM, et al., "Cold-activated brown adipose tissue in healthy men", N Engl J Med. 2009 Apr 9;360(15):1500-8. doi: 10.1056/NEJMoa0808718.
- Ouellet V, Labbé SM, Blondin DP, et al., "Brown adipose tissue oxidative metabolism contributes to energy expenditure during acute cold exposure in humans", J Clin Invest. 2012 Feb 1;122(2):545-52. doi: 10.1172/JCI60433.
- Nübel T, Ricquier D, "Respiration under control of uncoupling proteins: Clinical perspective", Horm Res. 2006;65(6):300-10.
- Guerra C, Navarro P, Valverde AM, et al., "Brown adipose tissue-specific insulin receptor knockout shows diabetic phenotype without insulin resistance", J Clin Invest. 2001 Oct;108(8):1205-13.
- Shigemura N, Ohta R, Kusakabe Y, et al., "Leptin modulates behavioral responses to sweet substances by influencing peripheral taste structures", Endocrinology. 2004 Feb;145(2):839-47. Epub 2003 Oct 30.
- Yoshida R, Niki M, Jyotaki M, Sanematsu K, Shigemura N, Ninomiya Y, "Modulation of sweet responses of taste receptor cells", Semin Cell Dev Biol. 2013 Mar;24(3):226-31. doi: 10.1016/j.semcdb.2012.08.004. Epub 2012 Aug 25.
- Domingos AI, Vaynshteyn J, Sordillo A, Friedman JM, "The reward value of sucrose in leptin-deficient obese mice", Mol Metab. 2013 Dec 5;3(1):73-80. doi: 10.1016/j.molmet.2013.10.007. eCollection 2014.
- Wolfgang MJ, Cha SH, Sidhaye A, Chohnan S, Cline G, Shulman GI, Lane MD, "Regulation of hypothalamic malonyl-CoA by central glucose and leptin", Proc Natl Acad Sci U S A. 2007 Dec 4;104(49):19285-90.
- Brun T, Roche E, Assimacopoulos-Jeannet F, Corkey BE, Kim KH, Prentki M, "Evidence for an anaplerotic/malonyl-CoA pathway in pancreatic beta-cell nutrient signaling", Diabetes. 1996 Feb;45(2):190-8.
- Saha AK, Vavvas D, Kurowski TG, Apazidis A, Witters LA, Shafrir E, Ruderman NB, "Malonyl-CoA regulation in skeletal muscle: its link to cell citrate and the glucose-fatty acid cycle", Am J Physiol. 1997 Apr;272(4 Pt 1):E641-8.
- Poirier M, Vincent G, Reszko AE, et al., "Probing the link between citrate and malonyl-CoA in perfused rat hearts", Am J Physiol Heart Circ Physiol. 2002 Oct;283(4):H1379-86.
- McGarry JD, Foster DW, "Regulation of hepatic fatty acid oxidation and ketone body production", Annu Rev Biochem. 1980;49:395-420.
- Prentki M, Vischer S, Glennon MC, Regazzi R, Deeney JT, Corkey BE, "Malonyl-CoA and long chain acyl-CoA esters as metabolic coupling factors in nutrient-induced insulin secretion", J Biol Chem. 1992 Mar 25;267(9):5802-10.
- Ruderman NB, Saha AK, Vavvas D, Witters LA, "Malonyl-CoA, fuel sensing, and insulin resistance", Am J Physiol. 1999 Jan;276(1 Pt 1):E1-E18.
- Kelley DE, He J, Menshikova EV, Ritov VB, "Dysfunction of mitochondria in human skeletal muscle in type 2 diabetes", Diabetes. 2002 Oct;51(10):2944-50.
- Kikuchi H, Nanri A, Hori A, Sato M, Kawai K, Kasai H, Mizoue T, "Lower serum levels of total cholesterol are associated with higher urinary levels of 8-hydroxydeoxyguanosine", Nutr Metab (Lond). 2013 Oct 2;10(1):59. doi: 10.1186/1743-7075-10-59.
- Folmes CD, Lopaschuk GD, "Role of malonyl-CoA in heart disease and the hypothalamic control of obesity", Cardiovasc Res. 2007 Jan 15;73(2):278-87.
- Chen S, Ogawa A, Ohneda M, Unger RH, Foster DW, McGarry JD, "More direct evidence for a malonyl-CoA-carnitine palmitoyltransferase I interaction as a key event in pancreatic beta-cell signaling", Diabetes. 1994 Jul;43(7):878-83.
- Ishikawa M, Okajima F, Inoue N, et al., "Distinct effects of pravastatin, atorvastatin, and simvastatin on insulin secretion from a beta-cell line, MIN6 cells", J Atheroscler Thromb. 2006 Dec;13(6):329-35.
- Xia F, Xie L, Mihic A, et al., "Inhibition of cholesterol biosynthesis impairs insulin secretion and voltage-gated calcium channel function in pancreatic beta-cells", Endocrinology. 2008 Oct;149(10):5136-45. doi: 10.1210/en.2008-0161.
- Guay C, Madiraju SR, Aumais A, Joly E, Prentki M, "A role for ATP-citrate lyase, malic enzyme, and pyruvate/citrate cycling in glucose-induced insulin secretion", J Biol Chem. 2007 Dec 7;282(49):35657-65.
- Wellen KE, Hatzivassiliou G, Sachdeva UM, Bui TV, Cross JR, Thompson CB, "ATP-citrate lyase links cellular metabolism to histone acetylation", Science. 2009 May 22;324(5930):1076-80. doi: 10.1126/science.1164097.
- Gøtzsche PC, "Deadly Medicines and Organised Crime: How Big Pharma Has Corrupted Healthcare", 2013
- Kaiser T, Ewers H, Waltering A, Beckwermert D, Jennen C, Sawicki PT, "Sind Die Aussagen Medizinischer Werbeprospekte Korrekt?" [Article in German], Originalarbeit, www.arznei-telegramm.de, a-t 2004; 35: 21-3, 13-Feb-2004
- Sultan S, Hynes N, "The Ugly Side of Statins. Systemic Appraisal of the Contemporary Un-Known Unknowns," Open Journal of Endocrine and Metabolic Diseases, Vol. 3 No. 3, Pp. 179-185, 2013. doi: 10.4236/ojemd.2013.33025.
- Ridker PM, Danielson E, Fonseca FA, et al., "Rosuvastatin to prevent vascular events in men and women with elevated C-reactive protein", N Engl J Med. 2008 Nov 20;359(21):2195-207. doi: 10.1056/NEJMoa0807646.
- Sukhija R, Prayaga S, Marashdeh M, et al., "Effect of statins on fasting plasma glucose in diabetic and nondiabetic patients", J Investig Med. 2009 Mar;57(3):495-9. doi: 10.231/JIM.0b013e318197ec8b.
- Koh KK, Quon MJ, Han SH, Lee Y, Kim SJ, Shin EK, "Atorvastatin causes insulin resistance and increases ambient glycemia in hypercholesterolemic patients", J Am Coll Cardiol. 2010 Mar 23;55(12):1209-16.
- Mills EJ, Wu P, Chong G, et al., "Efficacy and safety of statin treatment for cardiovascular disease: a network meta-analysis of 170,255 patients from 76 randomized trials", QJM. 2011 Feb;104(2):109-24. doi: 10.1093/qjmed/hcq165. Epub 2010 Oct 7.
- Sattar N, Preiss D, Murray HM, et al., "Statins and risk of incident diabetes: a collaborative meta-analysis of randomised statin trials", Lancet. 2010 Feb 27;375(9716):735-42. doi: 10.1016/S0140-6736(09)61965-6.
- Preiss D, Sattar N, "Statins and the risk of new-onset diabetes: a review of recent evidence", Curr Opin Lipidol. 2011 Dec;22(6):460-6. doi: 10.1097/MOL.0b013e32834b4994.
- Culver AL, Ockene IS, Balasubramanian R, et al., "Statin use and risk of diabetes mellitus in postmenopausal women in the Women's Health Initiative", Arch Intern Med. 2012 Jan 23;172(2):144-52. doi: 10.1001/archinternmed.2011.625.
- Danaei G, García Rodríguez LA, Fernandez Cantero O, Hernán MA, "Statins and risk of diabetes: an analysis of electronic medical records to evaluate possible bias due to differential survival", Diabetes Care. 2013 May;36(5):1236-40. doi: 10.2337/dc12-1756. Epub 2012 Dec 17.
- Cederberg H, Stancáková A, Yaluri N, Modi S, Kuusisto J, Laakso M, "Increased risk of diabetes with statin treatment is associated with impaired insulin sensitivity and insulin secretion: a 6 year follow-up study of the METSIM cohort", Diabetologia. 2015 Mar 10. [Epub ahead of print]; DOI:10.1007/s00125-015-3528-5
- U.S. Food and Drug Administration (FDA), "FDA Drug Safety Communication: Important safety label changes to cholesterol-lowering statin drugs", www.fda.gov, 28-Feb-2012 [webpage accessed 11-March-2015]
- Siddals KW, Marshman E, Westwood M, Gibson JM, "Abrogation of insulin-like growth factor-I (IGF-I) and insulin action by mevalonic acid depletion: synergy between protein prenylation and receptor glycosylation pathways", J Biol Chem. 2004 Sep 10;279(37):38353-9.
- Canadian Diabetes Association Clinical Practice Guidelines Expert Committee, "2013 Clinical Practice Guidelines for the Prevention and Management of Diabetes in Canada", Can J Diabetes, Vol. 37, Suppl. 1, Pp. 1-227, April 2013
- Canadian Diabetes Association Clinical Practice Guidelines Expert Committee, Stone JA, Fitchett D, Grover S, Lewanczuk R, Lin P, "Vascular protection in people with diabetes", Can J Diabetes. 2013 Apr;37 Suppl 1:S100-4.
- Ravnskov U, "Ignore the Awkward! How the Cholesterol Myths Are Kept Alive", 2010
- Sayers G, "The adrenal cortex and homoestasis", Physiol Rev. 1950 Jul;30(3):241-320.
- Prescrire International (Journal), "Rosuvastatin for Cardiovascular Prevention: Too Many Uncertainties", [No authors listed], Vol. 18, No. 102, P. 176, Aug-2009
- Ravnskov U, McCully KS, "Review and Hypothesis: Vulnerable plaque formation from obstruction of Vasa vasorum by homocysteinylated and oxidized lipoprotein aggregates complexed with microbial remnants and LDL autoantibodies", Ann Clin Lab Sci. 2009 Winter;39(1):3-16.
- Dublin S, Jackson ML, Nelson JC, Weiss NS, Larson EB, Jackson LA, "Statin use and risk of community acquired pneumonia in older people: population based case-control study", BMJ. 2009 Jun 16;338:b2137. doi: 10.1136/bmj.b2137.
- Pfrieger FW, "Role of cholesterol in synapse formation and function", Biochim Biophys Acta. 2003 Mar 10;1610(2):271-80.
- Kim JE, Jeon SM, Park KH, et al., "Does Glycine max leaves or Garcinia Cambogia promote weight-loss or lower plasma cholesterol in overweight individuals: a randomized control trial", Nutr J. 2011 Sep 21;10:94. doi: 10.1186/1475-2891-10-94.
- Vasques CA, Rossetto S, Halmenschlager G, et al., "Evaluation of the pharmacotherapeutic efficacy of Garcinia cambogia plus Amorphophallus konjac for the treatment of obesity", Phytother Res. 2008 Sep;22(9):1135-40. doi: 10.1002/ptr.2323.
- Soni MG, Burdock GA, Preuss HG, Stohs SJ, Ohia SE, Bagchi D, "Safety assessment of (-)-hydroxycitric acid and Super CitriMax, a novel calcium/potassium salt", Food Chem Toxicol. 2004 Sep;42(9):1513-29.
- Preuss HG, Bagchi D, Bagchi M, Rao CV, Dey DK, Satyanarayana S, "Effects of a natural extract of (-)-hydroxycitric acid (HCA-SX) and a combination of HCA-SX plus niacin-bound chromium and Gymnema sylvestre extract on weight loss", Diabetes Obes Metab. 2004 May;6(3):171-80.
- Yada T, Nakata M, Shiraishi T, Kakei M, "Inhibition by simvastatin, but not pravastatin, of glucose-induced cytosolic Ca2+ signalling and insulin secretion due to blockade of L-type Ca2+ channels in rat islet beta-cells", Br J Pharmacol. 1999 Mar;126(5):1205-13.
- Ishikawa M, Namiki A, Kubota T, Yajima S, Fukazawa M, Moroi M, Sugi K, "Effect of pravastatin and atorvastatin on glucose metabolism in nondiabetic patients with hypercholesterolemia", Intern Med. 2006;45(2):51-5.
- Iwakura T, Fujimoto S, Kagimoto S, et al., "Sustained enhancement of Ca(2+) influx by glibenclamide induces apoptosis in RINm5F cells", Biochem Biophys Res Commun. 2000 May 10;271(2):422-8.
- Maedler K, Carr RD, Bosco D, Zuellig RA, Berney T, Donath MY, "Sulfonylurea induced beta-cell apoptosis in cultured human islets", J Clin Endocrinol Metab. 2005 Jan;90(1):501-6. Epub 2004 Oct 13.
- Ansar MM, Ansari M, "Nitric oxide involvement in pancreatic beta cell apoptosis by glibenclamide", Nitric Oxide. 2006 Feb;14(1):39-44. Epub 2005 Oct 26.
- Sawada F, Inoguchi T, Tsubouchi H, et al., "Differential effect of sulfonylureas on production of reactive oxygen species and apoptosis in cultured pancreatic beta-cell line, MIN6", Metabolism. 2008 Aug;57(8):1038-45. doi: 10.1016/j.metabol.2008.01.038.
- Kauffman JM, "Misleading Recent Papers on Statin Drugs in Peer-Reviewed Medical Journals", Journal of American Physicians and Surgeons (J Am Phys Surg), Vol. 12, No. 1, Pp. 7-9, Spring 2007
- Sirvent P, Fabre O, Bordenave S, Hillaire-Buys D, Raynaud De Mauverger E, Lacampagne A, Mercier J, "Muscle mitochondrial metabolism and calcium signaling impairment in patients treated with statins", Toxicol Appl Pharmacol. 2012 Mar 1;259(2):263-8
- Abdul-Ghaffar NU, el-Sonbaty MR, "Pancreatitis and rhabdomyolysis associated with lovastatin-gemfibrozil therapy", J Clin Gastroenterol. 1995 Dec;21(4):340-1.
- Sreenarasimhaiah J, Shiels P, Lisker-Melman M, "Multiorgan failure induced by atorvastatin", Am J Med. 2002 Sep;113(4):348-9.
- Singh S, Nautiyal A, Dolan JG, "Recurrent acute pancreatitis possibly induced by atorvastatin and rosuvastatin. Is statin induced pancreatitis a class effect?", JOP. 2004 Nov 10;5(6):502-4.
- Singh S, Loke YK, "Statins and pancreatitis: a systematic review of observational studies and spontaneous case reports", Drug Saf. 2006;29(12):1123-32.
- Finsterer J, "Pancreatitis as a manifestation of mitochondrial disorder", Am J Med Genet A. 2007 Mar 15;143A(6):632-3.
- Dehoney S, Wellein M, "Rhabdomyolysis associated with the nutritional supplement Hydroxycut", Am J Health Syst Pharm. 2009 Jan 15;66(2):142-8. doi: 10.2146/ajhp070640.
- Odinokova IV, Sung KF, Mareninova OA, Hermann K, Gukovsky I, Gukovskaya AS, "Mitochondrial mechanisms of death responses in pancreatitis", J Gastroenterol Hepatol. 2008 Mar;23 Suppl 1:S25-30.
- Langsjoen PH, Book Review of "How Statin Drugs Really Lower Cholesterol and Kill You One Cell at a Time" by James and Hannah Yoseph, Journal of American Physicians and Surgeons (J Am Phys Surg), Vol. 18, No. 1, Pp. 30, Spring 2013
- Bacon F, "Meditationes Sacrae: De Haeresibus" (Religious Meditations: Of Heresies), Essay, 1597 ["Knowledge is power" is a modified, more concise version of the original Latin sentence "Nam et ipsa scientia potestas est" (literal English translation: "For even knowledge itself is power") from that essay by Philosopher & Scientist Sir Francis Bacon (1561–1626)]
- Prosser H, Almond S, Walley T, "Influences on GPs' decision to prescribe new drugs-the importance of who says what", Fam Pract. 2003 Feb;20(1):61-8.
- Smith R, “The trouble with medical journals”, J R Soc Med., 2006 Mar;99(3):115-9
- Anchors M, "Medical Myths Doctors Believe", 2012
- Vreeman RC, Carroll AE, "Medical myths", BMJ. 2007 Dec 22;335(7633):1288-9.
- Sekimoto M, Imanaka Y, Kitano N, Ishizaki T, Takahashi O, "Why are physicians not persuaded by scientific evidence? A grounded theory interview study", BMC Health Serv Res. 2006 Jul 27;6:92.
- Tobin L, de Almedia Neto AC, Wutzke S, et al., "Influences on the prescribing of new drugs", Aust Fam Physician. 2008 Jan-Feb;37(1-2):78-80, 83.
- Liang BA, Mackey T, "Direct-to-consumer advertising with interactive internet media: global regulation and public health issues", JAMA. 2011 Feb 23;305(8):824-5. doi: 10.1001/jama.2011.203.
- Liang BA, Mackey T, "Prevalence and Global Health implications of social media in direct-to-consumer drug advertising", J Med Internet Res. 2011 Aug 31;13(3):e64. doi: 10.2196/jmir.1775.
- Wilkes MS, Doblin BH, Shapiro MF, "Pharmaceutical advertisements in leading medical journals: experts' assessments", Ann Intern Med. 1992 Jun 1;116(11):912-9.
- Villanueva P, Peiró S, Librero J, Pereiró I, "Accuracy of pharmaceutical advertisements in medical journals", Lancet. 2003 Jan 4;361(9351):27-32.
- Angell M, "The Truth About the Drug Companies: How They Deceive Us and What to Do About It", 2004
- Alasbali T, Smith M, Geffen N, et al., “Discrepancy between results and abstract conclusions in industry- vs nonindustry-funded studies comparing topical prostaglandins”, Am J Ophthalmol., 2009 Jan;147(1):33-38.e2. Epub 2008 Aug 30
- Psaty BM, Ray W, "FDA guidance on off-label promotion and the state of the literature from sponsors", JAMA. 2008 Apr 23;299(16):1949-51. doi: 10.1001/jama.299.16.1949.
- Othman N, Vitry A, Roughead EE, "Quality of pharmaceutical advertisements in medical journals: a systematic review", PLoS One. 2009 Jul 22;4(7):e6350. doi: 10.1371/journal.pone.0006350.
- Heimans L, van Hylckama Vlieg A, Dekker FW, "Are claims of advertisements in medical journals supported by RCTs?", Neth J Med. 2010 Jan;68(1):46-9.
- Roseman M, Milette K, Bero LA, et al., "Reporting of conflicts of interest in meta-analyses of trials of pharmacological treatments", JAMA. 2011 Mar 9;305(10):1008-17. doi: 10.1001/jama.2011.257.
- Prescrire International (Journal), "Medicines agencies too often under the influence of drug companies", [No authors listed], Vol. 20, No. 115, P. 108, April 2011
- Lenzer J, "Why we can't trust clinical guidelines", BMJ. 2013 Jun 14;346:f3830. doi: 10.1136/bmj.f3830.
- Gladsø KH, Garberg HR, Spigset O, Slørdal L, "Written pharmaceutical advertising - still unreliable?", [Article in Norwegian], Tidsskr Nor Laegeforen. 2014 Sep 2;134(16):1563-8. doi: 10.4045/tidsskr.13.1571. eCollection 2014.
- Kulkarni V, "Advertisements in medical journals", Indian J Dermatol Venereol Leprol. 2014 Mar-Apr;80(2):104-5. doi: 10.4103/0378-6323.129376.
- Seife C, "Research Misconduct Identified by the US Food and Drug Administration: Out of Sight, Out of Mind, Out of the Peer-Reviewed Literature", JAMA Intern Med. 2015 Feb 9. doi: 10.1001/jamainternmed.2014.7774. [Epub ahead of print]
- Avorn J, "Dangerous deception--hiding the evidence of adverse drug effects", N Engl J Med. 2006 Nov 23;355(21):2169-71.
- Campbell R, "Fear: Motivator or Depressant?", Orthomolecular Medicine News Service, Vol. 10, No. 16, 1-Oct-2014
- Krogsbøll LT, Jørgensen KJ, Grønhøj Larsen C, Gøtzsche PC, "General health checks in adults for reducing morbidity and mortality from disease", Cochrane Database Syst Rev. 2012 Oct 17;10:CD009009. doi: 10.1002/14651858.CD009009.pub2.
- Saquib N, Saquib J, Ioannidis JP, "Does screening for disease save lives in asymptomatic adults? Systematic review of meta-analyses and randomized trials", Int J Epidemiol. 2015 Feb;44(1):264-77. doi: 10.1093/ije/dyu140.
- Heleno B, Thomsen MF, Rodrigues DS, Jørgensen KJ, Brodrsen J, "Quantification of harms in cancer screening trials: literature review", BMJ. 2013 Sep 16;347:f5334. doi: 10.1136/bmj.f5334.
- Lobb A, "Science of weight loss supplements: compromised by conflicts of interest?", World J Gastroenterol. 2010 Oct 14;16(38):4880-2.
- Korownyk C, Kolber MR, McCormack J, et al., "Televised medical talk shows-what they recommend and the evidence to support their recommendations: a prospective observational study", BMJ. 2014 Dec 17;349:g7346. doi: 10.1136/bmj.g7346.
- Emerging Risk Factors Collaboration, Seshasai SR, Kaptoge S, et al., "Diabetes mellitus, fasting glucose, and risk of cause-specific death", N Engl J Med. 2011 Mar 3;364(9):829-41. doi: 10.1056/NEJMoa1008862.
- Katz NR, Giffhorn S, "Glucose- and insulin-independent induction of ATP citrate lyase in primary cultures of rat hepatocytes", Biochem J. 1983 Apr 15;212(1):65-71.
- Cani PD, Amar J, Iglesias MA, et al., "Metabolic endotoxemia initiates obesity and insulin resistance", Diabetes. 2007 Jul;56(7):1761-72.
- Cani PD, Bibiloni R, Knauf C, et al., "Changes in gut microbiota control metabolic endotoxemia-induced inflammation in high-fat diet-induced obesity and diabetes in mice", Diabetes. 2008 Jun;57(6):1470-81. doi: 10.2337/db07-1403.
- Li Y, Jiang L, Jia Z, et al., "A meta-analysis of red yeast rice: an effective and relatively safe alternative approach for dyslipidemia", PLoS One. 2014 Jun 4;9(6):e98611. doi: 10.1371/journal.pone.0098611. eCollection 2014.
- Kumari S, Sherriff JM, Spooner D, Beckett R, "Peripheral neuropathy induced by red yeast rice in a patient with a known small bowel gastrointestinal tumour", BMJ Case Rep. 2013 Apr 5;2013. pii: bcr2013009060. doi: 10.1136/bcr-2013-009060.
- Prescrire International (Journal), "Rhabdomyolysis linked to Chinese red yeast rice", [No authors listed], Vol. 17, No. 94, P. 64, Apr-2008
- Li Z, Seeram NP, Lee R, Thames G, Minutti C, Wang HJ, Heber D, "Plasma clearance of lovastatin versus chinese red yeast rice in healthy volunteers", J Altern Complement Med. 2005 Dec;11(6):1031-8.
- Smith DJ, Olive KE, "Chinese red rice-induced myopathy", South Med J. 2003 Dec;96(12):1265-7.
- Man RY, Lynn EG, Cheung F, Tsang PS, O K, "Cholestin inhibits cholesterol synthesis and secretion in hepatic cells (HepG2)", Mol Cell Biochem. 2002 Apr;233(1-2):153-8.
- Alternative Medicine Review, "Monograph. Monascus purpureus (red yeast rice)", [No authors listed], Vol. 9, No. 2, Pp. 208-10, June-2004
- Gruber HE, Watts JA, Riley FE, Fulkerson MB, Norton HJ, Hanley EN Jr, "Mitochondrial bioenergetics, mass, and morphology are altered in cells of the degenerating human annulus", J Orthop Res. 2013 Aug;31(8):1270-5. doi: 10.1002/jor.22361.
- Gruber HE, Watts JA, Hoelscher GL, et al., "Mitochondrial gene expression in the human annulus: in vivo data from annulus cells and selectively harvested senescent annulus cells", Spine J. 2011 Aug;11(8):782-91. doi: 10.1016/j.spinee.2011.06.012.
- Ravnskov U, McCully KS, Rosch PJ, "The statin-low cholesterol-cancer conundrum", QJM. 2012 Apr;105(4):383-8. doi: 10.1093/qjmed/hcr243. Epub 2011 Dec 8.
- Puri R, Nicholls SJ, Shao M, et al., "Impact of Statins on Serial Coronary Calcification During Atheroma Progression and Regression", J Am Coll Cardiol. 2015 Apr 7;65(13):1273-82. doi: 10.1016/j.jacc.2015.01.036.
- Holbrook A, Wright M, Sung M, Ribic C, Baker S, "Statin-associated rhabdomyolysis: is there a dose-response relationship?", Can J Cardiol. 2011 Mar-Apr;27(2):146-51. doi: 10.1016/j.cjca.2010.12.024.
- Manco M, Putignani L, Bottazzo GF, "Gut microbiota, lipopolysaccharides, and innate immunity in the pathogenesis of obesity and cardiovascular risk", Endocr Rev. 2010 Dec;31(6):817-44. doi: 10.1210/er.2009-0030.
- Joseph JW, Jensen MV, Ilkayeva O, et al., "The mitochondrial citrate/isocitrate carrier plays a regulatory role in glucose-stimulated insulin secretion", J Biol Chem. 2006 Nov 24;281(47):35624-32.
- Corkey BE, Glennon MC, Chen KS, Deeney JT, Matschinsky FM, Prentki M, "A role for malonyl-CoA in glucose-stimulated insulin secretion from clonal pancreatic beta-cells", J Biol Chem. 1989 Dec 25;264(36):21608-12.
- Lacasse JR, Leo J, "Serotonin and depression: a disconnect between the advertisements and the scientific literature", PLoS Med. 2005 Dec;2(12):e392.
- Hamazaki T, Okuyama H, Ogushi Y, Hama R, "Towards a Paradigm Shift in Cholesterol Treatment. A Re-examination of the Cholesterol Issue in Japan", Ann Nutr Metab. 2015;66 Suppl 4:1-116. doi: 10.1159/000381654. Epub 2015 Apr 29.
- Waters DD, Ho JE, DeMicco DA, et al., "Predictors of new-onset diabetes in patients treated with atorvastatin: results from 3 large randomized clinical trials", J Am Coll Cardiol. 2011 Apr 5;57(14):1535-45. doi: 10.1016/j.jacc.2010.10.047.
- Zaharan NL, Williams D, Bennett K, "Statins and risk of treated incident diabetes in a primary care population", Br J Clin Pharmacol. 2013 Apr;75(4):1118-24. doi: 10.1111/j.1365-2125.2012.04403.x.
- Mansi I, Frei CR, Wang CP, Mortensen EM, "Statins and New-Onset Diabetes Mellitus and Diabetic Complications: A Retrospective Cohort Study of US Healthy Adults", J Gen Intern Med. 2015 Apr 28. [Epub ahead of print]
- Miller DW, "Fallacies in Modern Medicine: Statins and the Cholesterol-Heart Hypothesis," Journal of American Physicians and Surgeons, Vol. 20, No. 2, Pp. 54-56, Summer 2015
- Szabó C, Salzman AL, "Endogenous peroxynitrite is involved in the inhibition of mitochondrial respiration in immuno-stimulated J774.2 macrophages", Biochem Biophys Res Commun. 1995 Apr 17;209(2):739-43.
- Szabó C, Zingarelli B, Salzman AL, "Role of poly-ADP ribosyltransferase activation in the vascular contractile and energetic failure elicited by exogenous and endogenous nitric oxide and peroxynitrite", Circ Res. 1996 Jun;78(6):1051-63.
- de Graaf L, Brouwers AH, Diemont WL, "Is decreased libido associated with the use of HMG-CoA-reductase inhibitors?", Br J Clin Pharmacol. 2004 Sep;58(3):326-8.
- Golomb BA, Koperski S, "Testosterone Change Relates to Lipid Change on Statins", Circulation. 2013;127:AMP17.
- Schooling CM, Au Yeung SL, Freeman G, Cowling BJ, "The effect of statins on testosterone in men and women, a systematic review and meta-analysis of randomized controlled trials", BMC Med. 2013 Feb 28;11:57. doi: 10.1186/1741-7015-11-57.
- Medras M, Kubicka E, Józkow P, et al., "Treatment with statins and testosterone levels in men", Endokrynol Pol. 2014;65(6):464-8. doi: 10.5603/EP.2014.0064.
- de Keyser CE, de Lima FV, de Jong FH, et al., "Use of statins is associated with lower serum total and non-sex hormone-binding globulin-bound testosterone levels in male participants of the Rotterdam Study", Eur J Endocrinol. 2015 Aug;173(2):155-65. doi: 10.1530/EJE-14-1061.
- Lundell D, "World Renown Heart Surgeon Speaks Out On What Really Causes Heart Disease", www.preventdisease.com, 1-March-2012
- Zhang Y, Gao Y, Tan A, et al., "Endogenous sex hormones and C-reactive protein in healthy Chinese men", Clin Endocrinol (Oxf). 2013 Jan;78(1):60-6. doi: 10.1111/j.1365-2265.2012.04359.x.
- Tsilidis KK, Rohrmann S, McGlynn KA, et al., "Association between endogenous sex steroid hormones and inflammatory biomarkers in US men", Andrology. 2013 Nov;1(6):919-28. doi: 10.1111/j.2047-2927.2013.00129.x.
- Laaksonen DE, Niskanen L, Punnonen K, et al., "Sex hormones, inflammation and the metabolic syndrome: a population-based study", Eur J Endocrinol. 2003 Dec;149(6):601-8.
- Vikan T, Schirmer H, Njølstad I, Svartberg J, "Low testosterone and sex hormone-binding globulin levels and high estradiol levels are independent predictors of type 2 diabetes in men", Eur J Endocrinol. 2010 Apr;162(4):747-54. doi: 10.1530/EJE-09-0943.
- Needham BL, Kim C, Mukherjee B, et al., "Endogenous sex steroid hormones and glucose in a South-Asian population without diabetes: the Metabolic Syndrome and Atherosclerosis in South-Asians Living in America pilot study", Diabet Med. 2015 Sep;32(9):1193-200. doi: 10.1111/dme.12642. Epub 2014 Dec 11.
- Wickramatilake CM, Mohideen MR, Pathirana C, "Association of metabolic syndrome with testosterone and inflammation in men", Ann Endocrinol (Paris). 2015 Jul;76(3):260-3. doi: 10.1016/j.ando.2015.04.008.
- Navarro G, Xu W, Jacobson DA, et al., "Extranuclear Actions of the Androgen Receptor Enhance Glucose-Stimulated Insulin Secretion in the Male", Cell Metab. 2016 Apr 26. pii: S1550-4131(16)30118-8. doi: 10.1016/j.cmet.2016.03.015. [Epub ahead of print]
- Okuyama H, Langsjoen PH, Hamazaki T, Ogushi Y, Hama R, Kobayashi T, Uchino H, "Statins stimulate atherosclerosis and heart failure: pharmacological mechanisms", Expert Rev Clin Pharmacol. 2015 Mar;8(2):189-99. doi: 10.1586/17512433.2015.1011125.
- Corey R, Werner KT, Singer A, et al., "Acute liver failure associated with Garcinia cambogia use", Ann Hepatol. 2016 Jan-Feb;15(1):123-6.
- Kim C, Prasad V, "Cancer Drugs Approved on the Basis of a Surrogate End Point and Subsequent Overall Survival: An Analysis of 5 Years of US Food and Drug Administration Approvals", JAMA Intern Med. 2015 Dec;175(12):1992-4. doi: 10.1001/jamainternmed.2015.5868.
- Brownstein D, "Drugs That Don't Work and Natural Therapies That Do", 2007
- Rovira-Llopis S, Bañuls C, de Marañon AM, et al., "Low testosterone levels are related to oxidative stress, mitochondrial dysfunction and altered subclinical atherosclerotic markers in type 2 diabetic male patients", Free Radic Biol Med. 2017 Mar 27;108:155-162. doi: 10.1016/j.freeradbiomed.2017.03.029. [Epub ahead of print]
- Olotu BS, Shepherd MD, Novak S, et al., “Use of Statins and the Risk of Incident Diabetes: A Retrospective Cohort Study”, Am J Cardiovasc Drugs. 2016 Oct;16(5):377-90. doi: 10.1007/s40256-016-0176-1.
- Jones M, Tett S, Peeters GM, Mishra GD, Dobson A, “New-Onset Diabetes After Statin Exposure in Elderly Women: The Australian Longitudinal Study on Women's Health”, Drugs Aging. 2017 Mar;34(3):203-209. doi: 10.1007/s40266-017-0435-0.
- Mansi IA, English JL, Morris MJ, et al., “Statins for primary prevention in physically active individuals: Do the risks outweigh the benefits?”, J Sci Med Sport. 2017 Jul;20(7):627-632. doi: 10.1016/j.jsams.2016.12.075.
- Ravnskov U, Diamond DM, Hama R, Hamazaki T, et al., “Lack of an association or an inverse association between low-density-lipoprotein cholesterol and mortality in the elderly: a systematic review”, BMJ Open. 2016 Jun 12;6(6):e010401. doi: 10.1136/bmjopen-2015-010401.
- DuBroff R, de Lorgeril M, “Cholesterol confusion and statin controversy”, World J Cardiol. 2015 Jul 26;7(7):404-9. doi: 10.4330/wjc.v7.i7.404.
- Diamond DM, Ravnskov U, “Additional commentary on deception in statin research”, Expert Rev Clin Pharmacol. 2015 Oct 23:1-2. doi: 10.1586/17512433.2015.1102009.
- Roberts WC, “Evaluating lipid-lowering trials in the twenty-first century”, Am J Cardiol. 2009 May 1;103(9):1325-8. doi: 10.1016/j.amjcard.2009.02.008.
- Prescrire International (Journal), "Statins in primary cardiovascular prevention. Little benefit, documented harms and many uncertainties regarding long-term use", Reviews, [No authors listed], Vol. 27, No. 195, Pp. 183-190, Jul-2018
- Sacks FM, Pfeffer MA, Moye LA, et al., “The effect of pravastatin on coronary events after myocardial infarction in patients with average cholesterol levels. Cholesterol and Recurrent Events Trial investigators”, N Engl J Med. 1996 Oct 3;335(14):1001-9.
- Cariou B, Goronflot T, Rimbert A, et al., “CORONADO Investigators. Routine Use Of Statins And Increased COVID-19 Related Mortality In Inpatients With Type 2 Diabetes: Results From The CORONADO Study”, Diabetes Metab. 2021 Mar;47(2):101202. doi: 10.1016/j.diabet.2020.10.001. Epub 2020 Oct 19. PMID: 33091555; PMCID: PMC7572108. [https://archive.is/evt3P; accessed 2-Aug-2021]
- Home ›
- Articles (List Of My Articles) ›
- Supplements Politics ›
- Do Garcinia Cambogia Side Effects Boost Diabetes?